Stasis Dermatitis: Pathophysiology - Pooling Problems
- Definition: Eczematous dermatitis of lower legs due to chronic fluid pooling from chronic venous insufficiency (CVI).
- Etiology: CVI impairs venous return from legs, causing blood stasis and increased pressure.
- Key Pathophysiological Steps:
- Venous Hypertension: Sustained high pressure in leg veins damages valves.
- Capillary Leakage: ↑ pressure forces fluid, proteins, and RBCs from capillaries into dermal tissue.
- Inflammation: Stagnation and leakage trigger local inflammatory cascade and cytokine release.
- Hemosiderin Deposition: Extravasated RBCs break down; iron (hemosiderin) deposits cause brownish skin.
⭐ Often the earliest cutaneous sign of chronic venous insufficiency.
Stasis Dermatitis: Clinical Features - Itchy Leg Alert
- Location: Primarily affects lower legs, especially medial ankles; the "gaiter area." Often bilateral.
- Early Signs:
- Erythema, scaling, and eczematous patches.
- Pruritus is a hallmark symptom, often intense.
- Pitting edema, worse with dependency.
- Late Signs (Chronic Changes):
- Lichenification from chronic rubbing/scratching.
- Hyperpigmentation: Brownish discoloration, "cayenne pepper" spots (hemosiderin).
- Lipodermatosclerosis: Hardening, thickening of skin; may lead to:
⭐ Lipodermatosclerosis presents as an "inverted champagne bottle" appearance of the leg.
- Atrophie blanche: White, stellate, porcelain-like scars.
- Venous ulcers: Often painful, over medial malleolus.

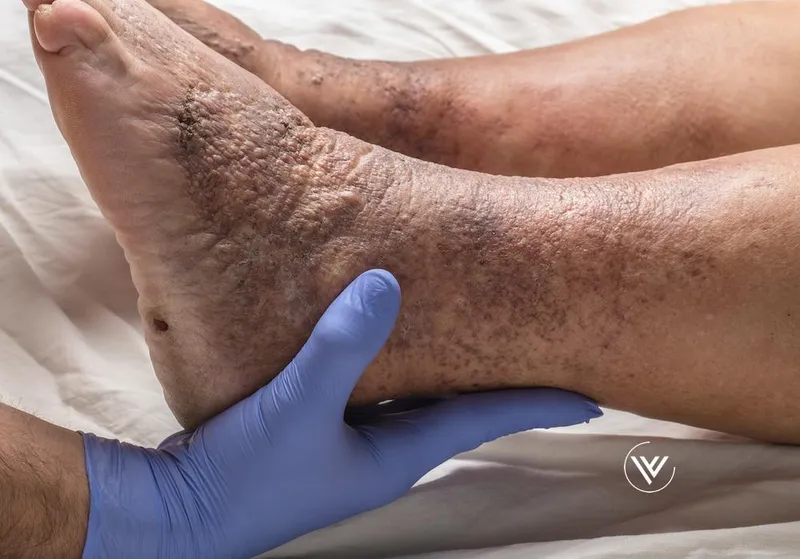
Stasis Dermatitis: Diagnosis & Differentials - Spotting the Stasis
- Clinical Diagnosis: Based on history (leg swelling, varicose veins) & exam (erythema, scale, hemosiderin deposition on lower legs).
- Doppler Ultrasound: Essential to confirm underlying Chronic Venous Insufficiency (CVI).
- Key Differentials:
- Contact dermatitis (patch testing)
- Cellulitis (acute, fever, unilateral)
- Asteatotic eczema (xerosis, "cracked pavement")
- Tinea corporis (annular lesions, KOH)
- Psoriasis (silvery scales, extensor sites)
⭐ Bilateral involvement is common, but unilateral presentation should raise suspicion for DVT or lymphedema.
Stasis Dermatitis: Management - Leg Up Care
- Core Conservative Care:
- Leg elevation: Above heart level, frequently.
- Compression therapy: Essential. Graduated stockings, multi-layer bandages.
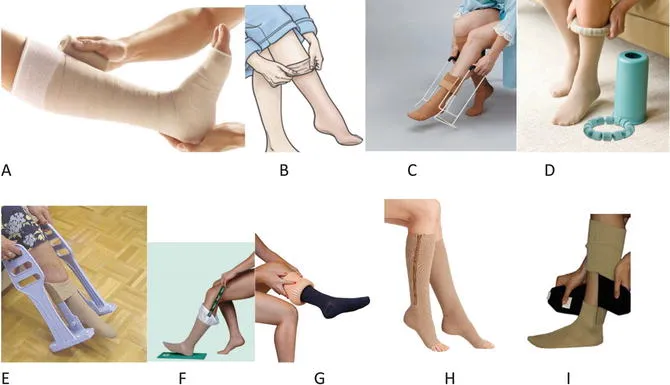
- Pressure: 20-30 mmHg (mild-moderate), 30-40 mmHg (severe).
- Topical Management:
- Emollients: Apply liberally and regularly.
- Topical corticosteroids: Mid-potency (e.g., triamcinolone 0.1%) for 1-2 weeks during flares.
- Addressing Complications:
- Weeping lesions: Wet compresses (e.g., Burow's solution, saline) until dry.
- Secondary infection: Topical (e.g., mupirocin) or systemic antibiotics based on severity.
- Systemic Therapy (severe/refractory cases):
- Diuretics: Cautious use for significant edema.
- Pentoxifylline: May improve healing.
⭐ Compression therapy is the cornerstone of stasis dermatitis management.
Stasis Dermatitis: Complications & Prevention - Trouble Ahead
- Key Complications:
- Secondary bacterial infection (e.g., cellulitis)
- Allergic contact dermatitis (often to topical treatments)
- Autoeczematization (Id reaction)
- Venous ulceration (frequent, serious)
- Lipodermatosclerosis (fibrosis, "inverted champagne bottle" leg)
- Atrophie blanche (stellate white scars)
- Prevention Strategies:
- Manage CVI: leg elevation, compression therapy, calf exercises
- Lifestyle: avoid prolonged static positions, gentle skin care, emollients
⭐ Allergic contact dermatitis to components of topical medications or dressings is a frequent complication.
oka
High‑Yield Points - ⚡ Biggest Takeaways
- Caused by chronic venous insufficiency (CVI) leading to venous hypertension.
- Typically affects lower legs, especially the medial malleoli.
- Presents with edema, erythema, scaling, pruritus, and later hemosiderin deposition (brownish discoloration).
- Lipodermatosclerosis ("inverted champagne bottle" leg) and venous ulcers are late complications.
- Atrophie blanche (stellate white scars) may also be seen.
- Management focuses on compression therapy, leg elevation, and topical steroids.
- Key complications: ulceration, cellulitis, and contact sensitization (e.g., to neomycin).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

