SSSS Introduction - Scaly Skin Saga
- A superficial blistering skin condition caused by specific Staphylococcus aureus strains.
- Primarily affects neonates, infants, and young children (typically <5 years).
- Pathogenesis: Mediated by exfoliative toxins (ETA and ETB).
- These toxins specifically cleave desmoglein-1.
- Site of cleavage: Stratum granulosum of the epidermis.
- Leads to widespread erythema, bullae formation, and subsequent desquamation.
- Nikolsky sign is characteristically positive.

⭐ Exfoliative toxins (ETA, ETB) from Staphylococcus aureus cleave desmoglein-1 in the stratum granulosum.
Clinical Features - Red, Raw, Peeling
- Initial Phase: Prodrome of fever, irritability, and diffuse skin tenderness.
- Erythema & Bullae Formation:
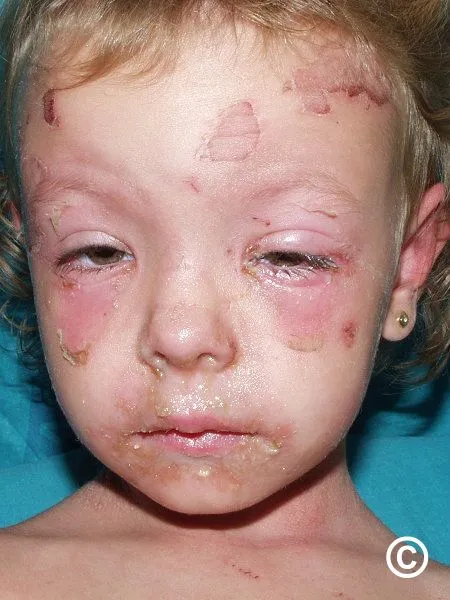
- Widespread, tender erythema appears; often starts periorificially (mouth, eyes), neck, axillae, and groin.
- Within 24-48 hours, large, flaccid, sterile bullae develop.
- Bullae rupture easily, revealing moist, red, raw "scalded" skin surface.
- Characteristic Signs:
- Exquisite pain and tenderness on palpation.
- Mucous membranes are typically spared (important diagnostic clue).
⭐ Nikolsky's sign (gentle rubbing causes exfoliation of the outermost skin layer) is typically positive in SSSS.
- Distribution: Primarily affects flexural areas, trunk, and periorificial regions; palms and soles usually spared.
- Resolution: Rapid healing within 7-10 days if treated, typically without scarring.
Diagnosis & Differentials - Spotting the Scald
- Clinical Dx: Sudden onset erythroderma, fever, skin tenderness, positive Nikolsky sign.
- Skin Biopsy (Gold Standard):
- Intraepidermal split at stratum granulosum.
- Minimal/no inflammatory cells in blister.
⭐ Skin biopsy in SSSS shows an intraepidermal split at the stratum granulosum level, with minimal or no inflammatory cells in the blister cavity, distinguishing it from TEN.
- Cultures:
- Source: Blood, nasopharynx, suspected primary site (NOT intact blister).
- Blister fluid: Usually sterile.
- Key Differentials:
- Toxic Epidermal Necrolysis (TEN): Deeper split (dermo-epidermal), severe mucosal involvement, drug hx.
- Bullous Impetigo: Localized, culture-positive blisters.
- Kawasaki Disease: No Nikolsky, coronary concerns.
Management & Prognosis - Soothe & Subdue
- Core Management (Hospitalize):
- Supportive: Crucial. IV fluids, electrolyte balance, temperature control, meticulous skin care (emollients, non-adherent dressings to minimize trauma), analgesia.
- Antibiotics: IV anti-staphylococcal (Nafcillin, Oxacillin, Flucloxacillin). Add Clindamycin (inhibits toxin). Vancomycin if MRSA suspected/confirmed.
- Prognosis:
- Children: Generally excellent. Full recovery typically within 7-14 days, usually without scarring.
- Adults & Immunocompromised: Higher morbidity/mortality.
⭐ Corticosteroids are contraindicated in SSSS as they can impair immune response and worsen the condition.
High‑Yield Points - ⚡ Biggest Takeaways
- Caused by Staphylococcal exfoliative toxins (ETA, ETB) targeting desmoglein-1.
- Leads to intraepidermal split at stratum granulosum; Nikolsky sign positive.
- Presents as tender erythroderma, widespread bullae, and desquamation, mainly in children <5 years.
- Mucous membranes are characteristically spared, distinguishing it from TEN/SJS.
- Bullae are sterile as it's toxin-mediated; biopsy shows subcorneal split.
- Treat with systemic anti-staphylococcal antibiotics and supportive measures.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

