Immune Cells & Basics - Tiny Troopers Team-Up
- Lymphocytes: Key players in adaptive immunity; morphologically small, round cells with scant cytoplasm.
- T cells (Thymus-derived): Cell-mediated. All express CD3.
- Helper (CD4+): Orchestrate immune response.
- Cytotoxic (CD8+): Directly kill infected/tumor cells.
- B cells (Bone marrow-derived): Humoral immunity; produce antibodies. Express CD19, CD20.
- NK cells (Natural Killer): Innate immunity. Large granular lymphocytes.
- T cells (Thymus-derived): Cell-mediated. All express CD3.
- Macrophages: Phagocytosis, antigen presentation. From monocytes. Abundant cytoplasm, kidney-shaped nucleus.
- Dendritic Cells (DCs): Most potent APCs; link innate & adaptive. Star-shaped processes.
- Immunity Overview:
- Innate: Rapid, non-specific first line (e.g., NK cells, macrophages).
- Adaptive: Slower, specific, develops memory (e.g., T/B cells).

⭐ Key CD markers: T-cells are universally CD3+. Helper T-cells are CD4+. Cytotoxic T-cells are CD8+. B-cells are CD19+ and CD20+.
Primary Lymphoid Organs - Boot Camp & College
- Bone Marrow:
- Central hematopoietic organ; origin of all blood cells.
- Site for B lymphocyte maturation and development (antigen-independent phase).
- Self-reactive B cells eliminated via negative selection.
- Thymus:
- Bilobed organ in superior mediastinum; crucial for T lymphocyte maturation ("Thymic Education").
- Blood-Thymus Barrier: In cortex; protects developing thymocytes from circulating antigens. Formed by epithelial reticular cells, capillary endothelium, and macrophages.
- Hassall's Corpuscles: Found in medulla. Eosinophilic, concentric lamellated structures of Type VI epithelial reticular cells. 📌 Mnemonic: "Hassall's Help T-regs Survive."
⭐ Hassall's corpuscles are unique to the thymic medulla and are believed to play a role in inducing T regulatory (Treg) cell development, possibly by secreting cytokines like TSLP (Thymic Stromal Lymphopoietin).
Thymus: Cortex vs. Medulla
| Feature | Cortex | Medulla |
|---|---|---|
| Thymocytes | Densely packed, immature (CD4+CD8+) | Fewer, more mature (CD4+ or CD8+) |
| Key Processes | Positive selection, proliferation | Negative selection, T cell maturation completion |
| Epithelial Cells | Type I-IV ERCs, form blood-thymus barrier | Type V-VI ERCs, Hassall's corpuscles (Type VI) |
| Staining | Darker (basophilic) | Lighter (eosinophilic) |
Secondary Lymphoid Organs I - Nodes & Spleen Scrutiny
Lymph Node: Filters lymph; initiates adaptive immunity.
- Structure:
- Capsule: Dense CT.
- Cortex: B-cell zone. Follicles (primary/secondary with germinal centers).
- Paracortex: T-cell zone. High Endothelial Venules (HEVs) for lymphocyte entry.
- Medulla: Medullary cords (plasma cells, macrophages) & sinuses.
- Lymph Flow:

Spleen: Filters blood; removes old RBCs; immune surveillance.
- Structure:
- Capsule: With trabeculae.
- White Pulp (Immune Response):
- Periarteriolar Lymphoid Sheaths (PALS): T-cells around central artery.
- Follicles: B-cells (may show germinal centers).
- Red Pulp (Blood Filtration):
- Splenic Cords (of Billroth): Macrophages, plasma cells.
- Sinusoids: Discontinuous endothelium.
- Marginal Zone: Interface between red/white pulp; antigen trapping & presentation.
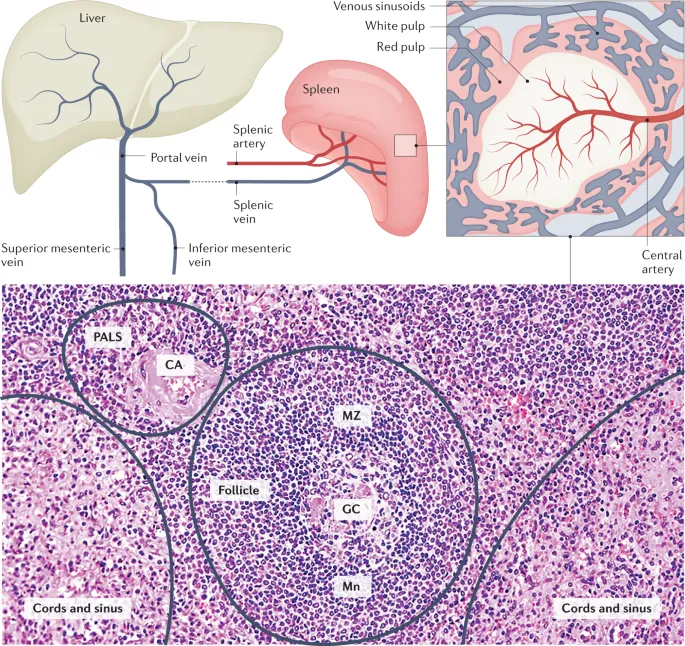
⭐ Key Cell Locations:
- Lymph Node: B cells primarily in follicles (cortex); T cells primarily in paracortex.
- Spleen: B cells in follicles (white pulp); T cells in PALS (white pulp).
Secondary Lymphoid Organs II - MALT & Mucosal Guards
- MALT (Mucosa-Associated Lymphoid Tissue):
- Diffuse, unencapsulated lymphoid aggregates in submucosa (respiratory, GI, GU tracts).
- Primary site of antigen encounter; initiates mucosal immunity.
- GALT (Gut-Associated Lymphoid Tissue):
- Peyer's Patches: Prominent in ileum.
- Contain specialized M (microfold) cells for antigen sampling.
- Dome area rich in B-lymphocytes, APCs; germinal centers present.
 ⭐ > Peyer's patches are characterized by M cells, specialized epithelial cells that transport luminal antigens to underlying immune cells.
⭐ > Peyer's patches are characterized by M cells, specialized epithelial cells that transport luminal antigens to underlying immune cells.
- Peyer's Patches: Prominent in ileum.
- Tonsils (Waldeyer's Ring): Guard pharynx.
-
📌 Epithelium: Palatine/Lingual - Stratified Squamous; Pharyngeal - Pseudostratified Columnar.
-
Comparison of Tonsil Types:
Feature Palatine Tonsil Pharyngeal Tonsil (Adenoids) Lingual Tonsil Epithelium Stratified squamous (non-keratinized) Ciliated pseudostratified columnar Stratified squamous (non-keratinized) Crypts 10-20 deep, branched Folds/pleats (no true crypts) Single, short crypt per unit Capsule Partial, thick Thin, incomplete Thin, poorly defined
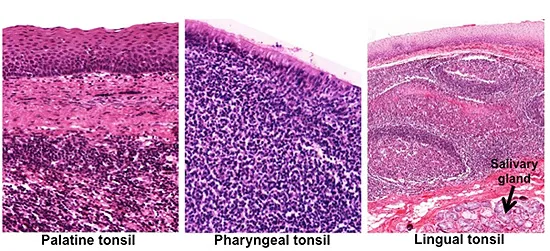
-
High‑Yield Points - ⚡ Biggest Takeaways
- Thymus: Essential for T-cell maturation; characterized by Hassall's corpuscles.
- Spleen: White pulp for immune reactions; red pulp for blood filtration.
- Lymph Nodes: Paracortex is T-cell rich; germinal centers in follicles indicate B-cell activation.
- MALT: Includes Peyer's patches (ileum) for mucosal immunity.
- Primary lymphoid organs (Bone Marrow, Thymus) are sites of lymphocyte development.
- Secondary lymphoid organs (Spleen, Lymph Nodes) initiate adaptive immune responses.
- DiGeorge Syndrome: Results from thymic aplasia, leading to severe T-cell deficiency.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

