Anatomy & Physiology - Tiny Glands, Big Impact
- Typically 4 glands, posterior to thyroid; ectopic sites common.
- Blood: Mainly inferior thyroid artery.
- Cells: Chief cells (PTH secretion); Oxyphil cells.
- PTH: Regulates $Ca^{2+}$/$PO_4^{3-}$ homeostasis.
- Trigger: ↓ Serum $Ca^{2+}$.
- Actions: ↑ Bone resorption; Kidney: ↑ $Ca^{2+}$ reabsorb, ↓ $PO_4^{3-}$ reabsorb, ↑ Vit D active.
- Result: ↑ Serum $Ca^{2+}$, ↓ Serum $PO_4^{3-}$.
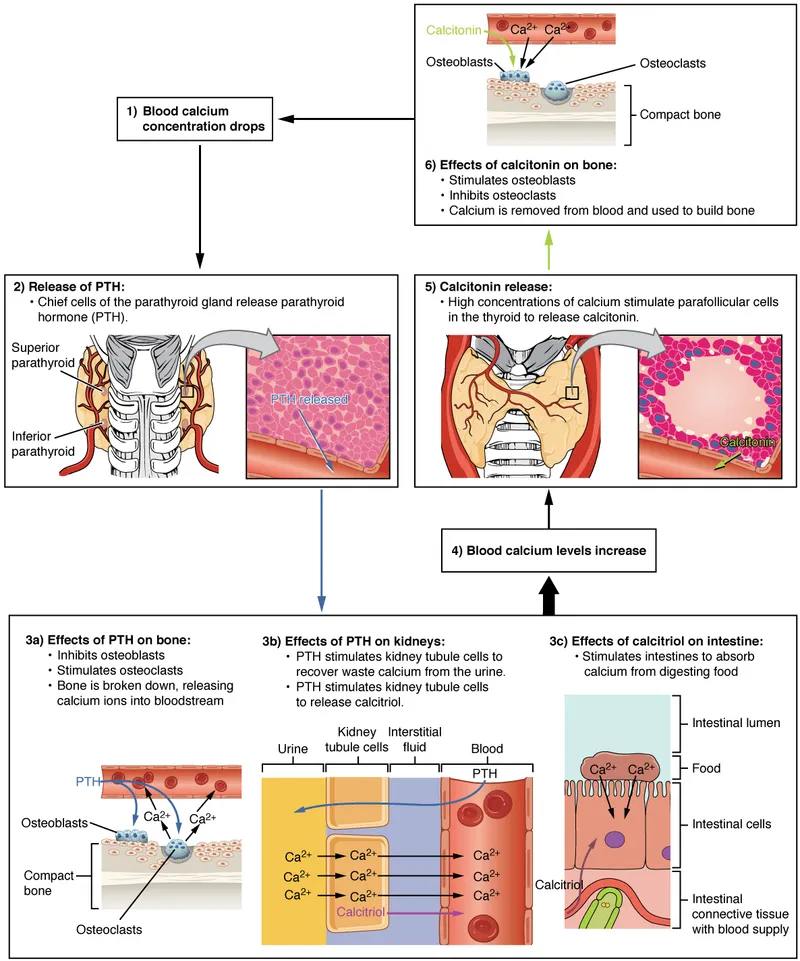
⭐ PTH enhances calcium reabsorption mainly in the kidney's Distal Convoluted Tubule (DCT).
Hyperparathyroidism - Calcium Chaos Creators
-
Excess PTH secretion leading to ↑ serum $Ca^{2+}$.
-
Types & Etiology:
- Primary: Adenoma (~85%), hyperplasia, carcinoma.
- Secondary: CKD (most common), Vit D deficiency.
- Tertiary: Autonomous PTH after chronic secondary.
-
Clinical Features: 📌 "Stones, Bones, Groans, Moans, Psychic Overtones"
- Stones: Renal ($Ca^{2+}$).
- Bones: Osteitis fibrosa cystica (OFC, brown tumors), subperiosteal resorption, pain.
- Groans: Abdominal pain, PUD, pancreatitis.
- Moans/Psychic: Fatigue, depression, confusion.
-
Investigations:
- Labs: ↑PTH, ↑$Ca^{2+}$, ↓$PO_4^{3-}$, ↑ALP, ↑urine cAMP.
- Imaging: Sestamibi, USG neck. X-ray: subperiosteal resorption (phalanges), 'salt & pepper' skull.
-
Management:
- Primary: Parathyroidectomy (symptomatic; or asymptomatic if: Age <50y, Serum $Ca^{2+}$ >1mg/dL above ULN, BMD T-score ≤-2.5, CrCl <60mL/min, Urine $Ca^{2+}$ >400mg/d). Medical: Cinacalcet.
- Secondary/Tertiary: Treat cause / Parathyroidectomy.
⭐ Subperiosteal bone resorption, especially of the radial aspects of the middle phalanges, is pathognomonic for hyperparathyroidism.
Hypoparathyroidism - Calcium Calamity
- ↓PTH → ↓Serum $Ca^{2+}$, ↑Serum $PO_4^{3-}$.
- Etiology:
- Most common: Post-surgical (thyroid/parathyroid surgery).
- Autoimmune, DiGeorge syndrome (22q11.2 deletion).
- Severe hypomagnesemia (functional).
- Clinical Features (Hypocalcemia):
- Neuromuscular: Tetany (Chvostek's, Trousseau's signs), paresthesias, muscle cramps, seizures.
- 📌 Mnemonic: "CATS go numb" (Convulsions, Arrhythmias, Tetany, Spasms).
- ECG: Prolonged QT interval.
- Chronic: Cataracts, basal ganglia calcification.
- Neuromuscular: Tetany (Chvostek's, Trousseau's signs), paresthesias, muscle cramps, seizures.
- Diagnosis: ↓Serum $Ca^{2+}$ (< 8.5 mg/dL), ↑Serum $PO_4^{3-}$, ↓PTH.
- Management:
- Acute: IV Calcium gluconate.
- Chronic: Oral calcium, Vitamin D (Calcitriol).

⭐ The most common cause of hypoparathyroidism is iatrogenic, following anterior neck surgery (e.g., thyroidectomy).
Diagnostics & Surgery - Scalpels & Scans
- Biochemical Diagnosis:
- ↑ Serum Ca (Total & Ionized), ↓ Serum Phosphate, ↑ PTH.
- ↑ 24-hr Urinary Ca, ↑ ALP (bone isoenzyme).
- Assess Vitamin D levels (rule out secondary HPT).
- Localization Studies (Pre-operative):
- Sestamibi Scan (Tc-99m): Primary modality; SPECT/CT enhances accuracy.
⭐ Sestamibi scan is the gold standard for preoperative localization of parathyroid adenomas, especially with SPECT/CT.
- Ultrasound Neck: Good for cervical glands, guides FNA; operator-dependent.
- 4D CT Scan: High resolution; for ectopic glands, reoperations.
- MRI: Alternative if others inconclusive/contraindicated.
- Sestamibi Scan (Tc-99m): Primary modality; SPECT/CT enhances accuracy.
- Surgery (Parathyroidectomy): Definitive treatment.
- Indications (Asymptomatic Primary HPT):
- Serum Ca > 1 mg/dL above upper limit of normal.
- Bone: T-score < -2.5 (osteoporosis) or fragility fracture.
- Renal: CrCl < 60 mL/min or 24-hr urine Ca > 400 mg/day / nephrolithiasis.
- Age < 50 years.
- Surgical Approaches:
- Minimally Invasive Parathyroidectomy (MIP): For pre-operatively localized single adenoma.
- Bilateral Neck Exploration (BNE): If localization fails or multiglandular disease suspected.
- Intraoperative PTH (IOPTH) Monitoring: Miami criterion: >50% drop from baseline 10 min post-excision confirms successful removal.
- Indications (Asymptomatic Primary HPT):
High‑Yield Points - ⚡ Biggest Takeaways
- Primary HPT: Most often parathyroid adenoma; causes hypercalcemia, hypophosphatemia, ↑PTH.
- Secondary HPT: Usually from CKD; features hypocalcemia/normal Ca, hyperphosphatemia, ↑PTH.
- Tertiary HPT: Autonomous PTH secretion after long-standing secondary HPT; leads to hypercalcemia.
- FHH: CaSR gene mutation; mild hypercalcemia, low urine calcium. Differentiate from primary HPT.
- Sestamibi scan: Key for localizing adenomas. Intraoperative PTH confirms removal.
- Hungry Bone Syndrome: Post-op hypocalcemia due to rapid bone uptake.
- MEN syndromes: Associate parathyroid issues with MEN 1 and MEN 2A.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

