Vulvar Disorders: Anatomy & Exam - Basic Blueprint

- Anatomy:
- External: Mons pubis, labia majora & minora, clitoris.
- Labia details: Majora (outer, keratinized), minora (inner, non-keratinized).
- Vestibule: Medial to labia minora. Contains urethral/vaginal openings, Bartholin's (posterolateral), Skene's (paraurethral) gland ducts.
- Examination:
- Inspection: Visual check for lesions, erythema, edema, discharge, atrophy, pigmentation.
- Palpation: Check all areas for masses, tenderness, induration; assess Bartholin's glands.
⭐ Bartholin's glands: posterolateral in vestibule; ducts open at 5 & 7 o'clock positions.
Vulvar Disorders: NNEDV Spotlight - Itchy Vulva Woes
- Non-Neoplastic Epithelial Disorders of the Vulva (NNEDV): Key causes of chronic vulvar pruritus, pain, lesions.
- Lichen Sclerosus (LS):
- Most common; intense pruritus, dyspareunia.
- Appearance: Porcelain-white papules, "figure-of-eight" pattern. Atrophy.
- Biopsy: Thin epidermis, dermal homogenization.
- Management: High-potency topical steroids (e.g., clobetasol).
- Risk: ~5% SCC. 📌 LS can cause clitoral phimosis.
- Lichen Planus (LP):
- Affects vulva, vagina, oral mucosa (Wickham's striae).
- Erosive form: Painful, red erosions; vaginal synechiae/stenosis.
- Management: Topical/systemic corticosteroids.
- Risk: ↑ SCC.
- Lichen Simplex Chronicus (LSC):
- Secondary to chronic scratching (itch-scratch cycle).
- Appearance: Thickened, leathery skin (lichenification), excoriations.
- Management: Mid-potency topical steroids, break itch-scratch cycle.
⭐ Lichen Sclerosus is the most common dermatosis associated with vulvar squamous cell carcinoma.
Vulvar Disorders: Infections & Cysts - Unwanted Guests
- Infections:
- Candida albicans: Thick, white, curdy discharge; pruritus. Dx: KOH mount (pseudohyphae). Tx: Topical/oral antifungals (e.g., Clotrimazole, Fluconazole).
- Bacterial Vaginosis (BV): Thin, greyish-white, fishy odor discharge. Dx: Clue cells, Whiff test (+). Tx: Metronidazole, Clindamycin.
- Trichomonas vaginalis: Frothy, yellow-green, malodorous discharge; strawberry cervix. Dx: Wet mount (motile trichomonads). Tx: Metronidazole (treat partner).
- Herpes Simplex Virus (HSV): Painful vesicles/ulcers. Dx: Tzanck smear (multinucleated giant cells), PCR. Tx: Acyclovir.
- Human Papillomavirus (HPV): Condylomata acuminata (genital warts). Types 6, 11 most common. Tx: Podophyllin, Imiquimod, cryotherapy.
- Cysts:
- Bartholin's Cyst/Abscess: Obstruction of Bartholin's gland duct; posterolateral introitus. Tx: Marsupialization for recurrent cysts/abscesses.
- Skene's Gland Cyst: Paraurethral. Often asymptomatic.
- Epidermal Inclusion Cyst: Benign, from trapped keratin. Usually asymptomatic.
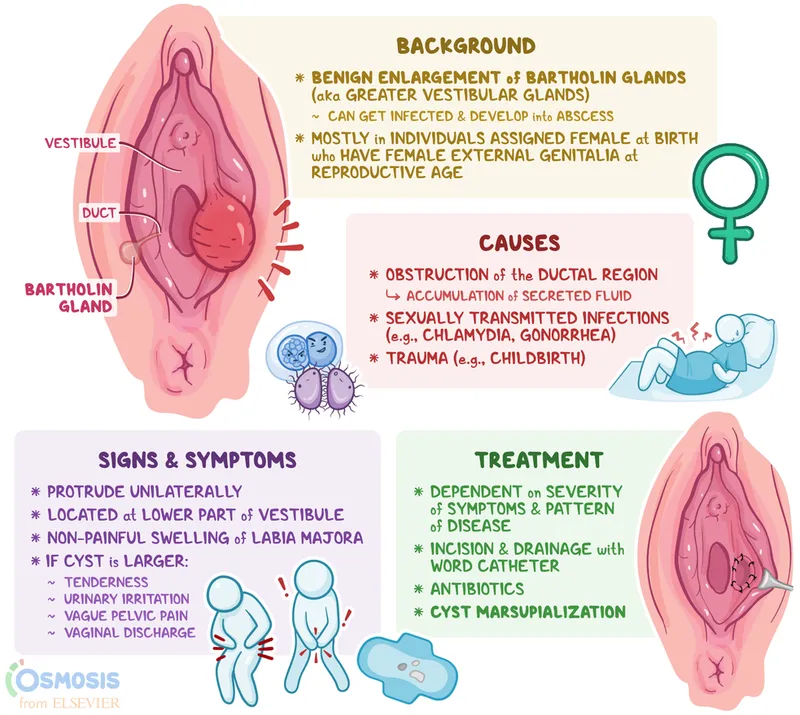
⭐ Bartholin's gland carcinoma, though rare (<1% of vulvar cancers), should be suspected in women >40 years with a new or enlarging Bartholin's gland mass, especially if solid or fixed. Biopsy is crucial.
📌 Bartholin's cyst = Back (posterior) and Big (can be).
Vulvar Disorders: Pain & VIN - Sensitive Signals
- Vulvodynia: Chronic vulvar pain > 3 months, no identifiable cause.
- Types:
- Generalized: Spontaneous or provoked.
- Localized (e.g., Vestibulodynia): Provoked by touch (e.g., intercourse). Positive Q-tip test.
- Rx: Multimodal: TCAs (amitriptyline), gabapentin, pelvic floor PT, topical lidocaine.
- Types:
- Vulvar Intraepithelial Neoplasia (VIN): Precursor to vulvar SCC.
- Sx: Persistent pruritus, visible lesion (white, red, pigmented, warty). May be asymptomatic.
- Dx: Biopsy of suspicious lesions is mandatory.
- Types:
- uVIN/HSIL: HPV-related (types 16, 18). Younger, multifocal. Rx: Excision, laser, imiquimod.
- dVIN: Non-HPV. Older, assoc. lichen sclerosus/p53. Unifocal. Rx: Wide local excision.
⭐ dVIN: older women, p53 mutation/lichen sclerosus-linked, higher & faster cancer progression risk vs. uVIN.
High‑Yield Points - ⚡ Biggest Takeaways
- Lichen sclerosus: "Cigarette paper" or parchment-like skin, figure-of-eight pattern; ↑ SCC risk. Biopsy crucial.
- Lichen planus: Violaceous, pruritic, polygonal papules (5 P's); Wickham's striae; oral lesions common; ↑ SCC risk.
- VIN (Vulvar Intraepithelial Neoplasia): Primarily HPV-related (types 16, 18); often asymptomatic or pruritic; precursor to SCC.
- Paget's disease of vulva: Fiery red, eczematoid, weeping lesion with pruritus; intraepithelial adenocarcinoma.
- Bartholin's gland cyst/abscess: Most common vulvar cystic mass; treat with I&D or Word catheter.
- Vulvodynia: Chronic vulvar pain (>3 months) without clear cause; diagnosis of exclusion.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

