BI Fundamentals - Spore Sentinels
Error generating content for this concept group: No object generated: the tool was not called.
BI Lineup - Sterilizer's Stars
Biological Indicators (BIs) are the gold standard for assuring sterilization. Key BIs include:
| Sterilization Method | BI Organism | Incubation Temp. | Positive Result (Growth) |
|---|---|---|---|
| Steam (Autoclave) | Geobacillus stearothermophilus | 55-60°C | Color change / Turbidity |
| Dry Heat (Hot Air Oven) | Bacillus atrophaeus | 30-37°C | Turbidity / Growth |
| Ethylene Oxide (EtO) | Bacillus atrophaeus | 30-37°C | Color change / Turbidity |
| $H_2O_2$ Plasma (e.g., Sterrad) | Geobacillus stearothermophilus | 55-60°C | Fluorescence / Color change |
| Formaldehyde Gas | Geobacillus stearothermophilus | 55-60°C | Color change / Turbidity |
| Ionizing Radiation | Bacillus pumilus | 30-37°C | Turbidity / Growth |
⭐ Geobacillus stearothermophilus spores (for steam, $H_2O_2$ plasma, formaldehyde) are incubated at 55-60°C. Failure of sterilization is indicated by microbial growth (e.g., pH indicator color change from purple to yellow due to acid production).
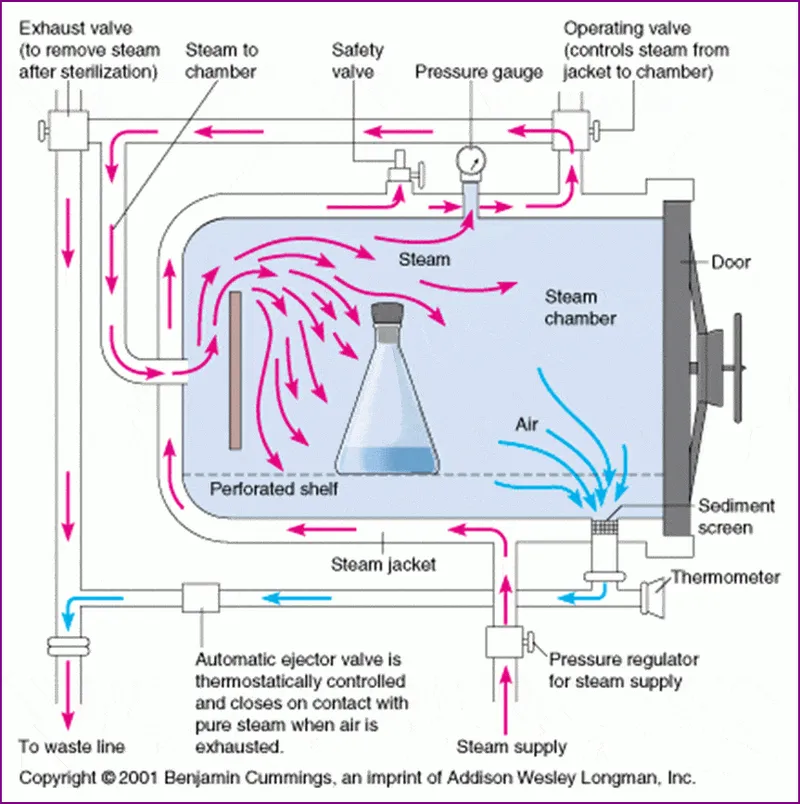
BI In Action - Test & Troubleshoot
- Placement: Coldest spots (door, bottom, center of large packs).
- Frequency:
- Steam: Weekly (min).
- ETO/Plasma: Daily.
- Implants: Every load.
- Post-repair, new sterilizer/packaging.
- Interpretation:
- Test BI: No growth = Pass. Growth = Fail.
- Control BI (unprocessed): Must show growth (validates BI viability).
- Positive BI: Indicates sterilization failure.
⭐ A single positive BI, even if subsequent tests are negative, requires thorough review of procedures & records.
High‑Yield Points - ⚡ Biggest Takeaways
- Biological Indicators (BIs) are the gold standard for confirming sterilization efficacy, directly assessing microbial killing.
- Contain a known population of highly resistant bacterial spores that challenge the sterilization process.
- Autoclave (Steam): Geobacillus stearothermophilus spores.
- Dry Heat Oven & Ethylene Oxide (ETO): Bacillus atrophaeus spores.
- Hydrogen Peroxide Plasma/Vapor: Geobacillus stearothermophilus spores.
- Ionizing Radiation: Bacillus pumilus spores.
- Successful sterilization is confirmed by no microbial growth (indicating spore inactivation) after proper incubation.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

