Monitoring Methods - Keeping Sterility Sure
Ensures sterilization efficacy. Three main types:
- Physical Monitoring:
- Charts/graphs for temperature, pressure, time.
- Verifies cycle parameters met.
- E.g., Autoclave printouts.
- Chemical Indicators (CIs):
- Color change on exposure to sterilant.
- External (e.g., autoclave tape): Shows processing, not sterility.
- Internal (e.g., Bowie-Dick test, Class 5 integrators): Placed inside packs.

- Biological Indicators (BIs):
- Gold standard for sterility assurance.
- Uses highly resistant bacterial spores.
- Steam Autoclave: Geobacillus stearothermophilus.
- Dry Heat/ETO: Bacillus atrophaeus.
- 📌 Steam = G. stearothermophilus; ETO & Dry Heat = B. atrophaeus (Remember: Evil Doctor Atrophaeus).
⭐ Biological indicators (BIs) are considered the most reliable method for verifying sterilization effectiveness as they directly assess the killing of highly resistant microorganisms.
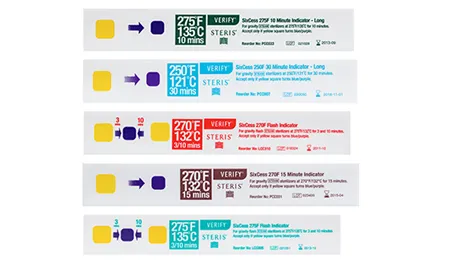
Chemical Indicators - Rainbow Reactions
- Monitor sterilization processes via chemical reactions leading to visible color changes ("rainbow reactions").
- Indicate exposure to parameters (e.g., temp, steam, time); do not confirm sterility.
- ISO 11140-1 Classes:
- Class 1 (Process): External, e.g., autoclave tape (white → black stripes). Distinguishes processed/unprocessed.
- Class 2 (Specific Use): For specific tests, e.g., Bowie-Dick test (air removal in prevacuum sterilizers).
⭐ Bowie-Dick test (Class 2) is run daily in prevacuum steam sterilizers. Checks for air leaks & inadequate steam penetration. Uniform color change indicates pass.
- Class 3 (Single Parameter): Responds to one critical variable (e.g., temperature).
- Class 4 (Multi-Parameter): Responds to ≥2 critical variables (e.g., steam & temp).
- Class 5 (Integrating): Reacts to all critical parameters; correlates with BIs.
- Class 6 (Emulating): Cycle-specific; verifies all parameters for a defined cycle.
- Provide immediate results; cost-effective.
Biological Indicators - Spore Score
Biological Indicators (BIs) provide the highest level of sterilization assurance by directly challenging the process with highly resistant bacterial spores. The "Spore Score" essentially signifies the test outcome: pass (sterilization successful) or fail (sterilization failure).
- Core Principle: If the specific sterilization method eradicates these tough spores, it's presumed effective against all other microorganisms. BIs typically contain $10^4$ to $10^6$ spores.
- Key Spores for Sterilization Methods:
| Method | Spore Organism | Typical Incubation |
|---|---|---|
| Steam (Autoclave) | Geobacillus stearothermophilus | 55-60°C |
| Dry Heat, Ethylene Oxide (ETO) | Bacillus atrophaeus | 30-37°C |
| H₂O₂ Plasma, Formaldehyde | Geobacillus stearothermophilus | 55-60°C |
| Ionizing Radiation | Bacillus pumilus | 30-37°C |

- Incubation & Readout:
- Conventional BIs: Visual color change/turbidity in 24-48 hours.
- Rapid Readout BIs: Detect enzyme activity (fluorescence), results in 1-3 hours.
- Frequency: Routinely (e.g., weekly for steam); essential for every load with implantable devices.
⭐ Geobacillus stearothermophilus is the indicator for steam autoclaves (both 121°C gravity displacement and 134°C prevacuum cycles) and also for vaporized hydrogen peroxide/plasma sterilization.
High‑Yield Points - ⚡ Biggest Takeaways
- Biological Indicators (BIs): Gold standard. G. stearothermophilus (steam/H₂O₂), B. atrophaeus (dry heat/ETO).
- Autoclave: Bowie-Dick test (prevacuum) for air removal. G. stearothermophilus spores verify kill.
- Chemical Indicators: Show exposure, not sterility. Class 5/6 CIs are most accurate.
- Physical Monitoring: Tracks cycle time, temperature, pressure; first alert to failure.
- ETO: B. atrophaeus BIs. Mandatory aeration to remove toxic ETO residues.
- BI Frequency: Weekly (ideal daily), and every implant load.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

