Introduction & Species - Parasite Parade
Plasmodium spp. cause malaria. Key features:
| Species | RBCs Infected | Hypnozoites | Periodicity (hrs) | Gametocytes | Stippling/Other |
|---|---|---|---|---|---|
| P. falciparum | All | No | 36-48 | Crescent | Maurer's dots; Multiple rings, appliqué |
| P. vivax | Reticulocytes | Yes | 48 | Round/Oval | Schüffner's dots; Amoeboid trophozoites |
| P. ovale | Reticulocytes | Yes | 48 | Round/Oval | James'/Schüffner's dots; Fimbriated RBCs |
| P. malariae | Mature | No | 72 | Round/Oval | Ziemann's dots; Band trophozoites |
| P. knowlesi | All | No | 24 | Round/Oval | Zoonotic; Can be severe; (Stippling variable) |
⭐ P. falciparum causes most severe malaria; shows multiple ring forms & appliqué (accolé) forms.
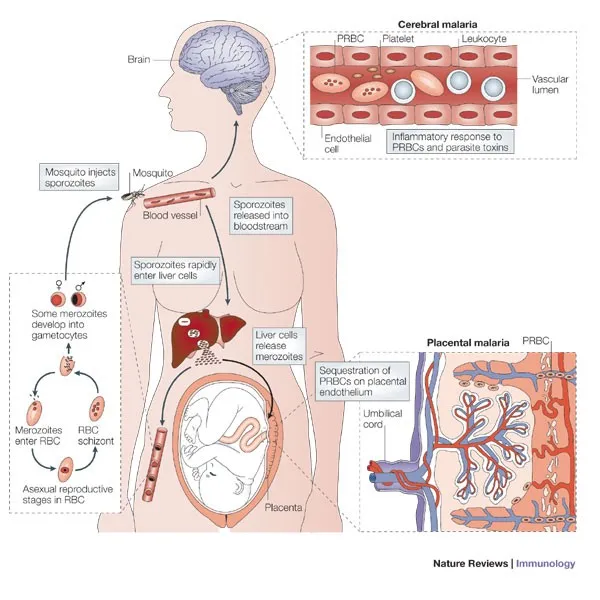
Life Cycle - Mosquito Tango
- Human Cycle (Asexual):
- Hepatic (Exo-erythrocytic) Schizogony: Anopheles injects sporozoites (infective). These travel to liver, form schizonts, then release merozoites.
- P. vivax/ovale: Hypnozoites (dormant liver stages) cause relapses.
- Erythrocytic Schizogony: Merozoites invade RBCs. Develop: trophozoite (ring stage) → schizont (multinucleated) → ruptures releasing more merozoites (causing fever). Some differentiate into gametocytes (male/female sexual forms).
- Hepatic (Exo-erythrocytic) Schizogony: Anopheles injects sporozoites (infective). These travel to liver, form schizonts, then release merozoites.
- Mosquito Cycle (Sexual - Sporogony):
- Mosquito ingests gametocytes. In gut: fertilization → zygote → ookinete → oocyst. Oocyst matures, releases sporozoites which migrate to salivary glands.

⭐ Infective stage for humans: Sporozoites. Infective stage for mosquitoes: Gametocytes.
Clinical Features & Pathogenesis - Fever Pitch
- Pathogenesis: RBC lysis → anemia, splenomegaly. Fever (TNF-α, IL-1) from schizont rupture. P. falciparum: cytoadherence (PfEMP1, knobs) → sequestration, microvascular obstruction.
- Clinical: Incubation 7-30 days. Paroxysms: cold, hot, sweating stages.
- Periodicity: Tertian (48h) - P. vivax, P. ovale, P. falciparum; Quartan (72h) - P. malariae.
- Severe Falciparum Malaria: Impaired consciousness (GCS < 11), ARDS, shock.
- Key complications: Cerebral malaria, severe anemia (Hb < 5 g/dL), hypoglycemia (< 40 mg/dL), lactic acidosis, ARDS, renal failure (Cr > 3 mg/dL), Blackwater fever.
⭐ Sequestration of parasitized RBCs in cerebral microvasculature is central to cerebral malaria pathogenesis.
Laboratory Diagnosis - Slide Sleuths
-
Microscopy (Gold Standard): Giemsa-stained thick (parasite detection) & thin smears (species ID, % parasitemia).
- Key features: RBC (size, stippling: 📌 Schüffner's: P. vivax/ovale; Maurer's clefts: P. falciparum; Ziemann's dots: P. malariae), parasite stages, gametocytes (crescent: Pf).
-
Rapid Diagnostic Tests (RDTs): Fast. Detect antigens: HRP-2 (Pf), pLDH (pan/species). Limitations: HRP-2 persistence, hrp2/3 deletions.
⭐ HRP-2 (P. falciparum specific) RDTs may stay positive weeks post-cure.
-
Other Methods: QBC; PCR (high sensitivity/specificity, speciation, drug resistance - reference labs); Serology (retrospective, not for acute).
Treatment & Prevention - Drug Duel
- Uncomplicated P. falciparum: Artemisinin-based Combination Therapies (ACTs). Chloroquine if sensitive.
- P. vivax/ovale: Chloroquine or ACT + Primaquine for radical cure (hypnozoites). ⚠️ G6PD test before Primaquine.
- Severe Malaria (all species): IV Artesunate.
- Prevention: Chemoprophylaxis (travellers); Vector control (LLINs, IRS, repellents).
⭐ IV Artesunate is the drug of choice for severe malaria, especially P. falciparum.
📌 No Primaquine if G6PD low, or hemolysis will flow!
High‑Yield Points - ⚡ Biggest Takeaways
- P. falciparum causes severe malaria; crescentic gametocytes are diagnostic.
- P. vivax & P. ovale cause relapses due to hypnozoites in the liver.
- Peripheral smear (Giemsa) showing ring forms is key for diagnosis.
- Schüffner's dots are seen in P. vivax/ovale infected RBCs.
- Maurer's clefts/dots are characteristic of P. falciparum.
- Blackwater fever is a complication of P. falciparum infection.
- ACTs (Artemisinin-based Combination Therapies) are first-line for uncomplicated falciparum malaria.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more