IBD Overview & Patho - Fiery Bowel Basics
- Inflammatory Bowel Disease (IBD): Chronic, relapsing-remitting GI tract inflammation.
- Types:
- Crohn's Disease (CD): Mouth to anus; transmural inflammation; skip lesions.
- Ulcerative Colitis (UC): Colon only (rectum often involved); mucosal/submucosal; continuous.
- Epidemiology:
- Increasing incidence in India.
- Bimodal age peaks: 15-30 yrs & 50-70 yrs.
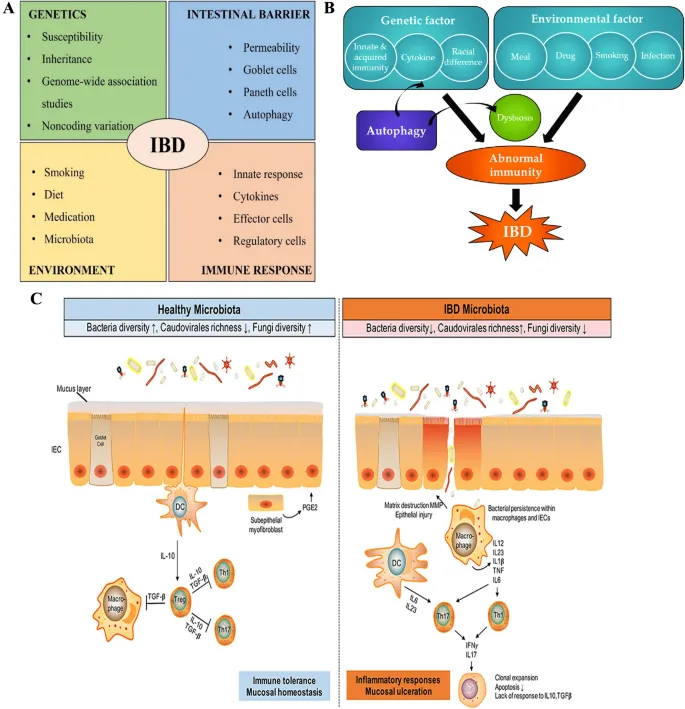
- Pathogenesis: Complex interplay of:
- Immune dysregulation: Exaggerated T-cell response to normal gut microbiota.
- Genetic factors: NOD2/CARD15 (strongest for CD), IL23R, ATG16L1.
- Environmental triggers: Smoking (CD risk ↑, UC protective ↓), diet, NSAIDs, infections.
⭐ > Smoking is protective in Ulcerative Colitis but a risk factor for Crohn's Disease.
CD vs UC Clincher - Tale of Two Guts
| Feature | Crohn's Disease (CD) | Ulcerative Colitis (UC) |
|---|---|---|
| Site | Any part of GIT (mouth to anus); Terminal ileum commonest | Colon only; Rectum invariably involved, extends proximally |
| Pattern | Skip lesions (discontinuous) | Continuous, symmetrical inflammation |
| Depth | Transmural inflammation | Mucosal & submucosal inflammation |
| Symptoms | RLQ pain, diarrhea (±blood), weight loss, perianal disease | Bloody diarrhea, tenesmus, urgency, abdominal cramps |
| Endoscopy | Aphthous ulcers, linear/serpiginous ulcers, cobblestones, strictures, fistulae | Diffuse erythema, granular/friable mucosa, pseudopolyps |
| Radiology | String sign of Kantor (barium study) | Lead pipe colon (loss of haustra) |
| Histology | Non-caseating granulomas (~50%), lymphoid aggregates | Crypt abscesses, crypt distortion, goblet cell depletion |
 vs Ulcerative Colitis (friable mucosa, crypt abscess))
vs Ulcerative Colitis (friable mucosa, crypt abscess))
⭐ > Extraintestinal manifestations are common in both, but p-ANCA is more associated with UC (60-70%), while ASCA is more with CD (60-70%).
IBD Workup - Diagnostic Deep Dive
- Key Investigations:
- Blood: CBC (anemia), ↑ESR/CRP.
- Stool: Fecal Calprotectin (> 50-100 µg/g suggests inflammation; > 250 µg/g highly indicative of IBD).
- Serology: ASCA (CD), pANCA (UC) - supportive, not diagnostic.
- Definitive Diagnosis & Staging:
- Endoscopy (Ileocolonoscopy) + Biopsy: Gold standard for diagnosis, activity, extent.
- Upper GI endoscopy for proximal symptoms.
- Small Bowel & Complication Imaging:
- CT/MR Enterography: Preferred for small bowel assessment, fistulae, abscesses.

- Barium studies (e.g., "String sign of Kantor" in CD).
⭐ Fecal calprotectin > 250 µg/g is highly specific for IBD, aiding differentiation from Irritable Bowel Syndrome (IBS).
IBD Management - Taming the Flames
- Goals: Induce & maintain remission.
- Medical Therapy Pyramid:
- Base: 5-ASA (Mesalamine) - Mild disease.
- Middle: Corticosteroids (flares, e.g., Prednisolone 40-60mg), Immunomodulators (AZA, MTX - maintenance, steroid-sparing).
- Apex: Biologics (Anti-TNF, Anti-integrin, Anti-IL12/23) - Moderate-severe, refractory.
- Acute Severe UC: IV steroids. No response in 3-5 days? → Rescue (Infliximab/Cyclosporine) or colectomy.
- Surgery: Complications (fistulae, strictures, dysplasia/cancer), refractory disease.
⭐ For acute severe UC refractory to IV steroids, Infliximab is a common rescue therapy before considering colectomy.
IBD Fallout - Gut & Beyond
- Gut Complications: Strictures, fistulas, abscesses. Toxic megacolon (UC > CD). Colorectal cancer (CRC) risk ↑ (duration/extent dependent).
- Extra-intestinal Manifestations (EIMs):
- MSK: Arthritis (peripheral, axial - sacroiliitis, ankylosing spondylitis).
- Skin: Erythema nodosum, Pyoderma gangrenosum.
- Ocular: Uveitis, episcleritis.
- Hepatobiliary: Primary Sclerosing Cholangitis (PSC; esp. UC), gallstones (CD).
- Other: Clubbing, aphthous ulcers.

⭐ Primary Sclerosing Cholangitis (PSC) is strongly associated with Ulcerative Colitis and carries a high risk of cholangiocarcinoma.
High‑Yield Points - ⚡ Biggest Takeaways
- Crohn's Disease (CD): Skip lesions, transmural, granulomas, cobblestoning. Terminal ileum common. ASCA positive.
- Ulcerative Colitis (UC): Continuous colonic, starts rectum, mucosal only, crypt abscesses, pseudopolyps. p-ANCA positive.
- Complications: CD: fistulas, strictures. UC: toxic megacolon, ↑CRC risk.
- EIMs: Arthritis, uveitis, erythema nodosum, pyoderma gangrenosum, PSC (UC > CD).
- Smoking: Worsens CD; protective for UC.
- Treatment: 5-ASA (mild UC), steroids (flares), immunomodulators, biologics.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

