Onychomycosis - Fungal Nail Invaders
- Definition: Fungal infection of the nail unit (nail plate, bed, matrix).
- Epidemiology: Common, prevalence ↑ with age; significant in India.
- Risk Factors:
- Diabetes mellitus
- Peripheral Vascular Disease (PVD)
- Immunosuppression
- Chronic tinea pedis
- Occlusive footwear
- Etiology:
- Dermatophytes (Most common):
- Trichophyton rubrum
- Trichophyton mentagrophytes
- Yeasts:
- Candida albicans (esp. fingernails, associated with chronic paronychia)
- Non-Dermatophyte Molds (NDMs):
- Aspergillus spp., Fusarium spp., Scopulariopsis brevicaulis
- Often soil saprophytes, opportunistic pathogens.
- Dermatophytes (Most common):
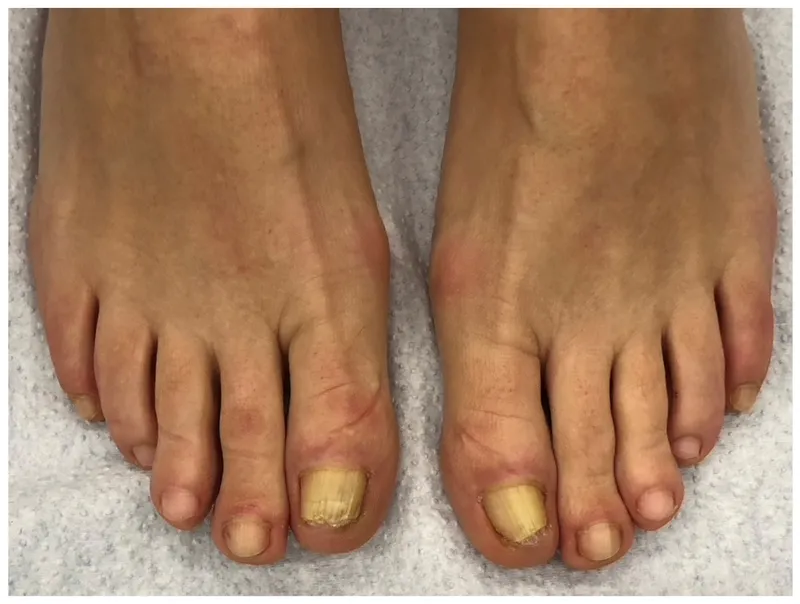
⭐ Trichophyton rubrum is the most common etiological agent for onychomycosis globally and in India.
Onychomycosis - Nail's Many Woes
Clinical classification is based on the pattern of nail invasion.
| Type | Invasion Pattern & Key Features | Common Organisms |
|---|---|---|
| DLSO (Distal Lateral Subungual) | Most common. Hyponychium/lateral fold entry → proximal spread. Subungual hyperkeratosis, onycholysis, yellow-brown discoloration. | T. rubrum |
| WSO (White Superficial) | Superficial nail plate. Chalky white patches, easily scraped. | T. mentagrophytes |
| PSO (Proximal Subungual) | Least common (healthy). Proximal nail fold/cuticle entry. Marker for immunosuppression (HIV). | T. rubrum |
| EO (Endonyx) | Nail plate interior invasion. No subungual debris/onycholysis. Milky white discoloration. | Trichophyton soudanense |
| TDO (Total Dystrophic) | End-stage of any type. Complete nail destruction. | Various fungi |
| Candida Onychomycosis | Often fingernails. Chronic paronychia, nail plate thickening, yellow-green-black discoloration, onycholysis. Immunosuppression. | Candida albicans |
⭐ Proximal Subungual Onychomycosis (PSO) is strongly associated with HIV infection and indicates underlying immunosuppression.
Onychomycosis - Spotting the Spores
Diagnosis confirmation is crucial before systemic therapy.
- Specimen Collection:
- Nail clippings (distal, crumbling) & subungual debris.
- Avoid topical antifungals for 1-2 weeks prior.
- Diagnostic Tests:
- Direct Microscopy (KOH Mount): Rapid, inexpensive. Uses $10-40%$ KOH solution $\pm$ DMSO. Visualizes hyphae, arthrospores. Sensitivity $\approx extbf{60-80}%$.

- Fungal Culture: Gold standard for species ID. Sabouraud Dextrose Agar (SDA) $\pm$ cycloheximide. Slow growth (2-6 weeks). Sensitivity $\approx extbf{40-60}%$.
- Histopathology (Nail Biopsy with PAS stain): Periodic Acid-Schiff stain highlights fungal elements. Highest sensitivity ($ extbf{80-95}%$). Useful if KOH/culture negative but high suspicion.

- Dermoscopy: Shows patterns (e.g., longitudinal striae, spiked pattern, ruin-like appearance).
- Newer Methods: PCR (high sensitivity, rapid), Dermatophyte Test Medium (DTM - color change).
- Direct Microscopy (KOH Mount): Rapid, inexpensive. Uses $10-40%$ KOH solution $\pm$ DMSO. Visualizes hyphae, arthrospores. Sensitivity $\approx extbf{60-80}%$.
⭐ PAS staining of a nail clipping is the most sensitive diagnostic test for onychomycosis.
Onychomycosis - Kicking the Fungus
- Goals: Achieve mycological and clinical cure, and prevent recurrence. Treatment choice depends on clinical type, severity, specific organism, and patient factors.
- Topical: For mild-moderate cases (e.g., WSO, <50% nail involvement, no lunula). Examples: Ciclopirox 8% lacquer, Amorolfine 5% lacquer. Duration: 6-12 months.
- Systemic: For moderate-severe cases (DLSO with lunula involvement, PSO, or multiple nail involvement).
- 📌 'Terbinafine for Toes, Itraconazole in Pulses' | Drug | Dose | Duration (FN/TN) | Key S/E / Monitor | |--------------|------------------------------------------|----------------------------------|-------------------| | Terbinafine | 250 mg/day | 6w / 12w | Monitor LFTs | | Itraconazole | 200 mg/day OR 200mg BID 1wk/mo | 6w/12w or 2/3-4 pulses | Monitor LFTs | | Fluconazole | 150-300 mg weekly | 6-12 months | GI upset |
- Combination: Systemic + topical may ↑ cure.
- Adjuncts: Nail debridement/avulsion, laser therapy.
- NDM/Candida: Itraconazole often preferred. Resistance common.
- Prevention: Treat tinea pedis, hygiene, avoid trauma.
⭐ Terbinafine 250 mg/day for 12 weeks is first-line for dermatophyte toenail onychomycosis (high efficacy, fungicidal).
High-Yield Points - ⚡ Biggest Takeaways
- Most common cause: Trichophyton rubrum.
- DLSO (Distal Lateral Subungual Onychomycosis) is the most frequent clinical type.
- Diagnosis: KOH mount (septate hyphae) and fungal culture are key; PAS stain for nail biopsy.
- Oral terbinafine is first-line for dermatophyte onychomycosis; requires LFT monitoring.
- Topical therapy (e.g., ciclopirox, efinaconazole) for superficial white onychomycosis or mild DLSO.
- PSO (Proximal Subungual Onychomycosis) is often linked to immunosuppression (e.g., HIV).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

