Definition & Staging - Kidney Crisis Code
Error generating content for this concept group: Failed to process successful response
Etiology - AKI's Usual Suspects
- Prerenal (↓ Perfusion):
- Hypovolemia: Hemorrhage, dehydration, burns
- ↓ Effective volume: CHF, cirrhosis, sepsis/shock
- Drugs: NSAIDs, ACEi/ARBs
- Renal Artery Stenosis
- Intrinsic Renal (Parenchymal Damage):
- ATN (most common): Ischemic; Nephrotoxic (contrast, aminoglycosides, amphotericin B, rhabdomyolysis)
- AIN: Drugs (antibiotics, NSAIDs, PPIs), infections, autoimmune
- Glomerulonephritis (e.g., RPGN)
- Vascular: HUS, TTP, vasculitis, malignant HTN
- Postrenal (Obstruction):
- Ureteric/Bladder neck/Urethral: BPH, stones, tumors, strictures
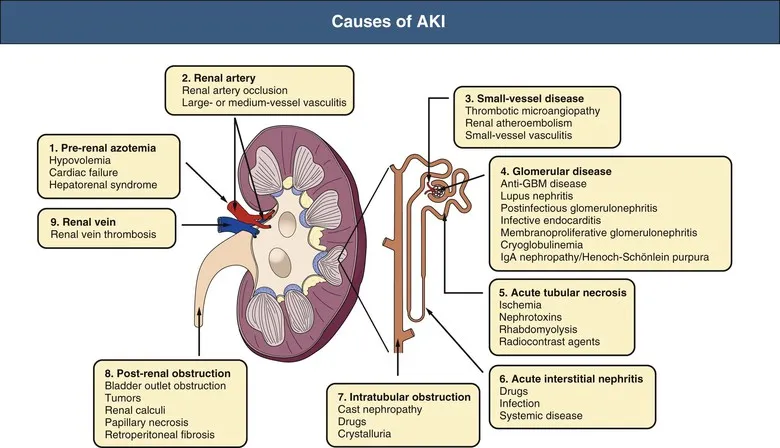
⭐ Acute Tubular Necrosis (ATN) is the most common cause of AKI in hospitalized patients, often due to ischemia or nephrotoxins.
Diagnosis & Evaluation - Kidney Detective Kit
- Clues: History (drugs, ↓intake), exam (volume, bladder).
- Urinalysis (U/A):
- Pre-renal: Bland, high SpGr.
- ATN: Muddy brown casts.
- AIN: WBC casts, eosinophils (📌 Wright/Hansel).
- GN: RBC casts.
- Urine Indices:
- FeNa: <1% (Pre-renal) vs >2% (ATN).
- FeUrea: <35% (Pre-renal, on diuretics).
- Bloods: ↑SCr, BUN:Cr >20:1 (Pre-renal), K↑, acidosis.
- Imaging: US KUB (obstruction? kidney size?).
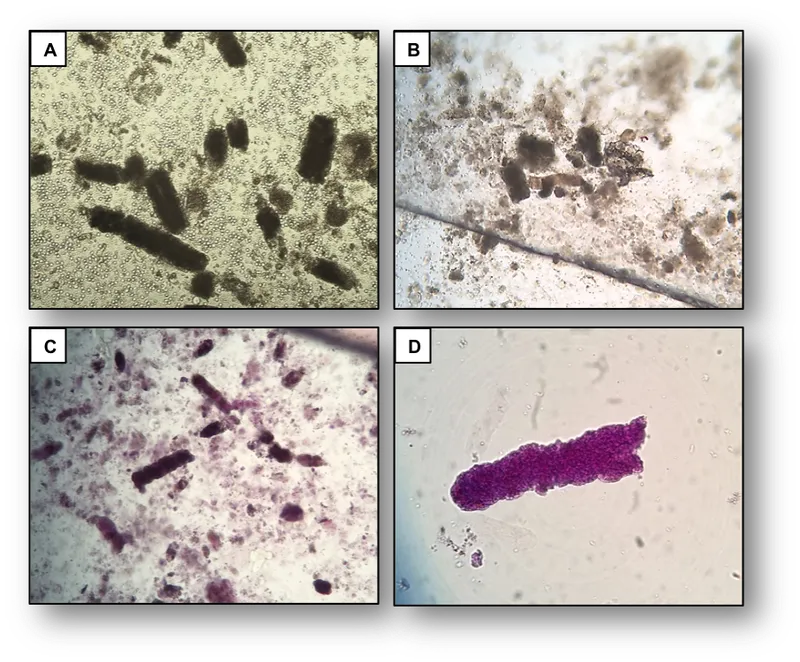
⭐ Muddy brown granular casts in urine sediment are highly suggestive of Acute Tubular Necrosis (ATN).
Complications - AKI's Ripple Effect
- Fluid Overload: Pulmonary edema, hypertension, heart failure.
- Electrolyte Imbalances:
- Hyperkalemia (≥5.5 mEq/L): Peaked T waves, arrhythmias. ⚠️ Most critical!
- Hyponatremia, Hyperphosphatemia, Hypocalcemia.
- Metabolic Acidosis (High Anion Gap).
- Uremic Syndrome:
- Encephalopathy (asterixis).
- Pericarditis (friction rub, tamponade risk).
- Platelet dysfunction (bleeding tendency).
- Increased Infection Risk.
- Cardiovascular: MI, arrhythmias.
- Progression to CKD.
⭐ Uremic pericarditis is an absolute indication for dialysis in AKI.
Management Principles - Kidney Rescue Plan
- Stop nephrotoxic drugs (e.g., NSAIDs, contrast).
- Optimize volume status & maintain MAP >65 mmHg.
- Rule out/Relieve obstruction (e.g., bladder scan, catheter).
- Treat hyperkalemia, severe acidosis.
- Adjust drug dosages to renal function.
- Diuretics (furosemide) for volume overload; not for anuria/oliguria without overload.
⭐ RRT Indications (AEIOU): Acidosis (severe); Electrolytes (refractory hyperK+ >6.5); Intoxications; Overload (refractory); Uremia (symptomatic: pericarditis, encephalopathy).
High‑Yield Points - ⚡ Biggest Takeaways
- AKI (KDIGO): ↑SCr ≥0.3 mg/dL (48h) or ≥1.5x baseline (7d); UO <0.5 mL/kg/h (6h).
- Prerenal: Most common; BUN:Cr >20, FENa <1%; due to hypoperfusion.
- ATN: Intrinsic AKI; muddy brown casts, FENa >2%.
- Postrenal: Obstruction; anuria/polyuria; ultrasound is key.
- Dialysis (AEIOU): Refractory Acidosis, Electrolytes (K⁺>6.5), Intoxications, Overload, Uremia.
- CIN Prevention: IV hydration (isotonic saline) pre-contrast.
- Rhabdomyolysis AKI: ↑CK, myoglobinuria; treat with aggressive hydration, urine alkalinization.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

