Breech Delivery - Bottoms Up Intro
- Definition: Longitudinal lie where fetal buttocks or lower limbs present at the pelvic inlet; sacrum is the fetal denominator.
- Incidence: 3-4% of all singleton deliveries at term.
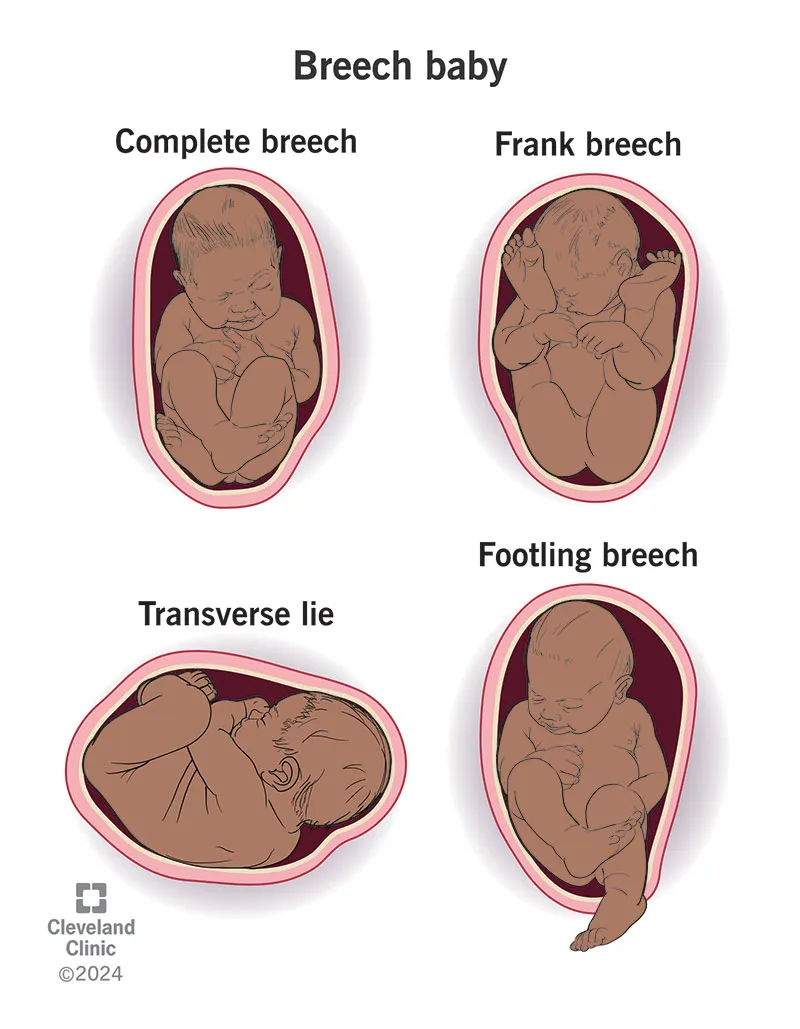
- Types:
- Frank Breech: Hips flexed, knees extended (like a pike dive).
⭐ Frank breech, with flexed hips and extended knees, is the most common type at term, accounting for approximately 65-70% of breech cases.
- Complete Breech: Hips flexed, knees flexed (fetal position).
- Incomplete Breech: One/both hips not fully flexed.
- Footling: One/both feet present below buttocks.
- Kneeling: One/both knees present below buttocks.
- Frank Breech: Hips flexed, knees extended (like a pike dive).
Breech Delivery - Why So Upside Down?
- Maternal Factors:
- Uterine: Anomalies (bicornuate, septate), fibroids.
- Pelvic: Contracted pelvis.
- Muscular: Lax abdominal/uterine walls (grand multiparity).
- Fetal Factors:
- Prematurity (most common).
- Multiple gestation.
- Anomalies: Hydrocephalus, anencephaly.
- Abnormal growth: Macrosomia, IUGR.
- Intrauterine Fetal Death (IUFD).
- Placental/Liquor Factors:
- Placenta: Placenta previa.
- Amniotic Fluid: Polyhydramnios (↑ fluid), oligohydramnios (↓ fluid, restricts turning).
- Cord: Short umbilical cord.
⭐ Prematurity is the single most common predisposing factor for breech presentation, as the fetus has more room to move and is less likely to have spontaneously turned to cephalic presentation.
Breech Delivery - Finding The Flip
- Clinical Diagnosis:
- Leopold's Maneuvers: Hard, round, ballotable head at fundus; softer, irregular breech at pelvis.
- Fetal Heart Sounds (FHS): Typically heard above the umbilicus.
- Vaginal Examination (during labor):
- Palpation of sacrum, ischial tuberosities, anus.
- Differentiate foot (calcaneum, toes of equal length) from hand (thumb, unequal fingers).
- Ultrasonography (USG):
- Confirmatory: Identifies type of breech (frank, complete, footling).
- Assesses: Estimated Fetal Weight (EFW), attitude, amniotic fluid, placental localization, congenital anomalies.

⭐ Ultrasonography (USG) is the gold standard for confirming breech presentation, accurately identifying the type of breech, fetal attitude, estimated fetal weight, and detecting any associated anomalies or placental issues.
Breech Delivery - The Exit Strategy
-
Antenatal: External Cephalic Version (ECV)
- Offered at 36-37 weeks (singleton).
- Contraindications: Absolute (e.g., APH, ROM, multiple gestation, fetal compromise), Relative (e.g., previous CS, IUGR, oligohydramnios).
-
Intrapartum: Mode of Delivery
> ⭐ The Term Breech Trial (Hannah et al., 2000) found planned CS ↓ perinatal mortality/morbidity for term singleton breech vs. planned VBD, significantly influencing practice.
-
Vaginal Breech Delivery (VBD) Criteria
- EFW 2.5-3.8 kg; Frank or complete type.
- No hyperextension of fetal head (flexed); Clinically adequate pelvis.
- Skilled team & Emergency CS facility; Informed consent.
-
Conduct of VBD (Assisted)
- Mechanisms: Standard sequence (engagement, descent, internal rotation, delivery).
- Maneuvers:
- Pinard's: For extended legs.
- Lovset's: For nuchal/extended arms.
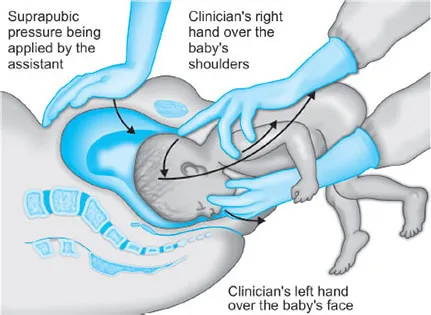
- Mauriceau-Smellie-Veit (MSV): For flexed aftercoming head.
- Piper's forceps: For controlled delivery of aftercoming head.
High‑Yield Points - ⚡ Biggest Takeaways
- Frank breech is the most common type; External Cephalic Version (ECV) can be attempted at 36-37 weeks.
- Prerequisites for vaginal breech delivery include estimated fetal weight 2.5-3.5 kg, flexed fetal head, and an adequate maternal pelvis.
- Key maneuvers include Pinard's (legs), Loveset's (shoulders), and Mauriceau-Smellie-Veit (aftercoming head).
- Major risks are head entrapment, birth asphyxia, and fetal trauma, especially in preterm breeches.
- Risk of cord prolapse is highest with footling or incomplete breech presentations.
- Elective Cesarean Section is often preferred to minimize neonatal morbidity, particularly in primigravidas or with other risk factors.
- Zavanelli maneuver is a last resort for an entrapped head, involving pushing the fetus back for CS delivery.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

