Intro to Superficial Mycoses - Surface Fungal Foes
- Fungal infections limited to the outermost layers of skin, hair, and nails (stratum corneum, hair shaft, nail plate).
- Caused by dermatophytes and non-dermatophyte molds (e.g., Malassezia, Piedraia, Trichosporon).
- Primarily cosmetic; minimal inflammation or tissue destruction.
- Transmission: direct contact with infected individuals, animals, or fomites.
- Diagnosis: clinical appearance, KOH microscopy, Wood's lamp.
⭐ Superficial mycoses generally do not elicit a significant host immune response because they are confined to the non-living, keratinized layers of skin and hair.
Pityriasis Versicolor - Skin's Color Chaos
- Causative Agent: Malassezia furfur (lipophilic yeast, normal skin flora).
- Mechanism: Malassezia produces dicarboxylic acids (e.g., azelaic acid) that inhibit tyrosinase, leading to altered pigmentation.
- Clinical Features:
- Well-demarcated, hypo- or hyperpigmented, or erythematous macules and patches.
- Fine, branny scales (furfuraceous scaling), often elicited by scraping (Besnier's sign).
- Common sites: Trunk, upper arms, neck, abdomen (sebaceous gland-rich areas).
- Usually asymptomatic; mild pruritus may occur.
- Predisposing Factors: Warm, humid climate; oily skin; hyperhidrosis; immunosuppression; malnutrition.
- Diagnosis:
- KOH mount (10-20%): Characteristic "spaghetti and meatballs" appearance (short, curved septate hyphae and clusters of yeast cells).
- Wood's lamp: Yellow-green to golden-yellow fluorescence (due to pteridine pigments).

- Treatment:
- Topical: Selenium sulfide (2.5%), ketoconazole shampoo/cream, ciclopirox, terbinafine solution.
- Systemic (for extensive/recurrent cases): Itraconazole, fluconazole.
⭐ The characteristic 'spaghetti and meatballs' appearance (hyphae and yeast cells) of Malassezia furfur on KOH mount is pathognomonic for Pityriasis versicolor.
Tinea Nigra & Piedras - Dark Stains & Hair Stones
Tinea Nigra
- Causative Agent: Hortaea werneckii (dematiaceous fungus).
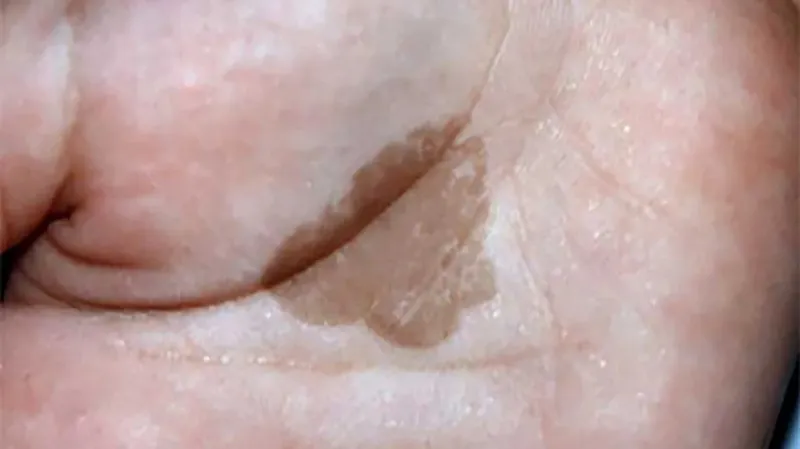
- Clinical: Asymptomatic, solitary, flat, dark brown/black macule. Non-inflammatory, non-scaly.
- Site: Palms (classic), soles.
- Diagnosis: KOH mount (pigmented hyphae, budding cells).
- Treatment: Topical antifungals (azoles, terbinafine), Whitfield's ointment.
⭐ Tinea nigra, caused by Hortaea werneckii, presents as a non-inflammatory, non-scaly, dark brown to black macule, often on the palms, and must be differentiated from melanocytic nevi or melanoma.
Piedras (Hair Stones)
- Fungal infection forming nodules on hair shafts.
| Feature | Black Piedra | White Piedra |
|---|---|---|
| Causative Agent | Piedraia hortae | Trichosporon spp. |
| Nodule Color/Texture | Black, hard, gritty, adherent | White/yellow, soft, detachable |
| Common Hair Sites | Scalp | Axillary, pubic, beard, scalp |
| Key Microscopic Feature | Ascospores present | Arthroconidia, blastoconidia |
| Treatment | Haircut, topical antifungals | Haircut, topical antifungals |
Lab Dx & Rx Summary - Fungal ID & Aid
⭐ Direct microscopic examination of clinical specimens (skin scrapings, plucked hairs) using a KOH wet mount is the most rapid and cost-effective method for diagnosing superficial mycoses.
Key investigations include KOH mount, culture (SDA; Malassezia needs lipid), and Wood's lamp. Summary:
| Mycosis | KOH Findings | Wood's Lamp | Key Rx (Topical; Systemic if severe) |
|---|---|---|---|
| Pityriasis Versicolor | "Spaghetti & meatballs" (hyphae & yeast) | Yellow-green | Ketoconazole shampoo, SeS$_2$; Oral azoles |
| Tinea Nigra | Pigmented (brown-black) hyphae | Negative | Topical azoles, Whitfield's oint. |
| White Piedra | Soft, white nodules; arthroconidia | Negative | Shave hair; Topical azoles |
| Black Piedra | Hard, black nodules; ascospores | Negative | Shave hair; Topical terbinafine |
High‑Yield Points - ⚡ Biggest Takeaways
- Malassezia furfur causes Pityriasis versicolor; KOH shows "spaghetti and meatballs" appearance.
- Pityriasis versicolor lesions exhibit yellow-green fluorescence under Wood's lamp.
- Hortaea werneckii is the causative agent of Tinea nigra, presenting as dark macules on palms/soles.
- Piedraia hortae causes Black piedra, characterized by hard, dark nodules on hair shafts.
- Trichosporon species are responsible for White piedra, forming soft, pale nodules on hair.
- Superficial mycoses are non-invasive, strictly limited to the stratum corneum or outermost hair/nail layers.
- Treatment typically involves topical antifungal agents like azoles or selenium sulfide for efficacy and safety.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

