Lymphatic Filariasis - Elephant Legs & Blocked Drains
- Causative Agents: Wuchereria bancrofti (90%), Brugia malayi, Brugia timori.
- Vector: Mosquitoes (Culex, Anopheles, Aedes, Mansonia).
- Pathogenesis: Adult worms in lymphatics → inflammation, obstruction → lymphedema, hydrocele, elephantiasis.
- Clinical Features:
- Asymptomatic microfilaremia.
- Acute: Adenolymphangitis (ADL), filarial fever.
- Chronic: Lymphedema → Elephantiasis (legs, scrotum, arms), hydrocele, chyluria.
- Diagnosis:
- Peripheral blood smear (PBS): Microfilariae (thick smear, Giemsa stain, nocturnal sample for W. bancrofti).
- Antigen detection: Immunochromatographic card test (ICT) for W. bancrofti antigen.
- Ultrasound: Filarial dance sign (FDS) of adult worms in lymphatics.
- DEC provocation test (daytime sample after 2 mg/kg DEC).
- Treatment: Diethylcarbamazine (DEC) - kills microfilariae & adult worms. Ivermectin + Albendazole for Mass Drug Administration (MDA). 📌 "Dogs Eat Cats" (DEC).

⭐ W. bancrofti microfilariae exhibit nocturnal periodicity (peak 10 PM - 2 AM); B. malayi can be nocturnal or subperiodic. Blood collection timing is crucial for diagnosis via PBS.
Onchocerciasis - River Blindness & Skin Bumps
- Agent: Onchocerca volvulus (filarial nematode).
- Vector: Female Simulium blackfly; breeds near fast-flowing rivers.
- Pathogenesis: Microfilariae migrate through skin & eyes, causing inflammation. Adults reside in subcutaneous nodules (onchocercomas).
- Clinical Features:
- Skin: Intense itching ("craw-craw"), papular dermatitis, lichenification ("lizard skin"), depigmentation ("leopard skin"), onchocercomas, "hanging groin".
- Ocular ("River Blindness"): Punctate keratitis, sclerosing keratitis, iridocyclitis, chorioretinitis, optic atrophy.
- Diagnosis:
- Skin snips (demonstrate microfilariae).
- Nodule biopsy (adult worms).
- DEC (diethylcarbamazine) patch test.
- Treatment:
- Ivermectin: Drug of choice (microfilaricidal). Given every 6-12 months.
- Doxycycline: Targets Wolbachia endosymbionts, leading to adult worm sterility/death.
- Nodulectomy.
- Prevention: Vector control, mass Ivermectin distribution (MDA).
⭐ Ivermectin primarily kills microfilariae of O. volvulus; doxycycline targets the endosymbiotic Wolbachia bacteria, which are essential for adult worm survival and embryogenesis, thus leading to adult worm death.

Trichinellosis & Dracunculiasis - Pork Worms & Fiery Serpents
-
Trichinellosis (Trichinella spiralis - Pork Worm)
- Transmission: Ingestion of undercooked pork containing encysted larvae.
- Pathogenesis: Larvae mature in intestine → new larvae migrate to striated muscles, forming nurse cells.
- Clinical: Myalgia, fever, periorbital edema, marked eosinophilia, splinter hemorrhages.
- Diagnosis: Muscle biopsy (larvae), serology.
- Treatment: Albendazole/Mebendazole; corticosteroids for severe cases.
-
Dracunculiasis (Dracunculus medinensis - Guinea Worm/Fiery Serpent)
- Transmission: Drinking water contaminated with copepods (Cyclops) containing L3 larvae.
- Pathogenesis: Larvae mature → gravid female migrates to subcutaneous tissue (lower limbs) → painful blister → ulcer → larval release on water contact.
- Clinical: Localized pain, blister, visible emerging worm.
- Diagnosis: Clinical visualization of worm.
- Treatment: Slow, mechanical extraction (e.g., on a stick); wound care. No curative drug.
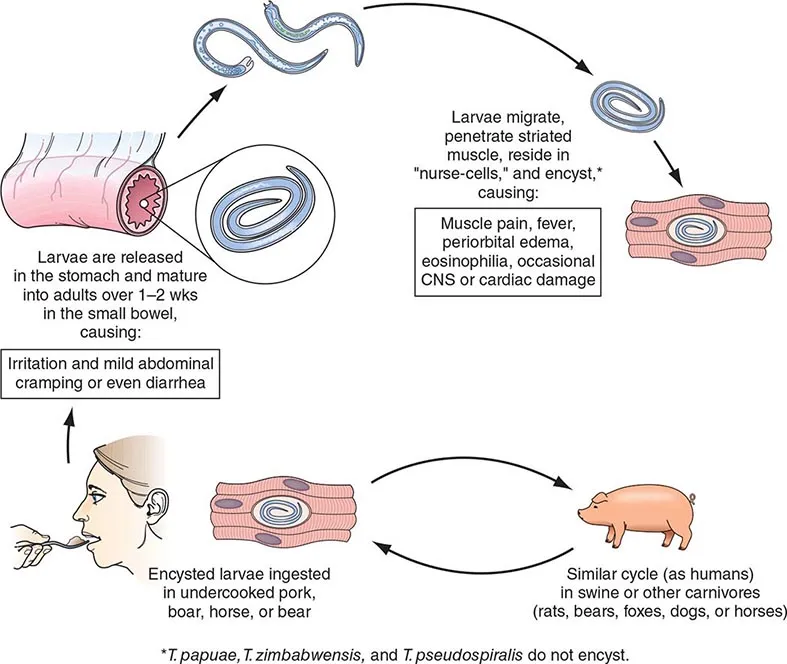
⭐ Trichinellosis: Periorbital edema and marked eosinophilia are highly suggestive clinical features; nurse cell formation in muscle is pathognomonic on biopsy.
Loiasis & Toxocariasis - Eye Worms & Wandering Larvae

- Loiasis (Loa loa)
- Vector: Chrysops spp. (deer/mango fly).
- Clinical: Fugitive Calabar swellings (transient angioedema), adult worm migration in subconjunctiva ("eye worm").
- Dx: Microfilariae in blood (diurnal periodicity), adult worm ID.
- Rx: Diethylcarbamazine (DEC).
- Toxocariasis (Toxocara canis/cati)
- Source: Ingestion of embryonated eggs from soil contaminated with dog/cat feces.
- Clinical:
- Visceral Larva Migrans (VLM): Fever, hepatomegaly, marked eosinophilia.
- Ocular Larva Migrans (OLM): Unilateral vision loss, strabismus, leukocoria.
- Dx: Serology (ELISA), marked eosinophilia. (No eggs in human stool).
- Rx: Albendazole; corticosteroids for inflammation.
⭐ OLM due to Toxocara can mimic retinoblastoma (leukocoria), a critical differential.
High‑Yield Points - ⚡ Biggest Takeaways
- Wuchereria bancrofti & Brugia malayi cause lymphatic filariasis; microfilariae show nocturnal periodicity.
- Loa loa (eye worm) causes Calabar swellings; microfilariae show diurnal periodicity; vector Chrysops.
- Onchocerca volvulus causes river blindness, dermatitis; diagnosed by skin snips; vector Simulium.
- Dracunculus medinensis (Guinea worm) emerges from painful skin ulcers; intermediate host Cyclops.
- Trichinella spiralis from undercooked pork; causes myalgia, periorbital edema, eosinophilia.
- Toxocara spp. cause Visceral Larva Migrans (VLM) and Ocular Larva Migrans (OLM).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

