Herd Immunity: Core Concept - Shielding the Masses
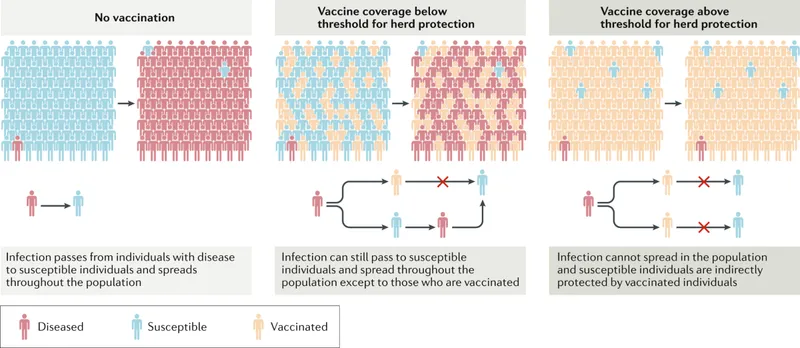
- Definition: Indirect protection from infectious disease when a high proportion of a population is immune, reducing transmission. Also known as community immunity.
- Mechanism: Immune individuals form a barrier, ↓ probability of infection spread to susceptible persons. The chain of transmission is disrupted.
- Primary Goal: Protects vulnerable individuals who cannot be vaccinated effectively.
- E.g., neonates, immunocompromised patients, individuals with vaccine contraindications.
- E.g., neonates, immunocompromised patients, individuals with vaccine contraindications.
⭐ Herd immunity protects unvaccinated individuals, including those ineligible for vaccines (e.g., newborns, immunocompromised).
Herd Immunity Threshold (HIT) - The Numbers Game
- HIT: Min. proportion of immune population to halt disease spread, protecting unvaccinated individuals.
- Determined by Basic Reproduction Number ($R_0$).
- $R_0$: Average secondary infections from one case in a fully susceptible population.
- Formula: HIT = $1 - 1/R_0$.
- Higher $R_0$ (e.g., Measles $R_0$ 12-18) means higher HIT needed (approx. 83-94%).
- Adjusting for Vaccine Efficacy (VE):
- If vaccine efficacy (VE) < 100%, required Pc = $HIT / VE$.
- E.g.: For HIT 85% & VE 90%, Pc $\approx$ 94.4% (calculated as $0.85/0.90$).
⭐ The basic reproduction number (R₀) is a key determinant of the herd immunity threshold; higher R₀ necessitates greater population immunity. The formula is HIT = 1 - 1/R₀.
Achieving Herd Immunity - Vax Power Up!
-
Concept: Indirect protection of unvaccinated; high population immunity ↓ pathogen circulation.
-
Key Metric: Herd Immunity Threshold (HIT). Formula: $1 - 1/R_0$.
- $R_0$ (Basic Reproduction Number): Higher $R_0$ requires higher HIT.
-
Achieved via: Sustained mass vaccination.
-
Factors: Pathogen $R_0$, vaccine efficacy (E), coverage, immunity duration, population mixing.
⭐ For vaccines not 100% effective, the proportion of population to be vaccinated (Pc) to achieve herd immunity is Pc = (1 - 1/R₀) / E, where E is vaccine efficacy.
- Benefits: Protects vulnerable (immunocompromised, infants, elderly).
- Challenges: Vaccine hesitancy, waning immunity, antigenic variation (e.g., influenza).

Impact & Challenges - Herd Power & Hurdles
- Herd Power (Impact):
- Shields vulnerable individuals: newborns, elderly, immunocompromised.
- Drastically ↓ pathogen circulation, breaking transmission chains.
- Aims for disease elimination (e.g., measles) or eradication (e.g., polio).
- Substantial public health & economic benefits.
- Hurdles (Challenges):
- High, sustained vaccination coverage essential (Herd Immunity Threshold: $H_{IT} = 1 - 1/R_0$).
- Vaccine hesitancy, misinformation, and logistical gaps in delivery.
- Immunity decline over time (waning immunity), necessitating boosters.
- Primary vaccine failure & less than 100% vaccine efficacy.
- Pathogen evolution (e.g., antigenic drift/shift) impacting vaccine effectiveness.
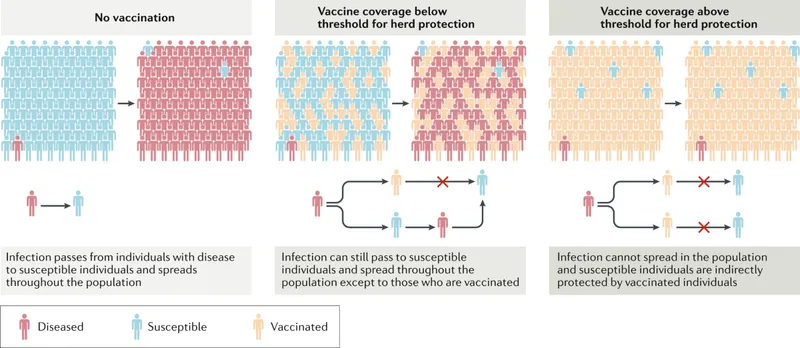
⭐ Failure to achieve or maintain herd immunity due to factors like vaccine hesitancy or waning immunity can lead to resurgence of vaccine-preventable diseases.
High‑Yield Points - ⚡ Biggest Takeaways
- Herd immunity provides indirect protection to unvaccinated individuals.
- Achieved when a critical proportion (Herd Immunity Threshold, HIT) becomes immune.
- HIT is calculated as (1 - 1/R0) x 100%, linked to the Basic Reproduction Number (R0).
- Essential for safeguarding vulnerable groups (e.g., immunocompromised, infants).
- High vaccine coverage and efficacy are prerequisites.
- Does not apply to non-communicable infections like tetanus.
- Factors like waning immunity or new pathogen variants can impact its effectiveness.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

