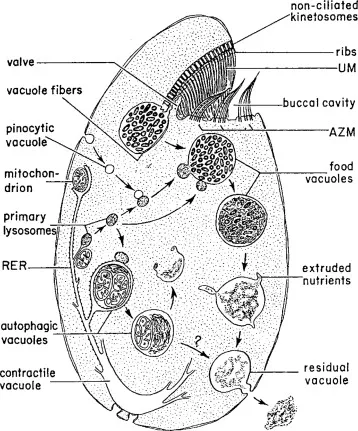
Intestinal Protozoa Overview - Gut Invaders Intro
- Microscopic, unicellular eukaryotic parasites colonizing human intestines, causing a spectrum of gastrointestinal diseases.
- A major global health burden, prevalent in regions with poor sanitation and contaminated water sources.
- Pathogenesis: mucosal adherence/invasion, toxin production, host inflammation, nutrient malabsorption.
- Key groups by motility:
- Amoebae (e.g., Entamoeba): use pseudopods.
- Flagellates (e.g., Giardia): possess flagella.
- Ciliates (e.g., Balantidium): use cilia.
- Apicomplexa (Sporozoa; e.g., Cryptosporidium): complex life cycles, apical complex.
⭐ Most intestinal protozoa transmit fecal-orally, typically via ingestion of resistant cysts or oocysts.
Entamoeba histolytica - Amoebic Menace
- Infective form: Cyst (quadrinucleate); Invasive form: Trophozoite.
- Transmission: Feco-oral route.
- Pathology: Flask-shaped ulcers in colon. 📌 Mnemonic: "Amoeba digs a FLASK to HIDE".
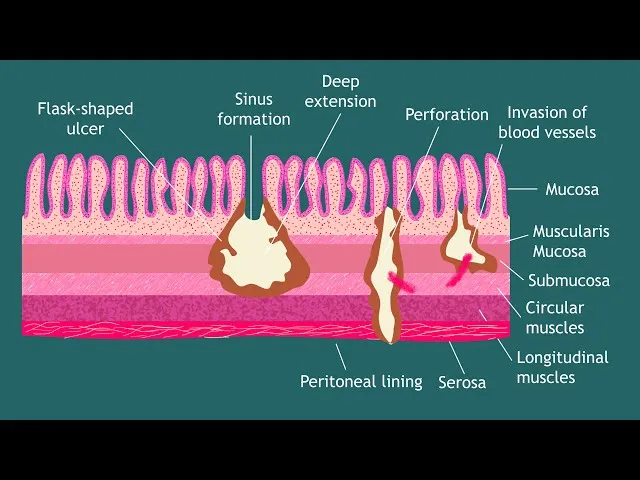
- Clinical Syndromes:
- Intestinal: Asymptomatic carriage; Amoebic dysentery (blood & mucus).
- Extra-intestinal: Amoebic liver abscess (RUQ pain, fever; "anchovy sauce" pus).
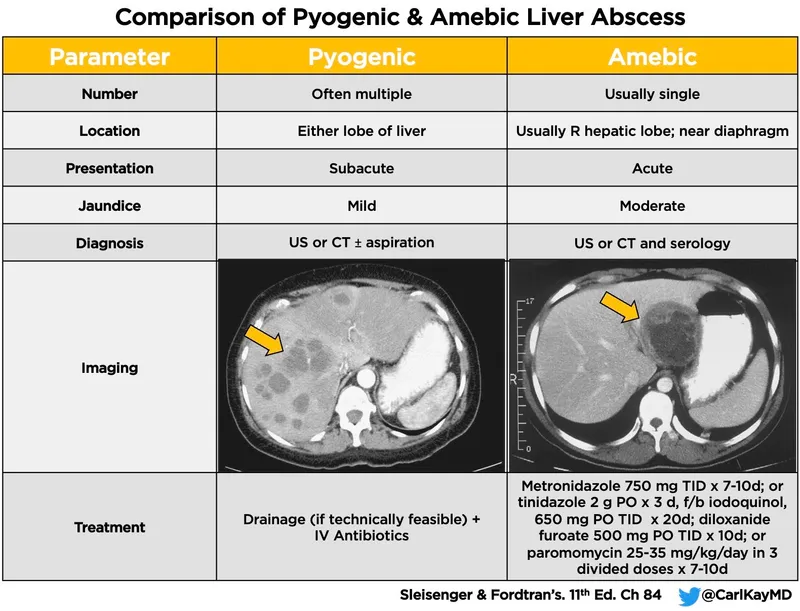
- Diagnosis:
- Microscopy: Trophozoites with ingested RBCs in stool/biopsy; Cysts in stool.
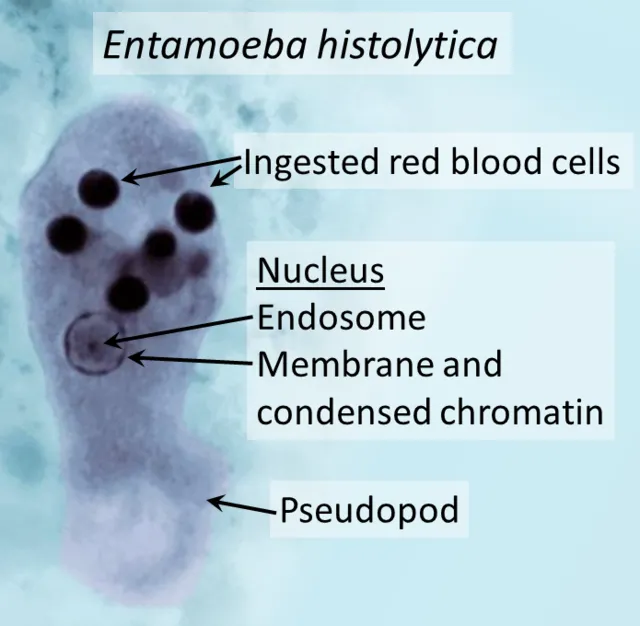
- Antigen detection in stool; Serology for invasive disease.
- Microscopy: Trophozoites with ingested RBCs in stool/biopsy; Cysts in stool.
- Treatment: Metronidazole (tissue amoebicide) followed by a luminal amoebicide (e.g., Diloxanide furoate).
⭐ Ingested RBCs in the trophozoite stage is diagnostic for E. histolytica.
Giardia lamblia - Beaver Fever Blues
- Flagellated protozoan; causes giardiasis ("Beaver Fever"). Most common intestinal protozoan in US.
- Forms:
- Trophozoite: Pear-shaped, binucleate (owl-eye), 4 pairs flagella. Motility: 📌 "Falling leaf".

- Cyst: Oval, 4 nuclei. Infective, environmentally resistant. Transmitted via contaminated water.
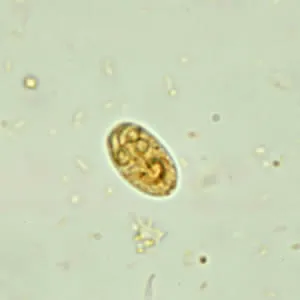
- Trophozoite: Pear-shaped, binucleate (owl-eye), 4 pairs flagella. Motility: 📌 "Falling leaf".
- Pathogenesis: Attaches to duodenal/jejunal mucosa → villous blunting, malabsorption (fat, vitamins A, D, E, K, B12).
- Clinical: Non-bloody, foul-smelling diarrhea (steatorrhea), cramps, bloating, flatulence, weight loss.
⭐ Giardiasis is known for causing foul-smelling steatorrhea and malabsorption.
- Diagnosis: Stool O&P (cysts/trophozoites), ELISA (stool antigen), string test (Entero-test).
- Treatment: Metronidazole, Tinidazole, Nitazoxanide. Consider lactose intolerance post-infection.
Intestinal Coccidia - Tiny Gut Wreckers
- Opportunistic protozoa causing diarrhea, severe in immunocompromised (CD4 < 200 cells/µL).
- Diagnosis: Oocysts in stool via Modified Acid-Fast Stain (MAFS). 📌 "Crypto, Cyclo, Cysto are Acid-Fast".
| Feature | Cryptosporidium spp. | Cystoisospora belli | Cyclospora cayetanensis |
|---|---|---|---|
| Oocyst Size (µm) | 4-6 (Small, round) | 20-30 (Large, oval) | 8-10 (Intermediate, round) |
| MAFS | Red/Pink (variable) | Red/Pink (uniform) | Red/Pink (variable) |
| Transmission | Waterborne | Fecal-oral | Imported produce |
| Clinical | Profuse watery diarrhea | Chronic diarrhea, malabsorption | Prolonged watery diarrhea |
| Treatment | Nitazoxanide; HAART | TMP-SMX | TMP-SMX |
⭐ Cryptosporidium parvum causes severe, chronic diarrhea in AIDS patients, especially with CD4 < 100 cells/µL.
Other Notable Gut Protozoa - Rare But Relevant
- Balantidium coli:
- Largest protozoan, only pathogenic ciliate. Reservoir: Pigs.
- Dysentery-like illness. Trophozoite: kidney-bean shaped macronucleus.

- Cystoisospora belli (Isospora belli):
- Immunocompromised (AIDS, CD4 < 200): chronic watery diarrhea.
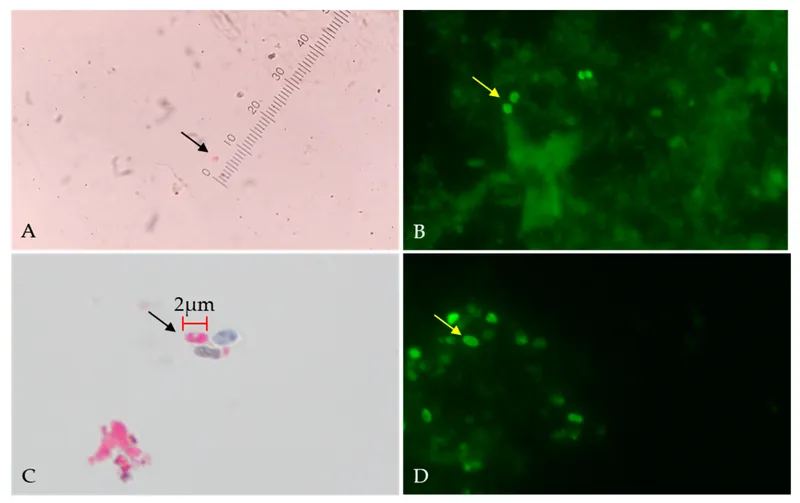
- Oocysts in stool (modified Acid-Fast Stain positive, autofluorescent).
- Sarcocystis spp.:
- Intestinal sarcocystosis (from undercooked beef/pork) or muscular sarcocystosis.
- Intestinal form: often asymptomatic or mild GI symptoms.
- Microsporidia (e.g., Enterocytozoon bieneusi, Encephalitozoon intestinalis):
- Obligate intracellular fungi (reclassified). Immunocompromised (AIDS): chronic diarrhea.
- Small spores seen with special stains (e.g., Chromotrope R).
⭐ Balantidium coli is the largest intestinal protozoan and the only ciliate pathogenic to humans.
High‑Yield Points - ⚡ Biggest Takeaways
- Entamoeba histolytica: Flask-shaped ulcers, liver abscess (anchovy sauce), ingested RBCs in trophozoites.
- Giardia lamblia: Steatorrhea, malabsorption, falling leaf motility; commonest protozoal diarrhea.
- Cryptosporidium parvum: Severe watery diarrhea in AIDS (CD4 < 100); modified acid-fast stain for oocysts.
- Cyclospora cayetanensis: Prolonged watery diarrhea; oocysts are autofluorescent.
- Isospora belli: Chronic diarrhea in immunocompromised; oval oocysts on modified acid-fast stain.
- Balantidium coli: Largest protozoan, only pathogenic ciliate, pig association, causes dysentery.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more