Neisseria & Moraxella: Overview - Gram-Negative Diplococci Duo
- Core Identity: Aerobic, non-motile, Gram-negative cocci, typically in pairs (diplococci).
- Neisseria: Kidney-bean shaped.
- Moraxella: Often coccobacillary.
- Biochemistry: Oxidase positive (key). Catalase positive (most Neisseria, M. catarrhalis).
- Habitat: Human mucosal surfaces.
- Major Pathogens & Diseases:
- N. gonorrhoeae: Gonorrhea.
- N. meningitidis: Meningitis, meningococcemia.
- M. catarrhalis: Otitis media, sinusitis, bronchitis.
⭐ Pathogenic Neisseria (e.g., gonococcus, meningococcus) are typically cultured on Thayer-Martin agar, a selective enriched medium.
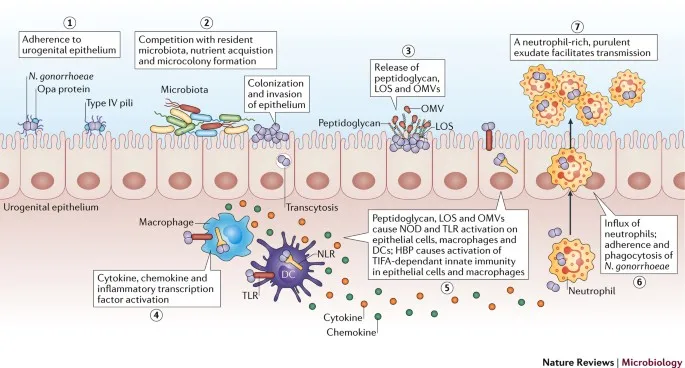
N. gonorrhoeae: Pathogenesis & Disease - The Clap Culprit
- Pathogenesis:
- Attachment/Invasion: Pili (Type IV, antigenic variation), Opa proteins (bind CEACAMs, invasion).
- Evasion: IgA1 protease, PorB (inhibits phagolysosome fusion), LOS (endotoxin, sialylation → serum resistance), antigenic/phase variation.
- Damage: LOS & peptidoglycan → TNF-α release → acute inflammation, neutrophil influx.
- Clinical Syndromes (The Clap):
- Males: Urethritis (purulent discharge, dysuria; incubation 2-7 days). Complications: epididymitis, prostatitis.
- Females: Cervicitis (often asymptomatic), PID (salpingitis, infertility, ectopic), Fitz-Hugh-Curtis syndrome.
- Neonates: Ophthalmia neonatorum (purulent conjunctivitis).
- Other Localized: Gonococcal pharyngitis, proctitis.
- Disseminated Gonococcal Infection (DGI): Arthritis-dermatitis syndrome (tenosynovitis, polyarthralgia, pustular skin lesions) or septic arthritis (monoarticular).
⭐ DGI risk ↑ in women (menses/pregnancy) & C5-C9 complement deficiencies.
- 📌 Pili, Opa, LOS, IgA protease: Core virulence.
N. meningitidis: Pathogenesis & Disease - The Meningitis Menace
- Transmission: Respiratory droplets; high risk in close contact settings (dorms, military barracks). 📌 "Close Contact Causes Meningitis."
- Key Virulence Factors:
- Polysaccharide capsule: Antiphagocytic; main virulence factor. Serogroups (A, B, C, Y, W-135) for vaccines.
- Pili (Fimbriae): Mediate attachment to nasopharyngeal epithelium.
- LOS (Lipooligosaccharide): Endotoxin → potent inflammatory mediator, septic shock, DIC.
- IgA1 protease: Cleaves IgA1, aids mucosal surface colonization.
- Pathogenesis:
- Clinical Syndromes:
- Meningitis: Most common. Acute onset: high fever, severe headache, stiff neck, altered mental status. Positive Kernig's/Brudzinski's signs.
- Meningococcemia (Sepsis): Life-threatening. Abrupt fever, chills, characteristic petechial or purpuric rash (non-blanching), hypotension. Rapidly progressive.
⭐ Waterhouse-Friderichsen syndrome: Fulminant, often fatal complication of meningococcemia, with bilateral adrenal hemorrhage, shock, DIC.

Moraxella & Commensal Neisseria - Other Oxidase Positives
- Moraxella catarrhalis
- Gram-negative diplococcus; aerobic
- Oxidase (+), Catalase (+), DNAse (+) (key: vs Neisseria)
- Asaccharolytic (no sugar fermentation)
- Normal URT flora
- Causes: Otitis media, sinusitis, bronchitis, pneumonia (esp. COPD)
- Most produce β-lactamase (penicillin-resistant)
- 📌 Mnemonic: Moraxella Catarrhalis causes Mucous Catarrh (bronchitis, sinusitis)
- Commensal Neisseria (e.g., N. sicca, N. lactamica, N. subflava)
- Gram-negative diplococci; normal URT flora
- Oxidase (+)
- Generally non-pathogenic; can cause opportunistic infections (e.g., endocarditis)
- Differentiate from pathogenic Neisseria: growth on nutrient agar at 22°C, some ferment lactose (N. lactamica).
⭐ Moraxella catarrhalis is characteristically DNAse positive and asaccharolytic, unlike pathogenic Neisseria species, and is a common cause of otitis media and COPD exacerbations.
High‑Yield Points - ⚡ Biggest Takeaways
- Neisseria: Gram-negative diplococci. N. gonorrhoeae (gonorrhea, Thayer-Martin, no maltose). N. meningitidis (meningitis, maltose+, capsule).
- M. catarrhalis: Gram-negative diplococcus; causes otitis media, sinusitis, COPD exacerbations; oxidase positive.
- Neisseria Virulence: Pili (adherence), IgA protease, LOS (endotoxin).
- N. meningitidis: Polysaccharide capsule (vaccine target, not B); Waterhouse-Friderichsen syndrome.
- N. gonorrhoeae: Causes PID, septic arthritis, ophthalmia neonatorum.
- Host Factor: Complement deficiency (C5-C9) ↑ risk for recurrent Neisseria infections.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more


