Viral Entry & Spread - Gateway Invaders
- Portals of Entry: Resp. (Influenza), GI (Rotavirus), Skin (HPV), GU (HSV), Transplacental (Rubella).
- Key Steps:
- Attachment: Viral ligand ↔ Host cell receptor. Defines tropism (e.g., HIV gp120 to CD4).
- Penetration:
- Direct Fusion (e.g., HIV, Measles) with cell membrane.
- Endocytosis (e.g., Influenza, Adenovirus); pH-dependent uncoating.
- Uncoating: Viral genome release.
- Spread:
- Local: Cell-to-cell (syncytia: RSV, HIV); extracellular release.
- Systemic:
- Hematogenous (Viremia): Primary & secondary phases.
⭐ Viremia is the most common route for systemic viral dissemination.
- Lymphatic: To nodes, then bloodstream.
- Neural: Axonal transport (Rabies, HSV, Polio).
Cell Tropism & Damage - Target Lock Tactics
- Cell Tropism: Virus's selective affinity for specific host cells/tissues. 📌 Tropism = Susceptibility (receptors) + Permissivity (replication factors).
- Key Determinants:
- Host cell surface receptors (e.g., HIV gp120 & CD4).
- Cellular factors for viral replication (e.g., transcription factors).
- Physical accessibility, local environment (pH, temperature).
- Key Determinants:
- Mechanisms of Cell Damage (Cytopathic Effects - CPE):
- Direct Effects:
- Inhibition of host protein, RNA, DNA synthesis.
- Cell fusion (syncytia formation) e.g., Measles, RSV, HIV.
- Inclusion bodies (e.g., Negri bodies - Rabies; Cowdry type A - HSV; Owl's eye - CMV).
- Induction of apoptosis.
- Indirect (Immune-Mediated) Damage:
- Cytotoxic T-lymphocyte (CTL) killing of infected cells.
- Direct Effects:
⭐ Some viruses encode anti-apoptosis proteins to prolong cell survival for maximal viral replication (e.g., Cowpox crmA protein).
Host Response & Evasion - Immune System Showdown
- Host Defenses:
- Innate (Rapid):
- Interferons ($IFN-\alpha/\beta$): Antiviral state.
- NK cells: Kill infected cells (↓MHC-I).
- Macrophages: Phagocytosis, Ag presentation.
- Adaptive (Specific, Memory):
- Humoral (B-cells → Abs): Neutralization, opsonization, ADCC.
- Cellular (T-cells):
- CTLs (CD8+): Lyse infected cells.
- Th cells (CD4+): Coordinate response.
- Innate (Rapid):
- Viral Evasion Mechanisms: 📌 "HIDE & SEEK"
- Hiding (Latency): Herpesviruses.
- Interfering MHC presentation: Adeno, CMV (↓MHC-I).
- Decoying: Virokines/Viroceptors.
- Evolving (Antigenic variation): Influenza, HIV.
- Suppressing apoptosis.
- Encoding IFN antagonists: HCV.
- Escaping Ab neutralization.
- Killing immune cells: HIV (CD4+).
⭐ CMV (US2, US3, US6, US11) & Adenovirus (E3/19K) downregulate MHC-I to evade CTL detection.
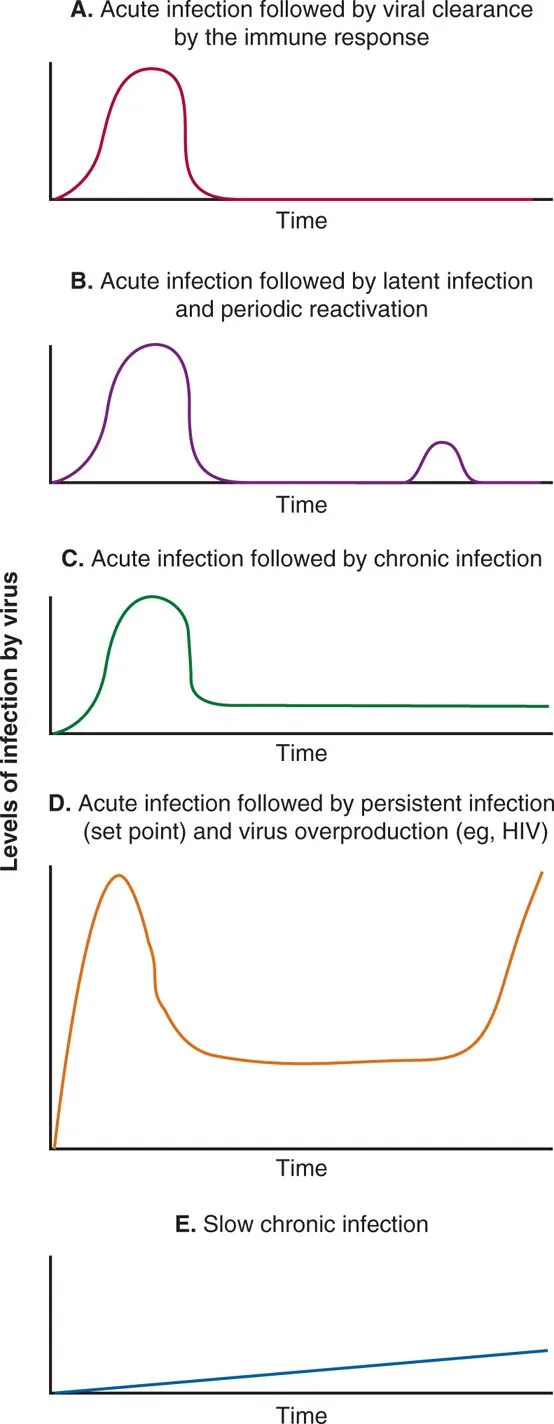
Infection Patterns & Outcomes - Viral Legacy
- Acute Infections: Rapid onset, short duration; virus cleared. E.g., Influenza, Rotavirus.
- Persistent Infections: Virus evades clearance.
- Chronic: Continuous viral shedding; long-term disease. E.g., HBV, HCV, HIV.
- Organ damage (cirrhosis, AIDS).
- Latent: Dormant virus, reactivates periodically. E.g., Herpesviruses (HSV, VZV), CMV.
- Slow: Long incubation; progressive, fatal. E.g., Measles (SSPE), Prions (CJD).
- Chronic: Continuous viral shedding; long-term disease. E.g., HBV, HCV, HIV.
- Key Outcomes:
- Oncogenesis (HPV, EBV, HTLV-1, HBV, HCV).
- Immunopathology (host response damage).
- Congenital (Rubella, CMV, Zika). 📌 Rubella, CMV, Zika: key viral teratogens.
⭐ Measles virus can cause Subacute Sclerosing Panencephalitis (SSPE), a rare, progressive, fatal neurological disease years after initial infection.
High‑Yield Points - ⚡ Biggest Takeaways
- Viral entry (e.g., fusion, endocytosis) and tissue tropism are critical initial steps.
- Cell injury results from direct cytopathic effects (CPE) or host immune-mediated damage.
- Key infection patterns include acute, chronic (persistent), and latent infections.
- Host immune responses (IFNs, CTLs) combat viruses but can cause immunopathology.
- Viruses utilize immune evasion mechanisms such as antigenic variation and latency.
- Certain viruses possess oncogenic potential, leading to cancer.
- Viremia (virus in blood) is crucial for systemic dissemination.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

