Leishmaniasis: Intro & Life Cycle - Sandfly's Sinister Secret
- Protozoal disease caused by genus Leishmania; transmitted by sandflies.
- Key Species & Manifestations:
- L. donovani: Visceral Leishmaniasis (Kala-azar)
- L. tropica: Cutaneous Leishmaniasis (Oriental Sore)
- L. braziliensis: Mucocutaneous Leishmaniasis (Espundia)
- Vector (India): Phlebotomus argentipes.
- Life Cycle Forms:
- Promastigote: Motile, flagellated; in sandfly (infective stage).
- Amastigote (Leishman-Donovan/LD body): Non-motile, intracellular; in vertebrate macrophages (diagnostic stage).
📌 Mnemonic: Promastigote in Phlebotomus (sandfly); Amastigote in Animal/human.
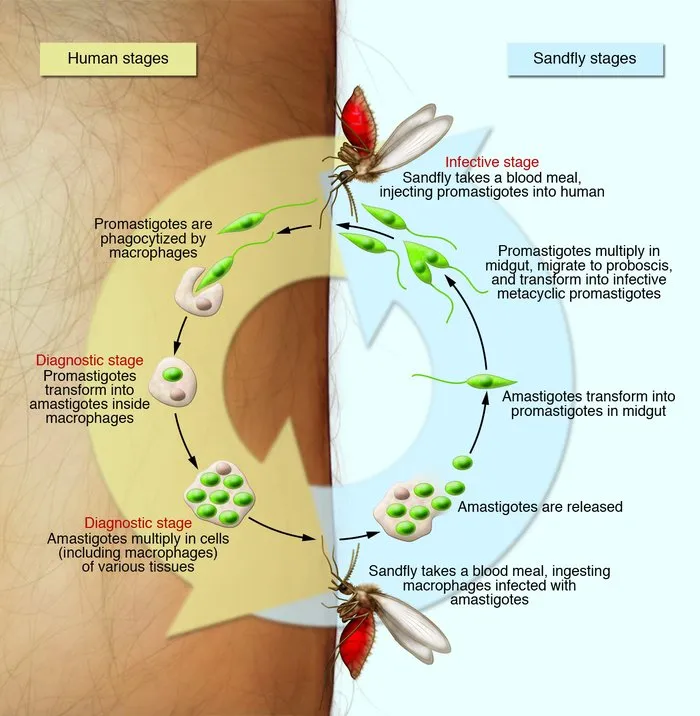
- Transmission Cycle:
- Sandfly injects promastigotes into skin.
- Macrophages phagocytose promastigotes → transform to amastigotes → multiply.
- Sandfly ingests macrophages with amastigotes during blood meal.
- Amastigotes → promastigotes in sandfly gut, migrate to proboscis.
⭐ Amastigote form (LD body) is found intracellularly in macrophages of the vertebrate host.
Leishmaniasis: Clinical Spectrums - Viscera, Skin & Scars
| Feature | Visceral (VL) / Kala-azar | Cutaneous (CL) | Mucocutaneous (MCL) | Post-Kala-azar Dermal (PKDL) |
|---|---|---|---|---|
| AKA | Kala-azar, Dumdum fever | Oriental sore, Chiclero ulcer | Espundia | Dermal leishmanoid |
| Key Sites | Spleen, Liver, Bone marrow | Skin | Naso-oro-pharyngeal mucosa | Skin |
| Manifestations | Prolonged fever (biphasic), massive Splenomegaly & Hepatomegaly, Pancytopenia, ↑Hypergammaglobulinemia, Cachexia | Chronic, painless papule → ulcer (raised border, central depression).  | Destructive mucosal lesions (nasal, oral, pharyngeal); epistaxis, septal perforation. | Hypopigmented/erythematous macules, papules, nodules (face). 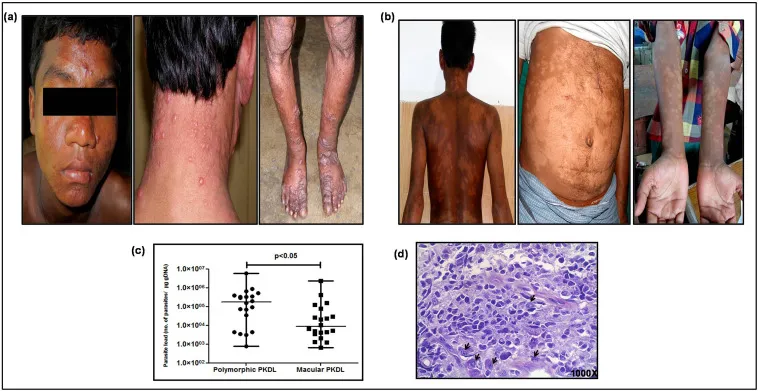 |
| Outcome/Notes | Fatal if untreated. | Self-heals (scar); can be chronic. | Progressive, disfiguring; risk of secondary infection. | Appears post-VL cure (months-years); reservoir. |
Leishmaniasis: Diagnosis Decoded - Finding Hidden Foes
- Microscopy: Gold standard for definitive diagnosis.
- Giemsa stain: Visualizes Leishman-Donovan (LD) bodies (amastigotes within macrophages).
- Specimens:
- VL: Spleen (highest yield), bone marrow, lymph node aspirates.
- CL: Skin biopsy from lesion edge / slit-skin smear.

- Culture:
- NNN medium: Cultivates promastigotes; slow (takes 1-4 weeks).
- Serology (Mainly for VL):
- rK39 strip test: Rapid, field-friendly immunochromatographic test.
- DAT (Direct Agglutination Test), ELISA: Detect antibodies.
- Montenegro Skin Test (Leishmanin Test):
- Assesses cell-mediated immunity (CMI); positive in CL & PKDL.
- Typically negative during active VL.
- Molecular Methods:
- PCR: Highest sensitivity & specificity; allows species identification.
⭐ rK39 antigen-based immunochromatographic test is highly sensitive and specific for Visceral Leishmaniasis diagnosis in field settings.
Leishmaniasis: Treatment & Control - Eradicating Endemics
Management aims to cure the patient, prevent relapse, reduce transmission, and prevent drug resistance. Treatment varies by species, clinical form, and region.
Key Drugs for Leishmaniasis:
| Drug | MOA (Simplified) | Key Doses/Regimens | Major Side Effects | Pregnancy |
|---|---|---|---|---|
| Sodium Stibogluconate (SSG) | Inhibits glycolysis & nucleic acid synth. | 20 mg/kg/day IV/IM x 28d (VL/PKDL) | Cardiotoxicity (QT), pancreatitis | Contraindicated |
| Amphotericin B (Deoxycholate) | Binds ergosterol, forms pores | 0.75-1 mg/kg/day IV x 15-20 doses | Nephrotoxicity, hypokalemia, rigors | Use if benefit > risk |
| Liposomal Amphotericin B | Ergosterol binding, targeted delivery | VL: Single dose 10 mg/kg IV; PKDL: 5 mg/kg x 6 doses (alternate days) | Infusion reactions, less nephrotoxic | Preferred |
| Miltefosine | Affects cell signaling, apoptosis | 50-100 mg/day PO x 28d (VL) | GI upset, teratogenicity | Contraindicated |
| Paromomycin | Aminoglycoside (protein synth. inhib.) | 11 mg/kg/day IM x 21d (VL); Topical for CL | Ototoxicity, nephrotoxicity, injection pain | Avoid (limited data) |
- Drug Resistance: Growing concern, especially with antimonials. Requires monitoring and combination therapy considerations.
- Control (NVBDCP, India):
- Early case detection & complete treatment.
- Integrated vector management (IRS with DDT).
- Kala-azar elimination targets (reducing annual incidence <1/10,000 population at block level).
High‑Yield Points - ⚡ Biggest Takeaways
- Transmitted by female Phlebotomine sandflies; L. donovani causes Kala-azar (Visceral Leishmaniasis).
- Infective form: Promastigote (sandfly); Diagnostic form: Amastigote (LD bodies) in macrophages.
- Kala-azar: Features prolonged fever, massive splenomegaly, pancytopenia, hypergammaglobulinemia.
- PKDL: Post-Kala-azar Dermal Leishmaniasis involves skin lesions post-VL treatment.
- Diagnosis: LD bodies in splenic/bone marrow aspirates; rk39 antigen test for VL.
- Treatment: Liposomal Amphotericin B (drug of choice for VL); Miltefosine (oral).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

