UTI Basics - When Pee Burns
Urinary Tract Infection (UTI): Microbial invasion & inflammation of the urinary system.
- Classification:
Type Description Uncomplicated Healthy, non-pregnant adult female Complicated Structural/functional abnormality; comorbidity Lower UTI Cystitis (bladder), Urethritis (urethra) Upper UTI Pyelonephritis (kidney) Recurrent ≥2 episodes/6 months or ≥3 episodes/1 year - Risk Factors: Female sex, sexual activity, catheterization, obstruction (e.g., stones, BPH), diabetes, immunosuppression.
- Common Pathogens: Escherichia coli (most common, ~80%), Staphylococcus saprophyticus, Klebsiella spp., Proteus mirabilis.
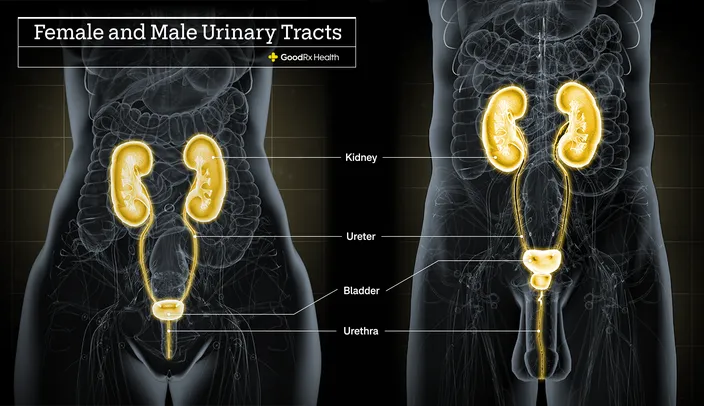
⭐ Uncomplicated UTI is most common in young, sexually active women; E. coli accounts for ~80% of cases.
Bugs & Biofilms - Culprit Critters Crawl
- Routes: Ascending (main), haematogenous. Biofilms on catheters/urothelium aid persistence, ↑drug resistance.
- Virulence: Adhesins (P-fimbriae), toxins (haemolysin), enzymes (urease), capsules.

Common Pathogens: 📌 Mnemonic: "Every Patient Should Know" (E. coli, Proteus, S. saprophyticus, Klebsiella)
| Pathogen | Key Features / Notes |
|---|---|
| Escherichia coli | UPEC; P-fimbriae (pyelo risk), haemolysin. Most common (~80%). |
| Staphylococcus saprophyticus | Young, sexually active women; Adhesins. "Honeymoon cystitis". |
| Klebsiella pneumoniae | Capsule; Nosocomial, diabetics. Mucoid. |
| Proteus mirabilis | Urease → $NH_3$ → ↑alkaline urine; Swarming motility; Struvite stones. |
Signs & Samples - Symptom Sleuthing & Tests
Symptom Spectrum: Cystitis vs. Pyelonephritis
| Feature | Cystitis (Lower UTI) | Pyelonephritis (Upper UTI) |
|---|---|---|
| Local Symptoms | Dysuria, frequency, urgency, suprapubic pain, hematuria. No systemic upset. | Often preceded/accompanied by cystitis symptoms. |
| Systemic | Absent | Fever (>38°C), chills, rigors, flank pain, CVA tenderness, nausea/vomiting. |
- Sample: Mid-Stream Urine (MSU) preferred to ↓contamination.
- Dipstick:
- Leukocyte esterase: +ve (pyuria)
- Nitrites: +ve (Enterobacteriaceae like E.coli) 📌 Nitrites = Gram-Negative Organisms
- Blood: +/- (hematuria)
- Protein: Mild, if present.
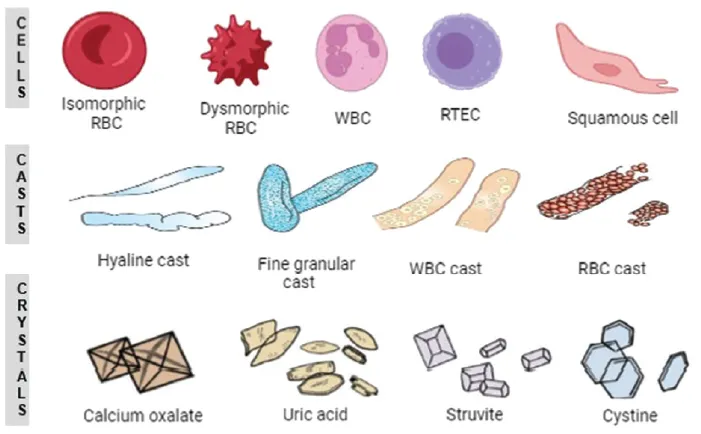
- Microscopy:
- Pyuria: WBCs >5-10/hpf.
- Bacteriuria: Significant if >10^5 CFU/mL (MSU in women); ≥10^3 CFU/mL (MSU in men/catheter); any growth in suprapubic aspirate.
- WBC Casts: Highly suggestive of pyelonephritis/renal involvement.
⭐ Presence of WBC casts in urine is pathognomonic for pyelonephritis or renal parenchymal inflammation.
Diagnostic Algorithm for Suspected UTI:
Treatment & Tricks - Bug Battle Blueprint
Antibiotic Choices:
| Condition | First-line | Alternatives | Duration |
|---|---|---|---|
| Uncomplicated Cystitis | Nitrofurantoin 100mg BD; TMP-SMX DS BD; Fosfomycin 3g x1 | Fluoroquinolones (if unsuitable) | 3-5 days |
| Pyelonephritis (OPD) | Fluoroquinolones (Cipro 500mg BD / Levo 750mg OD) | TMP-SMX (C/S known); Ceftriaxone 1g IV x1 then oral | 7-14 days |
| Pyelonephritis (IPD) | IV Ceftriaxone; IV Pip-Taz | IV Fluoroquinolones; Carbapenems (ESBL) | 10-14 days |
| UTI in Pregnancy | Cephalexin 500mg QID; Amoxi-Clav; Nitrofurantoin (not 1st/term) | Fosfomycin | 7 days |
- Behavioral mod (hydration, voiding), post-coital voiding.
- Prophylaxis: Continuous low-dose (Nitrofurantoin **50-100mg OD**, TMP-SMX **SS OD**) or post-coital.
- CAUTI (Catheter-Associated UTI):
- Treat only if symptomatic.
- Promptly remove/replace catheter.
- Abx per C/S 7-14 days (catheter out: 7d may suffice).
- Asymptomatic Bacteriuria (ASB):
- Screen & treat: Pregnant women; pre-urologic procedures (mucosal trauma).
⭐ Asymptomatic bacteriuria in pregnant women requires treatment to prevent complications like pyelonephritis and preterm labor.
High‑Yield Points - ⚡ Biggest Takeaways
- E. coli is the most common uropathogen.
- Uncomplicated cystitis: Common in healthy, non-pregnant women.
- Complicated UTIs: Associated with pregnancy, diabetes, male sex, or structural issues.
- Diagnosis: Urine culture (>10^5 CFU/mL) and pyuria (>5 WBCs/hpf).
- Asymptomatic bacteriuria: Treat in pregnancy and pre-urological procedures.
- Acute pyelonephritis: Fever, flank pain, CVA tenderness; may need IV antibiotics.
- Recurrent UTIs: ≥2 episodes/6 months or ≥3 episodes/1 year.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

