Intro: SubQ Mycoses - Sneaky Skin Fungi
- Fungal infections affecting dermis, subcutaneous tissues, often extending to muscle/fascia.
- Characterized by slow, chronic progression; generally localized, rarely disseminate.
- Caused by fungi commonly residing in soil or on vegetation (saprophytes).
- Mode of entry: Traumatic implantation of fungal spores/hyphae into skin.
⭐ Subcutaneous mycoses are typically acquired through traumatic implantation of fungal elements into the skin, often from soil or vegetation.
Sporotrichosis - Rose Gardener's Peril
- Organism: Sporothrix schenckii (dimorphic: mold in cold, yeast in heat).
- Transmission: Traumatic inoculation from soil/plants (e.g., rose thorns 📌 "Rose Gardener's Disease").
- Clinical (Lymphocutaneous type - most common):
- Initial lesion: painless papule/nodule at inoculation site, may ulcerate.
- Follows lymphatic drainage: linear chain of subcutaneous nodules ("sporotrichoid spread").
- Diagnosis:
- Culture (Sabouraud Dextrose Agar, SDA): thermal dimorphism (yeast at 37°C, mycelial/mold at 25°C).
- Biopsy/Microscopy: Cigar-shaped budding yeasts; Asteroid bodies (Splendore-Hoeppli phenomenon - Ag-Ab complexes).
- Treatment: Itraconazole (Drug of Choice). Saturated Solution of Potassium Iodide (SSKI) for fixed cutaneous. Amphotericin B for severe/disseminated cases.
⭐ Sporothrix schenckii typically causes a lymphocutaneous infection, with nodules appearing along lymphatic channels.
 Mnemonic: "Sporothrix schenckii typically causes a lymphocutaneous infection, with nodules appearing along lymphatic channels."
Mnemonic: "Sporothrix schenckii typically causes a lymphocutaneous infection, with nodules appearing along lymphatic channels."
Chromoblastomycosis - Copper Penny Culprits
- Etiology: Dematiaceous (pigmented) fungi; Fonsecaea pedrosoi (most common), Phialophora verrucosa, Cladophialophora carrionii.
- Transmission: Traumatic inoculation of fungal elements from soil/vegetation.
- Clinical: Chronic, slowly progressive. Verrucous, warty, cauliflower-like nodules/plaques. "Black dots" (hemorrhagic points) on surface. Usually on lower limbs.
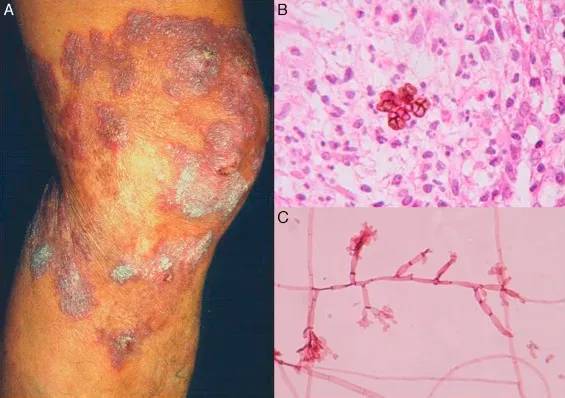
- Diagnosis:
- Microscopy (KOH/biopsy): Pathognomonic Medlar bodies (sclerotic cells, muriform cells, 'copper pennies') - thick-walled, pigmented, septate cells.
⭐ The presence of Medlar bodies (sclerotic cells, 'copper pennies') in tissue biopsy is diagnostic for Chromoblastomycosis.
- Treatment: Itraconazole, terbinafine; surgery, cryotherapy, local heat. Often refractory to treatment.
Mycetoma - Grainy Discharge Drama
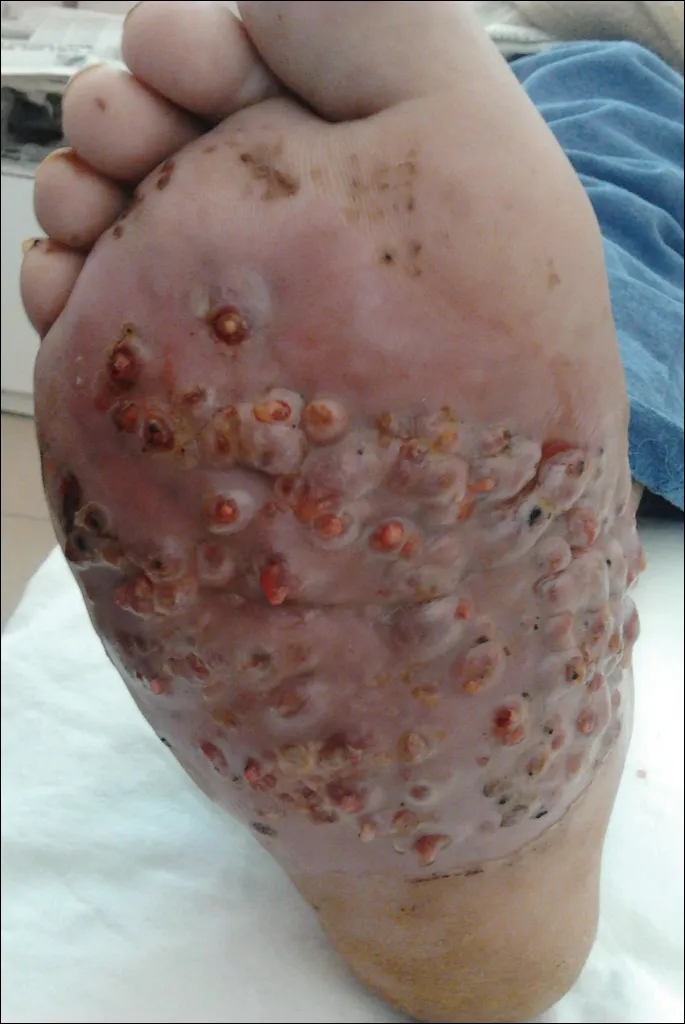
- Chronic granulomatous infection: skin, subcutaneous tissue, fascia, bone.
- 📌 Triad: Tumefaction (swelling), Draining Sinuses, Granules (grains).
- Grains: Visible colonies; color aids diagnosis.
- Eumycetoma: Larger grains; poorer medical response, often needs surgery.
- Actinomycetoma: Smaller grains; better response to prolonged antibiotics.
⭐ Mycetoma is characterized by the clinical triad of tumefaction, draining sinuses, and the presence of granules (grains).
Other Mycoses - SubQ Rarities
- Phaeohyphomycosis
- Etiology: Dematiaceous (pigmented) fungi (e.g., Exophiala, Wangiella).
- Clinical: Solitary cysts, nodules, plaques; disseminated in immunocompromised.
- Diagnosis: Pigmented (brown) septate hyphae in tissue.
- Lobomycosis (Lobo's Disease)
- Etiology: Lacazia loboi.
- Clinical: Chronic keloidal, verrucous skin lesions (ears, limbs).
- Diagnosis: Chains of yeast-like cells ("string of beads"). Amazon basin endemic.
- Rhinosporidiosis
- Etiology: Rhinosporidium seeberi (aquatic protist).
- Clinical: Polypoidal, friable, vascular "strawberry-like" nasal/ocular masses.
- Diagnosis: Large, thick-walled sporangia with numerous endospores.

⭐ Rhinosporidiosis, caused by Rhinosporidium seeberi, typically presents as friable, polypoidal masses in the nose and nasopharynx containing large sporangia with endospores.
High‑Yield Points - ⚡ Biggest Takeaways
- Sporotrichosis: "Rose gardener's disease", lymphocutaneous spread, cigar-shaped yeasts, asteroid bodies.
- Chromoblastomycosis: Sclerotic bodies (copper pennies), warty lesions, caused by dematiaceous fungi.
- Mycetoma: Granules in discharge, tumefaction, draining sinuses; distinguish eumycetoma (fungal) from actinomycetoma.
- Phaeohyphomycosis: Caused by dematiaceous fungi with pigmented hyphae in tissue.
- Rhinosporidiosis: Nasal/ocular polyps with large sporangia and endospores.
- Diagnosis: Direct microscopy (KOH, biopsy) and culture are crucial.
- Treatment: Often itraconazole; surgery may be needed_._
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

