Intraoperative Monitoring - ASA's Vigilant Five
- Oxygenation:
- Inspired O2 analyzer (detects hypoxic mixture).
- Pulse oximetry (SpO2 >92%; detects hypoxemia).
- Ventilation:
- Capnography (ETCO2 35-45 mmHg): Confirms ETT, assesses ventilation.
- Clinical signs: chest rise, breath sounds.
- Circulation:
- ECG (continuous): Detects arrhythmias, ischemia.
- Blood Pressure (NIBP/IBP): q3-5min; maintain MAP within 20% of baseline.
- Peripheral pulse palpation/plethysmography.
- Temperature:
- Core temperature monitoring (e.g., esophageal, nasopharyngeal).
- Maintain normothermia (36.0-37.5°C).
- Neuromuscular Function (if NMBAs used):
- Peripheral Nerve Stimulator (PNS): Assesses block depth.
- Train-of-Four (TOF) count/ratio (target TOF ratio >0.9 for safe extubation).
⭐ Capnography (ETCO2) is the most reliable method to confirm endotracheal tube placement immediately after intubation and continuously monitor ventilation adequacy during general anesthesia an
Intraoperative Monitoring - Heart's Beat & Flow
- ECG: Standard 5-lead (II & V5 for ischemia). Detects arrhythmias, ischemia (ST >1mm), K+.
- Invasive Cardiovascular Monitoring:
| Feature | IBP (Arterial Line) | CVP (Central Line) | PAC (Swan-Ganz) |
|---|---|---|---|
| Site | Radial | IJV (R) | IJV (R) -> PA |
| Measures | Real-time BP, MAP; ABGs | RAP (2-6 mmHg); volume | PAP, PCWP (6-12 mmHg), CO, SvO2 |
| Key Ind. | Unstable BP; ABGs | Major surgery; fluids | Cardiac dx; shock; ARDS |
| Waveform | 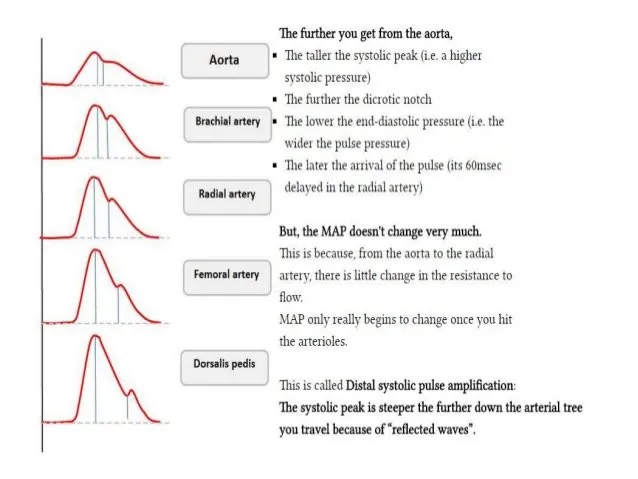 | 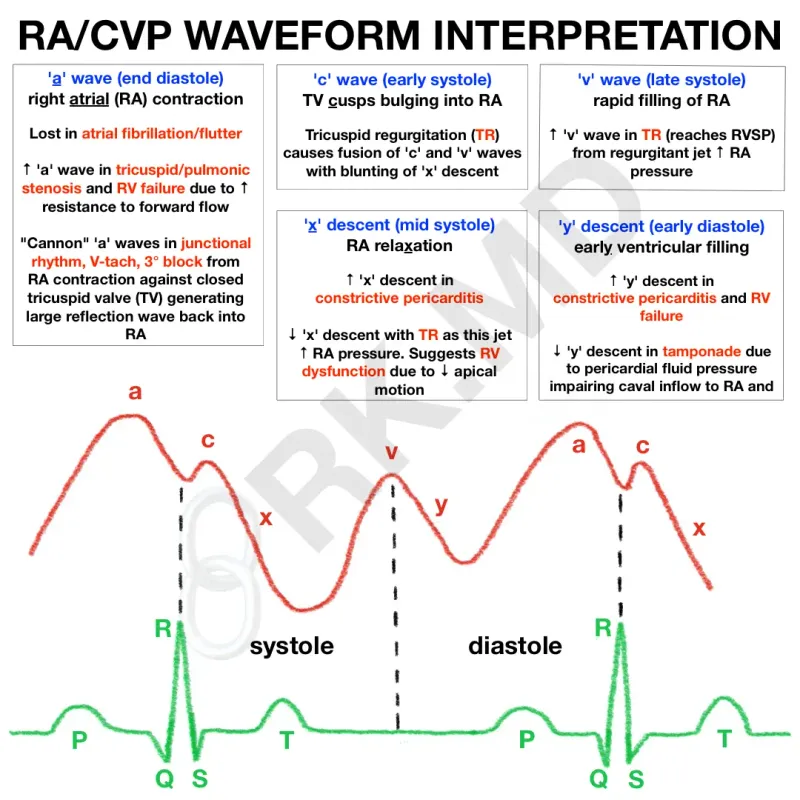 | 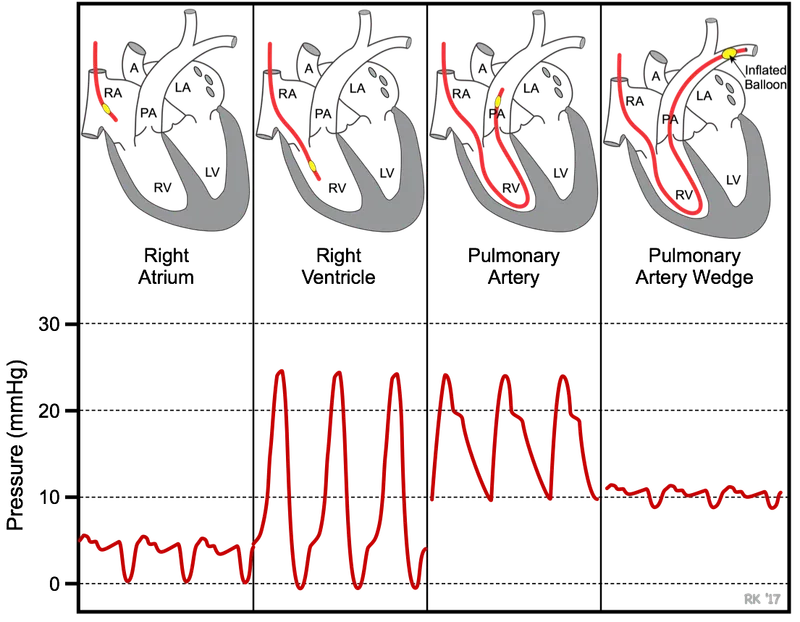 |
Intraoperative Monitoring - Breath by Breath
- Capnography: Gold standard for ETT placement confirmation.
- Measures $P_{ET}CO_2$; normal range 35-45 mmHg.
- $P_{a}CO_2 - P_{ET}CO_2$ gradient: normally 2-5 mmHg; ↑ with ↑ dead space (e.g., PE, ↓ cardiac output).
- Waveform: Phase I (baseline/dead space), II (expiratory upstroke), III (alveolar plateau), 0 (inspiratory downstroke).
- 📌 Mnemonic: "No Trace, Wrong Place!" (for absent $P_{ET}CO_2$ after intubation).
⭐ Sudden ↓ $P_{ET}CO_2$ to 0 or near 0 indicates esophageal intubation, ventilator disconnect, or cardiac arrest.
- Ventilator Parameters & Spirometry:
- Tidal Volume ($V_T$): Target 6-8 mL/kg Ideal Body Weight.
- Plateau Pressure ($P_{plat}$): Keep <30 cmH2O (lung protective ventilation).
- Driving Pressure ($P_{plat}$ - PEEP): Aim for <15 cmH2O.
- Loops (Volume-Pressure, Flow-Volume): Diagnose obstruction (e.g., bronchospasm), leaks, compliance changes.
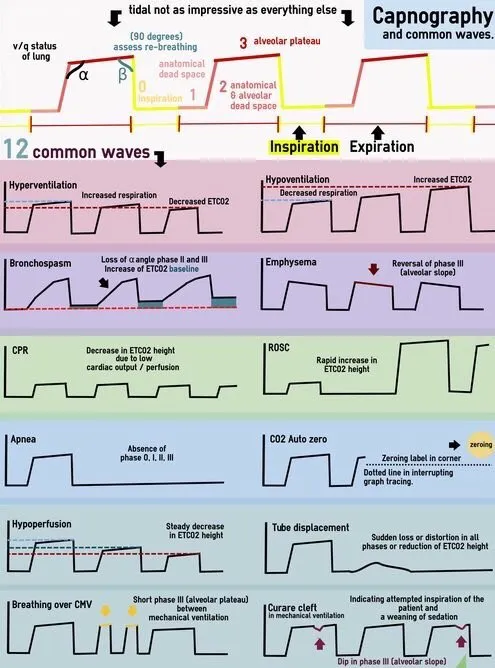
Intraoperative Monitoring - Nerve & Muscle Check
Nerve (Depth of Anesthesia):
- Bispectral Index (BIS):
- Measures hypnotic effect. Range: 0-100.
- Target for GA: 40-60.
- < 40: Deep hypnosis; > 60: Risk of awareness.
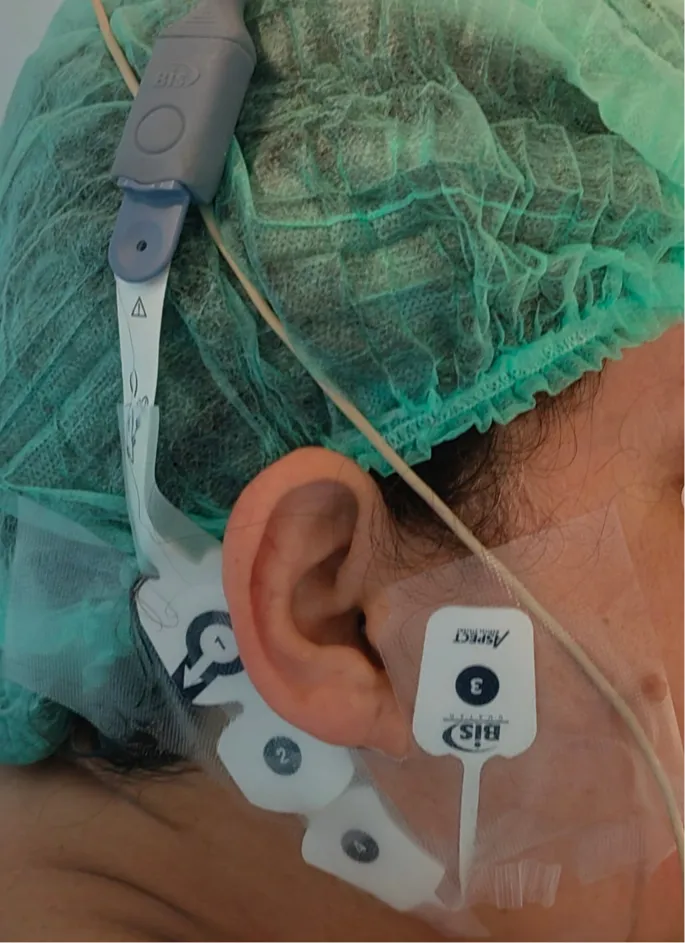
Muscle (Neuromuscular Blockade):
- Peripheral Nerve Stimulator (PNS) assesses NMB.
- Stimulation Patterns:
- Train-of-Four (TOF): T4/T1 ratio for recovery.
- Post-Tetanic Count (PTC): Deep blocks (TOF=0).
- Double Burst Stimulation (DBS): Detects residual block.
- Sites: 📌 Ulnar nerve (adductor pollicis), Facial nerve (orbicularis oculi).
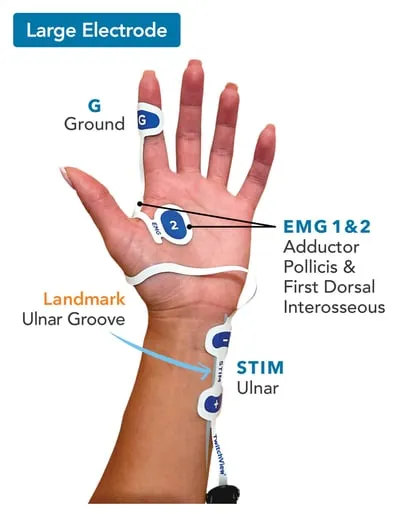
- TOF Ratio & Clinical Correlation:
TOF Ratio (T4/T1) Clinical Correlation > 0.9 Safe extubation 0.7 - 0.9 Residual weakness; diplopia < 0.7 Significant blockade; ↓ resp. function 0 (No T4) Deep block
⭐ TOF ratio > 0.9 (adductor pollicis) crucial for safe extubation, prevents post-op respiratory complications.
High‑Yield Points - ⚡ Biggest Takeaways
- Standard ASA monitoring (ECG, NIBP, SpO2, Temperature, EtCO2) is universally mandatory.
- ECG leads II & V5 are vital for detecting arrhythmias & myocardial ischemia.
- Capnography (EtCO2): gold standard for ET tube placement & monitors ventilation adequacy.
- Pulse oximetry (SpO2) monitors oxygenation; <90% signals critical hypoxemia.
- Neuromuscular monitoring (TOF ratio) guides muscle relaxant administration and reversal.
- Core temperature monitoring prevents hypothermia & detects malignant hyperthermia.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

