Quality Control in Sterilization - Sterile Shield Basics
- Sterility: Absolute state; free from all viable microorganisms (including spores and viruses).
- Sterilization: Process that eliminates or kills all forms of microbial life, including bacterial spores, to achieve sterility.
- Disinfection: Process that reduces the number of pathogenic microorganisms (excluding bacterial spores) on inanimate objects to a level considered safe.
- Antisepsis: Application of an antimicrobial chemical to living tissue/skin to inhibit or destroy microorganisms.
- Sterility Assurance Level (SAL): Probability of a single viable microorganism surviving on an item after sterilization.
- Regulatory standard for medical devices: $10^{-6}$.
⭐ The Sterility Assurance Level (SAL) of $10^{-6}$ means a one-in-a-million probability of a non-sterile item occurring after a sterilization process.
- Importance of QC:
- Ensures consistent efficacy of sterilization cycles.
- Prevents healthcare-associated infections (HAIs).
- Validates and monitors the sterilization process parameters.
- Monitoring Methods: QC involves Physical (e.g., temperature, pressure), Chemical (e.g., indicator tapes), and Biological Indicators (BIs using resistant spores).
Quality Control in Sterilization - Indicator Insights
Ensures sterilization efficacy. Key indicators:
- Physical: Cycle printouts (time, temp, pressure). Continuous.
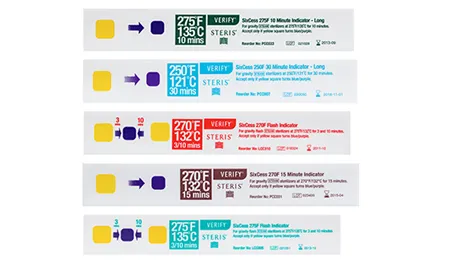
- Chemical (CIs): Color change shows exposure to conditions.
- External (Class 1): On pack (e.g., autoclave tape). Shows processing.
- Internal: Inside packs.
Class Type Purpose Example 1 Process Exposure Autoclave tape 2 Specific Test Specific function (e.g., air removal) Bowie-Dick test 3 Single-param One critical parameter Temp tube 4 Multi-param ≥2 critical parameters Steam/Temp strip 5 Integrating All critical params (mimics BI) Enzyme strip 6 Emulating All params of specific cycle Cycle strip
- Biological (BIs): Gold standard. Test kill power using spores (G. stearothermophilus - steam; B. atrophaeus - ETO/dry heat). Frequency: weekly (min. monthly).
⭐ The Bowie-Dick test is a Class 2 chemical indicator used daily for air removal & steam penetration checks in pre-vacuum steam sterilizers.
Quality Control in Sterilization - Spore Power Proof
- Biological Indicators (BIs): Gold standard, sterility assurance.
- Contain resistant bacterial spores (e.g., 10⁵-10⁶).
- Kills BIs → Kills all microbes.
- Frequency: Daily (steam), per load (implants, EtO).
Table: Biological Indicators (BIs)
| Sterilization Method | Organism | Incubation Temp & Time |
|---|---|---|
| Steam (Autoclave) | Geobacillus stearothermophilus | 55-60°C, 24-48 hrs |
| Dry Heat Oven | Bacillus atrophaeus | 30-37°C, 24-48 hrs |
| Ethylene Oxide (EtO) | Bacillus atrophaeus | 30-37°C, 24-48 hrs |
| H₂O₂ Plasma/Vapour | Geobacillus stearothermophilus | 55-60°C, 24 hrs (or rapid) |
| Formaldehyde | Geobacillus stearothermophilus | 55-60°C, 7 days |
BI Testing Process:
⭐ Biological indicators (BIs) containing spores of Geobacillus stearothermophilus are used for steam and hydrogen peroxide sterilization, while Bacillus atrophaeus spores are used for dry heat and ethylene oxide.
- Self-Contained BIs (SCBIs): Spores & media in one unit.
- Rapid Readout BIs: Enzyme activity detection; results 1-4 hrs.
- Positive Control: Unexposed BI; must show growth for test validity.
High‑Yield Points - ⚡ Biggest Takeaways
- Biological Indicators (BIs), especially spore tests, are the gold standard for sterilization assurance.
- Geobacillus stearothermophilus spores are used for steam autoclaves; Bacillus atrophaeus for ETO and dry heat.
- Chemical Indicators (CIs) verify exposure to sterilant (e.g., autoclave tape), but do not prove sterility.
- The Bowie-Dick test specifically checks for air removal and steam penetration in prevacuum steam sterilizers.
- Physical monitoring (time, temperature, pressure charts) provides real-time data but not direct proof of sterility.
- BI testing frequency: at least weekly, ideally daily; every load with implants. CIs with every pack.
- Meticulous record-keeping of sterilization cycles and QC tests is mandatory for traceability.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

