Etiology & Risk Factors - Joint Under Siege
- Pathogens:
- Overall: Staphylococcus aureus (most common).
- Young, sexually active: Neisseria gonorrhoeae (📌 Mnemonic: "STD" - Synovitis, Tenosynovitis, Dermatitis).
- Neonates: Group B Strep, S. aureus, Gram-neg bacilli.
- IVDU, immunocompromised: Gram-neg bacilli (e.g., Pseudomonas), Candida.
- Sickle cell: Salmonella spp.
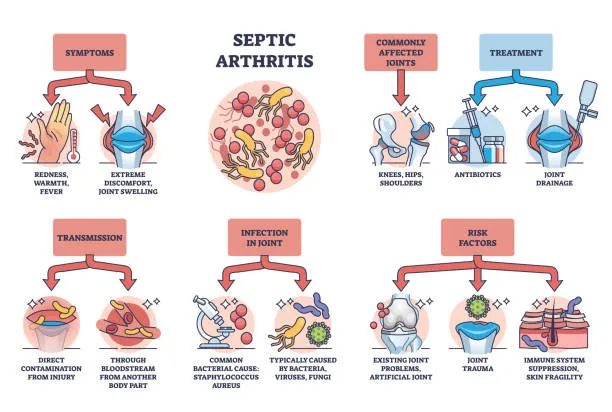
- Risk Factors:
- Damaged joints (RA, OA, gout).
- Prosthetic joints.
- IV drug use.
- Immunosuppression (DM, HIV, steroids).
- Age extremes.
- Joint surgery/injection.
- Skin infection, bacteremia.
⭐ S. aureus is the most common cause of septic arthritis in adults and children; N. gonorrhoeae in sexually active individuals.
Pathogenesis & Symptoms - Fiery Joint Drama
- Pathogenesis:
- Bacterial entry: Hematogenous (commonest), direct inoculation, contiguous spread.
- Synovial inflammation: Rapid bacterial proliferation → intense neutrophilic response → pus.
- Cartilage destruction: By bacterial toxins (e.g., PVL), host enzymes (MMPs, elastase), ↑ intra-articular pressure, inflammatory cytokines (TNF-α, IL-1β).
- Clinical Features (Fiery Joint):
- Acute onset: Severe pain (arthralgia), swelling (effusion), warmth, erythema.
- Restricted movement: Pseudoparalysis, pain on passive motion.
- Systemic: Fever, chills, malaise, tachycardia.
- 📌 Kocher's Criteria (pediatric septic hip):
- Fever > 38.5°C
- ESR > 40 mm/hr
- Non-weight bearing on affected side
- WBC count > 12,000/mm³
⭐ Irreversible cartilage damage can occur within 24-48 hours if untreated.
Diagnosis - Cracking Joint Case
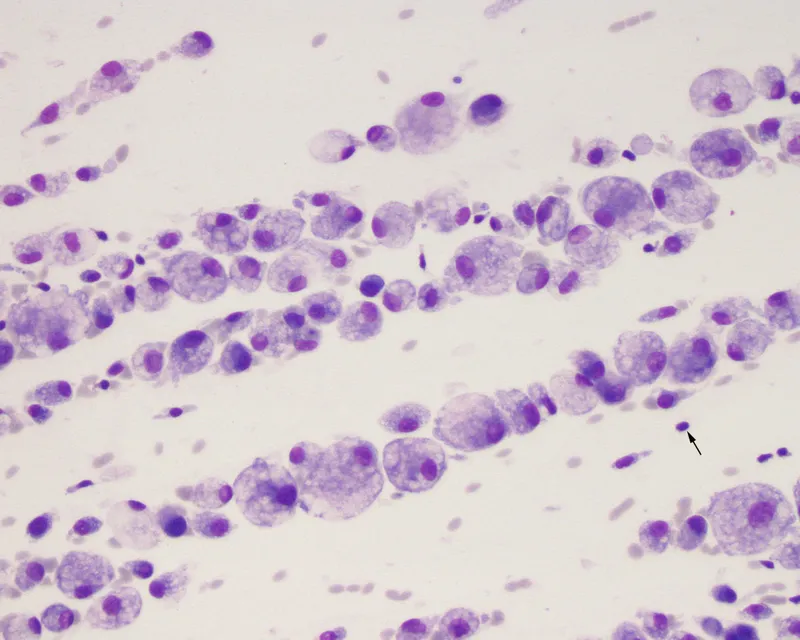
- Synovial Fluid Analysis (Arthrocentesis): KEY!
- Appearance: Turbid, purulent
- WBC: > 50,000/mm³
- PMN: > 75%
- Gram Stain & Culture: ~50-70% positive
- Crystals: Exclude gout/pseudogout
- Blood Tests:
- CBC: ↑WBC
- Inflammatory markers: ↑ESR (>30 mm/hr), ↑CRP
- Blood Culture: ~50% positive
- Imaging:
- X-ray: Early: normal/swelling. Late: joint narrowing, erosions.
- USG: Effusion detection, aspiration guidance.
- MRI: Most sensitive for early changes, osteomyelitis.
- Kocher's Criteria (Pediatric Hip): 📌 FEN-W
- Fever > 38.5°C
- Non-weight bearing
- ESR > 40 mm/hr
- WBC > 12,000/mm³
- (≥3 criteria suggest high risk)
⭐ Synovial fluid: WBC > 50,000/mm³ & PMNs > 75% strongly suggest septic arthritis, even with negative Gram stain.
Management & Complications - Dousing Joint Flames
- Immediate Goals:
- Eradicate infection: Prompt IV antibiotics (empiric → culture-guided).
- Remove pus: Urgent joint drainage.
- Pain relief & preserve function.
- Treatment Pillars:
- Antibiotics: IV for 2-4 weeks (e.g., Vancomycin + Ceftriaxone/Cefotaxime), then oral for 2-4 weeks. Total 4-6 weeks.
- Drainage:
- Needle aspiration (repeated).
- Arthroscopic lavage.
- Arthrotomy (hip, resistant cases).
- Supportive: Splinting, analgesia, later physiotherapy.
- Complications (If Delayed/Severe):
- Cartilage destruction → Degenerative Joint Disease (DJD).
- Osteomyelitis.
- Joint stiffness/ankylosis.
- Growth plate damage (children).
- Sepsis.
⭐ Failure to drain a septic joint within 24-48 hours can lead to irreversible cartilage loss.
High‑Yield Points - ⚡ Biggest Takeaways
- Most common organism: Staphylococcus aureus.
- Hematogenous spread is the predominant infection route.
- Knee is most affected in adults; hip in children.
- IV drug users: Suspect Pseudomonas aeruginosa, often in sacroiliac joints.
- Diagnosis: Synovial fluid with WBC >50,000/mm³, >75% PMNs, and positive culture.
- Treatment: Urgent IV antibiotics and joint drainage (arthrocentesis, arthroscopy, or arthrotomy).
- Kocher criteria (fever, non-weight bearing, ESR >40, WBC >12,000) aid pediatric septic hip diagnosis.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

