LSDs Overview - Enzyme Trouble Tales
- LSDs Defined: Inherited metabolic disorders; specific enzyme deficiency → lysosomal dysfunction → toxic accumulation of undegraded substrates.
- Common Features: Progressive, multi-systemic involvement.
- Organomegaly (esp. hepatosplenomegaly).
- Neurological regression/decline.
- Skeletal dysplasia (e.g., dysostosis multiplex).
- Coarse facial features (in some types).
- Inheritance Pattern: Mostly Autosomal Recessive (AR).
- 📌 Key Exceptions (X-Linked Recessive): Fabry disease, Hunter syndrome (MPS II).
- Basic Pathophysiology: Deficient lysosomal enzyme → Accumulation of its specific substrate within lysosomes → Cellular engorgement & dysfunction → Progressive organ damage.
⭐ Most Lysosomal Storage Diseases are Autosomal Recessive. Remember the two major X-Linked Recessive exceptions: Fabry disease and Hunter syndrome (MPS II).
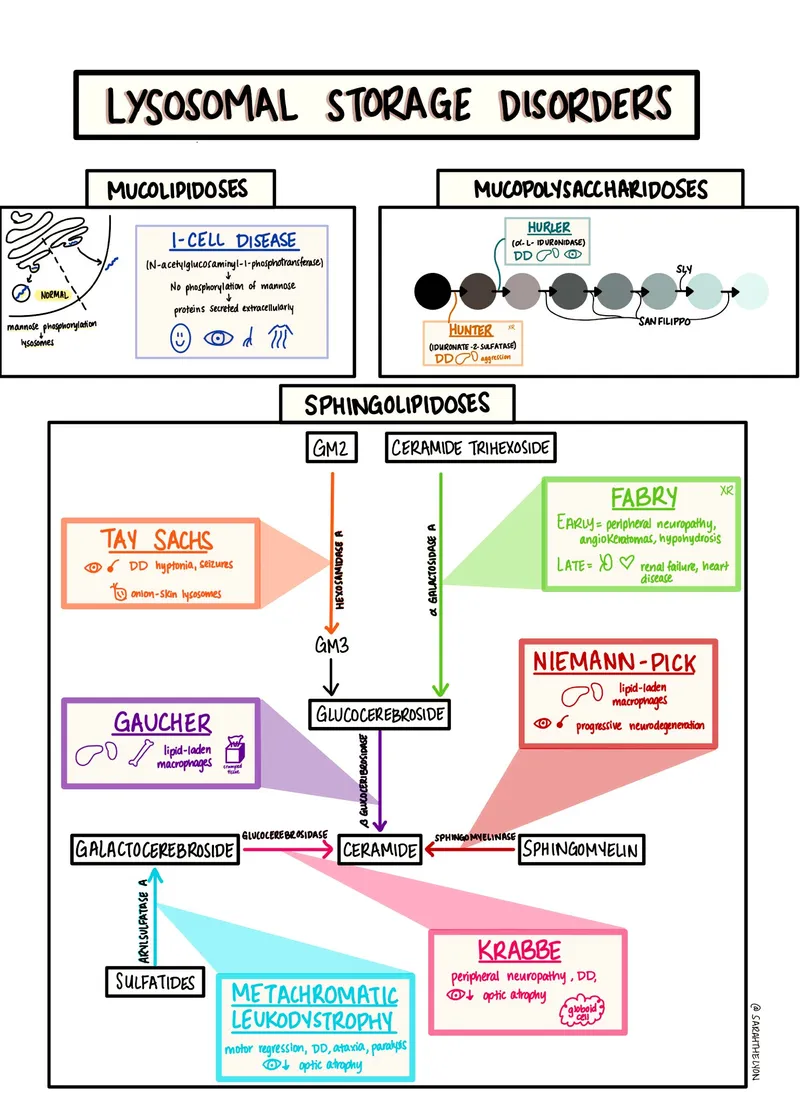
Sphingolipidoses - Lipid Mayhem Mess
- Gaucher Disease: Glucocerebrosidase ↓; Glucocerebroside ↑. Hepatosplenomegaly, pancytopenia, bone crises, pain. 📌 Gaucher cells (crumpled tissue paper macrophages), Erlenmeyer flask deformity.
- Niemann-Pick Disease (A/B): Sphingomyelinase ↓; Sphingomyelin ↑. Type A: Severe neurodegeneration, cherry-red spot, hepatosplenomegaly, early death. Type B: Visceral, less neuro. 📌 Foam cells.
- Tay-Sachs Disease: Hexosaminidase A ↓; GM2 Ganglioside ↑. Progressive neurodegeneration, developmental delay, cherry-red spot (NO hepatosplenomegaly). 📌 Onion-skin lysosomes.
- Fabry Disease (X-linked): α-Galactosidase A ↓; Globotriaosylceramide (Gb3) ↑. Episodic peripheral neuropathy (acroparesthesias), angiokeratomas, hypohidrosis, renal failure, cardiac issues.
- Krabbe Disease (Globoid Cell Leukodystrophy): Galactocerebrosidase ↓; Galactocerebroside/Psychosine ↑. Rapid neurodegeneration, irritability, optic atrophy, peripheral neuropathy. 📌 Globoid cells.
- Metachromatic Leukodystrophy (MLD): Arylsulfatase A ↓; Sulfatides ↑. Progressive demyelination → motor (ataxia) & cognitive decline, peripheral neuropathy.
⭐ Tay-Sachs and Niemann-Pick Type A both present with a cherry-red spot, but Tay-Sachs lacks hepatosplenomegaly.
Mucopolysaccharidoses - Sugar Stash Snags
- General: Defective Glycosaminoglycan (GAG) breakdown. Chronic, progressive.
- Features: Coarse facies, dysostosis multiplex, organomegaly, joint stiffness. Corneal clouding (exceptions: Hunter, Sanfilippo).
- Hurler Syndrome (MPS I-H):
- Deficiency: $\alpha$-L-Iduronidase. AR.
- Key: Most severe. Corneal clouding, HSM, neurodegeneration.
- Hunter Syndrome (MPS II):
- Deficiency: Iduronate-2-Sulfatase. X-Linked Recessive.
- Key: NO corneal clouding.
- 📌 Mnemonic: "Hunters see clearly (no corneal clouding) & aim for X (X-linked)".
- Others:
- Sanfilippo (MPS III): Neurodegeneration.
- Morquio (MPS IV): Severe skeletal issues, normal intellect, corneal clouding.
⭐ Hunter Syndrome (MPS II) is the only X-linked recessive MPS; others are autosomal recessive.

LSD Diagnosis & Management - Spot & Support Strategy
- Diagnosis:
- Clinical suspicion guides.
- Enzyme assays (leukocytes, fibroblasts, plasma specific to LSD).
- Genetic testing (confirmatory, carrier detection, prenatal).
- Urine GAG analysis for MPS.
- Management: Largely supportive & symptomatic.
- ERT: For Gaucher, Fabry, Pompe, MPS I, II, IVA, VI. Regular IV.
⭐ ERT is available for Gaucher, Fabry, Pompe, and several MPS types, but is costly with limited CNS reach.
- SRT: Oral drugs. Miglustat (Gaucher type 1, NPC), Eliglustat (Gaucher type 1).
- HSCT: For some CNS forms (e.g., early Hurler, Krabbe) if done early.
- Future: Gene therapy, chaperone therapy.
- ERT: For Gaucher, Fabry, Pompe, MPS I, II, IVA, VI. Regular IV.
High‑Yield Points - ⚡ Biggest Takeaways
- LSDs: Caused by deficient lysosomal enzymes leading to substrate accumulation.
- Inheritance: Mostly autosomal recessive, except Fabry & Hunter (X-linked).
- Gaucher: Glucocerebrosidase deficiency; crumpled tissue paper cells; hepatosplenomegaly.
- Tay-Sachs: Hexosaminidase A deficiency; cherry-red spot; NO hepatosplenomegaly.
- Niemann-Pick: Sphingomyelinase deficiency; cherry-red spot; hepatosplenomegaly; foam cells.
- Fabry: α-Galactosidase A deficiency; X-linked; angiokeratomas, peripheral neuropathy.
- Hunter (MPS II): Iduronate-2-sulfatase deficiency; X-linked; aggressive behavior, NO corneal clouding.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

