Sample Collection & Processing - First Steps Crucial
- Timing is key: Collect samples when parasite numbers are highest (e.g., nocturnal blood for filariasis, early morning stool for some helminths).
- Freshness matters: Examine immediately or use appropriate preservatives (e.g., PVA, SAF, 10% formalin for stool).
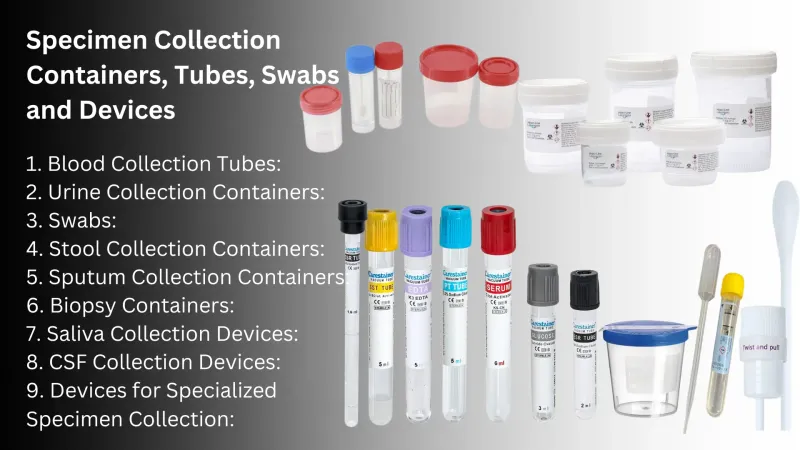
- Proper container: Sterile, leak-proof, wide-mouthed for stool; anticoagulant (EDTA) for blood.
- Adequate quantity: Sufficient sample ensures detection (e.g., 3 stool samples over several days for intermittent shedding).
- Labeling: Patient name, ID, date, time of collection.
⭐ For suspected Acanthamoeba keratitis, corneal scrapings or biopsy are preferred over contact lens solution, though both can be tested using culture or PCR.
- Processing: Concentration techniques (sedimentation, flotation) for stool; thick/thin smears for blood; CSF centrifugation for CNS parasites.
Microscopic Examination - Seeing is Believing
Microscopy: cornerstone for identifying parasites via morphology, motility, staining.
- Wet Mounts: Rapid, initial assessment.
- Saline (0.85%): Detects motility (e.g., Trichomonas), ova, larvae, cysts.
- Iodine (Lugol's): Stains glycogen, cyst nuclei (Entamoeba differentiation).
- Permanent Stained Smears: For detailed morphology & species identification.
- Giemsa: Blood parasites (Malaria, Babesia, Trypanosomes, Leishmania, Microfilaria); tissue protozoa (Toxoplasma).
- Trichrome: Intestinal protozoa (cysts, trophozoites); good nuclear detail.
- Modified Acid-Fast (MAF): Coccidian parasites (Cryptosporidium, Cyclospora, Cystoisospora oocysts).
- Iron Hematoxylin: Excellent protozoan morphology, nuclear details.
- Fluorescence Microscopy:
- Calcofluor White: Binds chitin (Microsporidia spores, Acanthamoeba cysts).
- Quantitative Techniques:
- Kato-Katz: Standardized method for helminth egg counts (Schistosoma, STH) in feces.
⭐ Giemsa stain is crucial for malaria diagnosis, revealing parasite stages (rings, trophozoites, schizonts, gametocytes) in RBCs; note Schüffner's dots (P. vivax/ovale), Maurer's clefts (P. falciparum).

Immunological & Molecular Methods - Beyond the Scope
- Immunodiagnostics: Detect parasite antigens or host antibody responses.
- ELISA, IFA: Sero-diagnosis (e.g., toxoplasmosis, amoebic liver abscess), epidemiological surveys.
- ICTs: Rapid, point-of-care results; some routine (malaria), others specialized.
- Western Blot: Confirmatory for specific infections (e.g., cysticercosis).
- Molecular Techniques: Target parasite nucleic acids (DNA/RNA) with high precision.
- PCR: High sensitivity/specificity. For low parasitemia, speciation, drug resistance.
- DNA Probes, Sequencing: Advanced research, genotyping, epidemiological tools.
- Context: For complex cases, research, public health surveillance; complement traditional methods.
⭐ PCR excels in diagnosing infections with minimal parasites (e.g., cerebral malaria from CSF) and differentiating similar species.
Special Techniques & Culture - Uncommon but Key
- Xenodiagnosis: Detects Trypanosoma cruzi (Chagas); uninfected triatomine bugs feed on patient.
- Animal Inoculation: Susceptible animals (mice, hamsters) for Toxoplasma, Leishmania, Trypanosoma.
- Culture Methods:
- NNN Medium: Biphasic; for Leishmania (amastigotes → promastigotes).
- Harada-Mori Culture: Filter paper method for hookworm, Strongyloides (rhabditiform → filariform larvae).
- Baermann Technique: Larval recovery (Strongyloides) from feces using warm water.
⭐ NNN medium (Novy-MacNeal-Nicolle) is a biphasic medium primarily used for cultivating Leishmania species.
High‑Yield Points - ⚡ Biggest Takeaways
- Stool examination (microscopy, concentration) is cornerstone for intestinal protozoa & helminths.
- Kato-Katz technique for quantitative egg counts (e.g., Schistosoma, hookworm).
- Peripheral blood smears (Giemsa/Leishman) are vital for malaria, filariasis, trypanosomiasis.
- Serological tests (ELISA, IFA) detect antibodies/antigens, crucial for tissue parasites (e.g., Toxoplasma, Echinococcus).
- Molecular methods (PCR) offer high sensitivity/specificity, especially for cryptic infections or speciation.
- Culture is selective: Leishmania (NNN medium), Trichomonas vaginalis, Acanthamoeba.
- Biopsy and aspirate examination are key for diagnosing tissue-dwelling parasites like Leishmania or Toxoplasma in specific sites.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

