Ambulatory Anesthesia: Basics & Patient Preparation - Prep & Go!
- Definition: Surgery with same-day patient admission & discharge; no overnight hospital stay.
- Core Objectives:
- Rapid recovery, early ambulation.
- Minimal Post-Operative Nausea & Vomiting (PONV).
- Effective pain control.
- Early return to home.
- Patient Selection Criteria:
- Primarily ASA class I & II.
- Stable ASA III patients for selected procedures.
- Crucial factors: age, social support, travel distance to hospital.
- Surgical Procedure Suitability:
- Duration ideally < 90 minutes.
- Minimal physiological disturbance.
- Low risk of major post-op pain, bleeding, or complications.
- Preoperative Fasting (NPO) Guidelines (ASA):
- Clear liquids: 2 hours.
- Breast milk: 4 hours.
- Infant formula, non-human milk, light meal: 6 hours.
- Heavy meal (fried/fatty food, meat): 8 hours.
⭐ Clear liquids up to 2 hours before elective surgery is a key ASA guideline for adults and children.
- Premedication Goals:
- Anxiolysis: e.g., Midazolam (short-acting).
- Analgesia: e.g., Paracetamol, NSAIDs.
- PONV prophylaxis: e.g., Ondansetron, Dexamethasone.
- Aspiration prophylaxis (if high risk): e.g., H2 blockers, PPIs.
Core Anesthetic Techniques for Ambulatory Surgery - Zap & Nap Choices
Key goal: Employ short-acting agents and techniques facilitating rapid recovery and discharge.
- General Anesthesia (GA): Aim for rapid awakening, minimal Post-Operative Nausea and Vomiting (PONV).
- TIVA (Total Intravenous Anesthesia): Propofol (e.g., 2-2.5 mg/kg induction, 100-200 mcg/kg/min maintenance), Remifentanil for short-acting analgesia.
⭐ Propofol is a cornerstone for TIVA in ambulatory settings due to its rapid onset, short duration, and antiemetic properties.
- Inhalational: Sevoflurane, Desflurane (low blood:gas solubility → fast emergence).
- Airway: Supraglottic airways (LMA) preferred over Endotracheal Tube (ETT) to ↓ airway stimulation.
- TIVA (Total Intravenous Anesthesia): Propofol (e.g., 2-2.5 mg/kg induction, 100-200 mcg/kg/min maintenance), Remifentanil for short-acting analgesia.
- Regional Anesthesia (RA): Excellent analgesia, opioid-sparing, ↓ PONV.
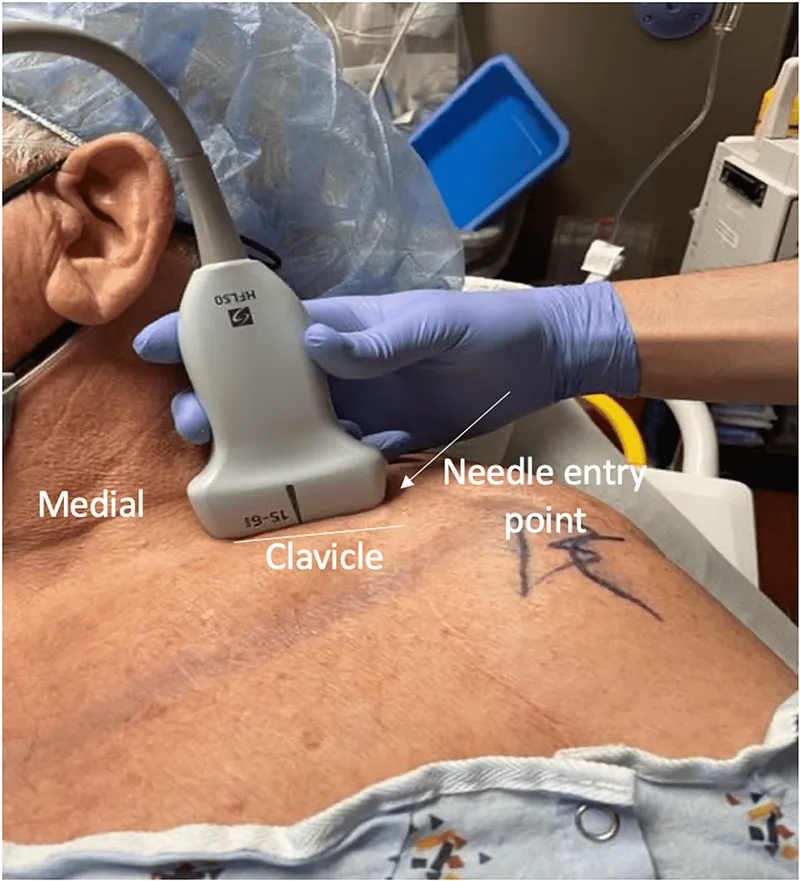
- PNBs (Peripheral Nerve Blocks): Ultrasound-guided (USG) for precision (e.g., interscalene, femoral). Single-shot or catheter.
- Central Neuraxial: Short-acting spinals (e.g., 2-Chloroprocaine 30-60 mg, low-dose Bupivacaine <7.5 mg) or titrated epidurals. Avoids GA side effects.
- Monitored Anesthesia Care (MAC): 📌 Minimal Alteration, Conscious sedation.
- Combines Local Anesthesia (LA) with IV sedation/analgesia (Midazolam 0.5-2 mg, Fentanyl 25-50 mcg, Propofol 25-75 mcg/kg/min).
- Patient responsive, maintains airway reflexes & spontaneous ventilation.
- Local Anesthesia (LA): For minor superficial procedures or as adjunct.
- Techniques: Infiltration, topical, field blocks. Often combined with MAC/light GA.
Postoperative Care & Discharge Criteria in Day Surgery - Wake & Wave
- Postoperative Care Goals:
- Swift awakening, effective symptom management.
- Multimodal analgesia (opioid-sparing preferred).
- Proactive PONV control.
- Key Discharge Criteria (PADSS ≥ 9):
- Vitals: Stable (e.g., BP/HR within 20% of baseline).
- Orientation: Alert & oriented.
- Pain: Controlled (e.g., VAS < 4/10).
- PONV: Minimal or absent.
- Mobility: Able to ambulate safely.
- Voiding: As indicated (e.g., post-spinal, urology).
- Support: Responsible adult escort, clear instructions.
⭐ The Post Anesthetic Discharge Scoring System (PADSS) is a validated tool; a score ≥ 9 (out of 10) is commonly required for discharge.
High‑Yield Points - ⚡ Biggest Takeaways
- MAC is preferred for rapid recovery & minimal side effects.
- Regional blocks offer excellent post-op analgesia & ↓ opioid needs.
- TIVA (e.g., propofol) allows fast emergence & clear-headed recovery.
- Use short-acting opioids & non-opioid analgesics to minimize PONV & hasten discharge.
- LMA often preferred over ET intubation for less airway trauma & quicker wake-up.
- Multimodal analgesia is vital for superior pain relief & fewer side effects.
- Rigorous patient selection & preoperative optimization are crucial for safety.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

