Lung Volumes & Mechanics - Air Chambers & Pipes
- Lung Volumes (approx. values for 70kg adult):
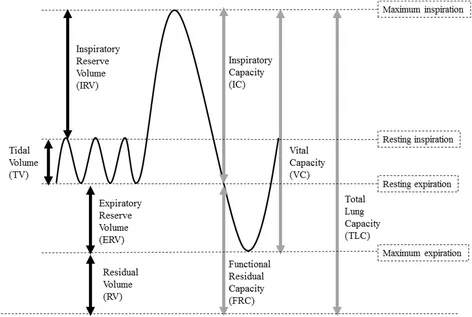
- Tidal Volume (TV): 500 mL (normal breath)
- Inspiratory Reserve Volume (IRV): 3000 mL
- Expiratory Reserve Volume (ERV): 1100 mL
- Residual Volume (RV): 1200 mL (cannot be measured by spirometry)
- Lung Capacities (sums of ≥2 volumes):
- Inspiratory Capacity (IC) = TV + IRV
- Functional Residual Capacity (FRC) = ERV + RV ≈ 2300 mL
- Vital Capacity (VC) = IRV + TV + ERV ≈ 4600 mL
- Total Lung Capacity (TLC) = VC + RV ≈ 5800 mL
- Mechanics:
- Compliance ($C = \Delta V / \Delta P$): Lung distensibility. ↓ in Fibrosis, ARDS, Pulm Edema; ↑ in Emphysema, Ageing.
- Resistance ($R = \Delta P / \text{Flow}$): Airway opposition, mainly in large airways. ↑ in Asthma, COPD, Bronchitis.
- Anatomical Dead Space: Conducting airways. ~150 mL or 2 mL/kg. 📌 Mnemonic: "Anatomic Two mL/kg".
⭐ FRC (Functional Residual Capacity) is the volume of air in lungs after normal passive exhalation; it's the equilibrium volume where inward lung elastic recoil balances outward chest wall recoil. Measured by helium dilution or body plethysmography, not spirometry alone.
Gas Exchange & Transport - Oxygen's Great Exchange
- Diffusion: Governed by Fick's Law. Depends on pressure gradient, surface area, membrane thickness, gas solubility.
- Oxygen Transport:
- Primarily bound to Hemoglobin (Hb). Small amount dissolved.
- Oxyhemoglobin Dissociation Curve (ODC): Sigmoidal. $P_{50}$ ">
⭐ Cyanide poisoning causes histotoxic hypoxia by inhibiting cytochrome c oxidase, leading to increased mixed venous oxygen saturation as tissues cannot utilize delivered oxygen.
Ventilation/Perfusion - Lung's Perfect Pair
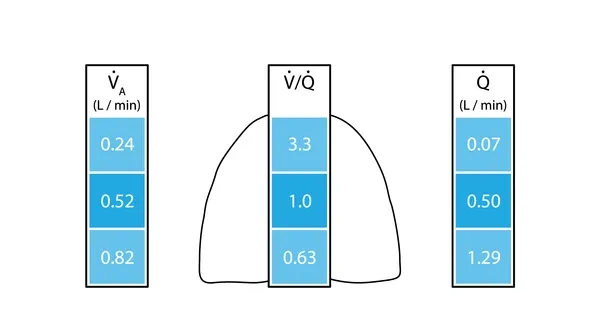
- V/Q Ratio: Balance between alveolar ventilation ($V_A$ ~4 L/min) & pulmonary blood flow ($Q$ ~5 L/min). Ideal $V_A/Q$ ≈ 0.8.
- Optimal Gas Exchange: Requires well-matched V and Q.
- V/Q Mismatch Types:
- Dead Space (V/Q > 0.8 to ∞): Ventilated, not perfused.
- Physiological = Anatomic + Alveolar.
- Causes: PE, ↓CO, emphysema. Leads to ↑$PaCO_2$.
- Shunt (V/Q < 0.8 to 0): Perfused, not ventilated.
- Causes: Atelectasis, pneumonia, ARDS. Leads to ↓$PaO_2$.
⭐ True shunt (V/Q=0) causes hypoxemia refractory to 100% O2 administration.
- Dead Space (V/Q > 0.8 to ∞): Ventilated, not perfused.
- Regional Distribution (Upright Lung):
- Apex: ↑V/Q (↓$Q$ more than ↓$V$)
- Base: ↓V/Q (↑$Q$ more than ↑$V$)
Respiratory Control & Failure - Breathless Alarms
- Neural Control:
- Medulla: DRG (Dorsal - Inspiration 📌 "DI"), VRG (Ventral - Expiration 📌 "VE", forced).
- Pons: Pneumotaxic (↑Rate, ↓Depth 📌 "Taxes breath"), Apneustic (↑Depth, ↓Rate 📌 "Aids inspiration").
- Chemical Control:
- Central Chemoreceptors: Medulla, sense CSF $H^+$ (from $CO_2$).
- Peripheral Chemoreceptors: Carotid/Aortic bodies, sense $↓PaO_2 (< \textbf{60} mmHg)$, $↑PaCO_2$, $↑H^+$.
- Respiratory Failure (RF): Inability to maintain $O_2$ or eliminate $CO_2$.
- Type I (Hypoxemic): $PaO_2 < \textbf{60} mmHg$, normal/↓$PaCO_2$. (e.g., ARDS, Pneumonia).
- Type II (Hypercapnic): $PaCO_2 > \textbf{45-50} mmHg$. (e.g., COPD, NMD).
- Alarms: Dyspnea, tachypnea, cyanosis, altered sensorium, ABG.

⭐ ARDS Berlin Criteria: Acute onset, bilateral opacities (not fully cardiac), $PaO_2/FiO_2 \le \textbf{300} mmHg$. Severity: Mild ($\textbf{201-300}$), Mod ($\textbf{101-200}$), Severe ($\le \textbf{100}$).
High‑Yield Points - ⚡ Biggest Takeaways
- ARDS: Bilateral opacities, PaO2/FiO2 < 300 mmHg, non-cardiogenic edema.
- Lung Protective Ventilation: Low tidal volumes (4-6 mL/kg PBW), Pplat < 30 cmH2O.
- PEEP: Improves oxygenation, recruits alveoli; risks barotrauma, hemodynamic compromise.
- Driving Pressure (Pplat - PEEP): Target < 15 cmH2O in ARDS for improved outcomes.
- Permissive Hypercapnia: Minimizes Ventilator-Induced Lung Injury (VILI).
- Prone Positioning: Improves V/Q matching and oxygenation in severe ARDS.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

