Opportunistic Fungi - Sneaky Invaders

- Fungi causing disease primarily in immunocompromised individuals; usually harmless in healthy hosts.
- Sources: Endogenous (normal flora) or exogenous (environment).
- Major Risk Factors:
- Neutropenia (ANC <500/μL)
- HIV/AIDS (CD4 <200/μL)
- Immunosuppressive drugs (corticosteroids, chemotherapy)
- Organ transplantation
- Broad-spectrum antibiotics
- Indwelling catheters
- Diabetes Mellitus
⭐ Candida albicans is the most frequent opportunistic fungal pathogen, capable of causing a wide spectrum of diseases from superficial to systemic infections.
Candida Infections - Yeastie Beasties
- Candida albicans most common; dimorphic (yeast, pseudohyphae, true hyphae).
- Forms:
- Superficial: Oral thrush (scrapeable white plaques), vulvovaginitis (cottage cheese discharge), intertrigo.
- Invasive: Candidemia (esp. ICU, central lines), endocarditis, disseminated (liver, spleen).
- Dx: KOH (yeast, pseudohyphae), culture (SDA), Germ tube test (C. albicans). β-D-glucan.
- Rx: Topical (nystatin, azoles); Systemic (fluconazole, echinocandins, Ampho B).
- Risk: Immunosuppression, DM, antibiotics, catheters.

⭐ Candida albicans is germ tube positive at 37°C in serum within 2-4 hours, differentiating it from most other Candida species.
Aspergillus Infections - Moldy Menace
- Ubiquitous mold; spore inhalation. Common species: A. fumigatus, A. flavus (aflatoxin).
- Clinical Forms:
- Allergic Bronchopulmonary Aspergillosis (ABPA): Asthma, eosinophilia, IgE ↑.
- Aspergilloma: Fungus ball in pre-existing lung cavities (e.g., TB).
- Invasive Aspergillosis: Immunocompromised (neutropenia); angioinvasion, fever, cough.
- Diagnosis: Septate hyphae with 45° (acute) angle branching on microscopy. Galactomannan antigen test.
- Treatment: Voriconazole (drug of choice). 📌 Aspergillus = Acute Angle branching.
⭐ Aspergillus flavus produces aflatoxin, a potent hepatocarcinogen strongly linked to hepatocellular carcinoma (HCC).
Cryptococcus Infections - Capsulated Crypt-keeper
- Encapsulated yeast; C. neoformans (immunocompromised, AIDS CD4 <100/µL), C. gattii (immunocompetent).
- Source: Pigeon droppings. Pathogenesis: Inhalation → lungs → hematogenous dissemination, predilection for CNS (meningoencephalitis).
- Virulence: Polysaccharide capsule (antiphagocytic).
- Diagnosis:
- India ink stain (CSF): Visualizes capsule (halos).
- Cryptococcal antigen (CrAg) test (serum/CSF): Rapid, highly sensitive & specific.
- Culture on Sabouraud Dextrose Agar (SDA).
- Treatment: Amphotericin B + Flucytosine (induction); Fluconazole (consolidation/maintenance).

⭐ India ink stain of CSF is a classic rapid diagnostic test revealing the characteristic polysaccharide capsule of Cryptococcus as a clear halo around the yeast cells against a dark background.
Pneumocystis Pneumonia - Lung Parasite Peril
- Agent: Pneumocystis jirovecii (fungus). Airborne transmission.
- Risk: Immunocompromised, esp. HIV (CD4 < 200/µL).
- Sx: Progressive dyspnea, non-productive cough, fever, hypoxemia.
- Dx:
- BAL/sputum: Cysts/trophozoites (GMS, Giemsa stains).
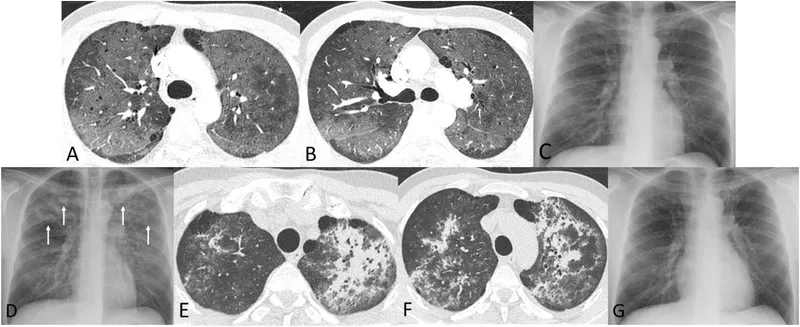
- CXR: Diffuse bilateral interstitial infiltrates (ground-glass).
- ↑ Serum LDH.
- Rx: TMP-SMX. Steroids if severe (PaO2 < 70 mmHg, A-a gradient > 35 mmHg).
- Prophylaxis: TMP-SMX if CD4 < 200/µL or other risks.
⭐ Cell membrane: cholesterol, not ergosterol → most antifungals ineffective.
Mucormycosis - Rhino's Ruin
- Agents: Mucor, Rhizopus, Absidia, Lichtheimia.
- Pathogenesis: Angioinvasion → tissue necrosis (black eschar).
- Risk Factors: Diabetes (DKA), neutropenia, steroids, iron overload (deferoxamine use).
- Clinical: Rhinocerebral (most common; black eschar, facial pain, orbital involvement), pulmonary, cutaneous.
- Diagnosis: Biopsy - broad (5-20 µm), non-septate/pauciseptate hyphae, wide-angle (90°) branching.
⭐ Histopathology: Ribbon-like, aseptate hyphae with wide-angle branching is a key finding.
- Treatment: Surgical debridement + Liposomal Amphotericin B; Posaconazole.

High‑Yield Points - ⚡ Biggest Takeaways
- Candida albicans: Most common; germ tube test (+); thrush, vaginitis, systemic in immunocompromised.
- Aspergillus fumigatus: ABPA, aspergilloma, invasive; acute angle (45°) branching septate hyphae.
- Cryptococcus neoformans: Meningitis in AIDS; India ink for capsule; urease (+); pigeon droppings.
- Mucormycosis: Rhino-orbito-cerebral in diabetics (DKA); broad, non-septate hyphae, 90° branching.
- Pneumocystis jirovecii (PCP): Pneumonia in HIV (CD4 < 200); silver stain for cysts.
- Affect severely immunocompromised (HIV, neutropenia, transplants).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

