Physical Sterilization - The Germ Gauntlet
⭐ Autoclave: 121°C, 15 psi for 15-20 min is crucial for sporicidal action.
Dry Heat Sterilization - Desert Scorchers
- Mechanism: Kills by protein denaturation, oxidative damage, and toxic effects of elevated electrolyte levels.
- Methods:
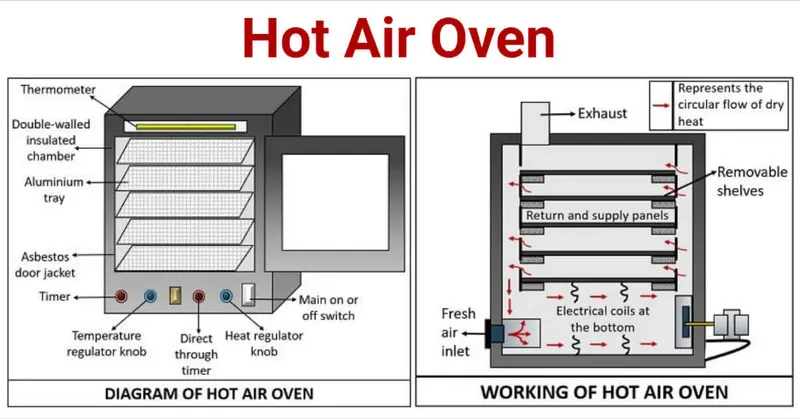
- Hot Air Oven:
- Temperatures/Times: 160°C for 2 hours; 170°C for 1 hour; 180°C for 30 minutes.
- Uses: Glassware (syringes, Petri dishes), surgical instruments (scalpels, forceps if not heat-sensitive), powders (talc, sulphonamides), oils, fats, waxes.
- Biological indicator: Spores of Bacillus atrophaeus.
⭐ Hot Air Oven: Standard holding time is 160°C for 2 hours. Used for glassware, oils, powders.
- Incineration: Burning to ashes. For contaminated dressings, animal carcasses, pathological material. Temp: 870-980°C.
- Flaming: Passing items through a Bunsen burner flame. For inoculating loops, needles, tips of forceps.
- Infrared Radiation: For rapid mass sterilization of pre-packed items like syringes and catheters.
- Hot Air Oven:
- 📌 Mnemonic: "Dry Heat Oven Sterilizes Glassware, Powders, Oils" (Dry Heat Oven, Syringes/Scalpels, Glassware, Powders, Oils).
Moist Heat (Non-Autoclave) - Steamy Subduers
- Utilizes temperatures at or below 100°C; denatures microbial proteins.
- Pasteurization: Kills non-sporing pathogens (e.g., Mycobacterium, Salmonella, Brucella).
- Holder method: 63°C for 30 min.
- Flash (HTST): 72°C for 15-20 sec.
- Used for milk, vaccines, serum. Spores survive.
- Inspissation: Thickening by evaporation.
- Heating at 80-85°C for 30 min on 3 successive days.
- For media with egg/serum (Löwenstein-Jensen, Loeffler’s serum slope).
- Boiling:
- At 100°C for 10-30 min. Kills most vegetative bacteria & viruses.
- Not sporicidal reliably; some spores resist.
- Tyndallization (Fractional Sterilization):
- Steam at 100°C for 20-30 min on 3 successive days.
- For heat-labile media (sugars, gelatin).
⭐ Inspissation is the method of choice for sterilizing heat-sensitive egg-based media like Löwenstein-Jensen (LJ) medium.
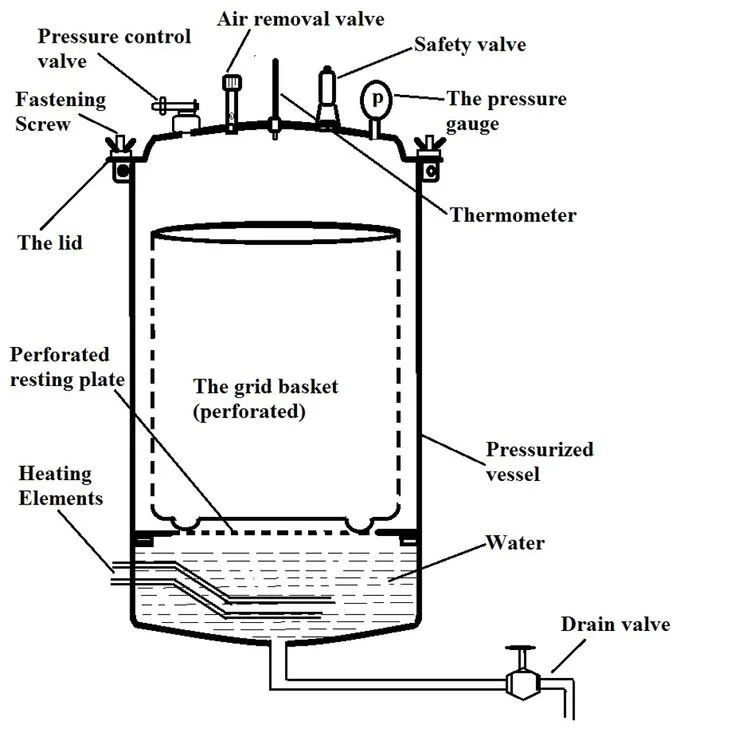
Autoclaving - Pressure Point Power
- Principle: Moist heat (steam) under ↑ pressure (↑P → ↑Boiling Point of $H_2O$).
- Mechanism: Saturated steam denatures & coagulates proteins.
- Key Parameters:
- 121°C at 15 psi (~1.05 kg/cm²) for 15-20 min.
- 134°C at 30 psi (~2.1 kg/cm²) for 3-5 min (flash; prions).
- Monitoring:
- Chemical: Autoclave tape, Bowie-Dick test (air removal).
- Biological: Geobacillus stearothermophilus spores. 📌 Gee, Steam Treats Bugs!
- Uses: Surgical instruments, media, dressings. Not for oils, powders.
⭐ Geobacillus stearothermophilus spores are the most resistant biological indicators for validating autoclave efficacy.
Radiation & Filtration - Ray & Sieve Shield
- Radiation Sterilization (Cold Sterilization)
- Non-ionizing:
- UV (260 nm): DNA damage (pyrimidine dimers). Surfaces, air (OT, LAF), water. Low penetration.
- Infrared (IR): Heats; mass sterilization (syringes).
- Ionizing (Gamma rays, X-rays, Electron beams):
- Mechanism: DNA damage (free radicals). High penetration.
- Dose: 2.5 Mrad (25 kGy).
- Uses: Disposables (gloves, syringes), drugs, food.
⭐ Gamma radiation source: Cobalt-60 ($^{60}$Co).
- Non-ionizing:
- Filtration Sterilization (Mechanical Sieving)
- Heat-labile liquids (sera, antibiotics) & air (HEPA).
- Membrane filters: Pore size 0.22 µm (bacteria), 0.01 µm (viruses).
- HEPA filters: Remove >99.97% of particles >0.3 µm (air).
High‑Yield Points - ⚡ Biggest Takeaways
- Autoclave (121°C, 15 psi, 15 min) is most reliable for surgicals & media.
- Hot Air Oven (160°C, 2 hours) sterilizes glassware, oils, and powders.
- Incineration ensures complete destruction of contaminated waste.
- Filtration sterilizes heat-labile liquids (e.g., sera) & air (HEPA filters).
- Ionizing radiation (Gamma, X-rays) sterilizes pre-packaged disposables.
- UV radiation (non-ionizing) is for surface and air disinfection.
- Tyndallization: intermittent steaming for heat-sensitive, spore-containing media.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

