Specimen Collection & Transport - Fungal Haul & Handle
- Specimens: Skin, nails, hair; sputum, CSF, blood, tissue.
- Collection: Aseptic technique into sterile containers.
- Site Selection: Crucial; e.g., active lesion edge for skin.
- Quantity: Adequate for microscopy, culture, molecular tests.
- Transport: Rapid, at appropriate temperature (often room temp), prevent drying.
⭐ For dermatophytes, scrape the active, erythematous border of skin lesions.
Direct Microscopic Examination - Scope The Spores
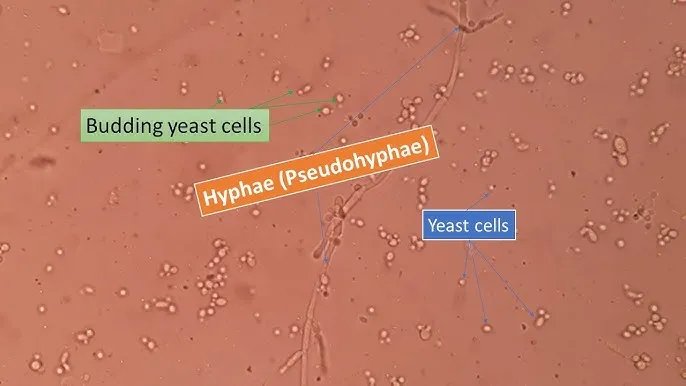
Rapid, cost-effective initial detection. Observe: yeast, pseudohyphae, true hyphae (septate/aseptate), spores, spherules.
| Stain | Use | Fungi (Examples) | Key Finding |
|---|---|---|---|
| $10-20% KOH## Direct Microscopic Examination - Scope The Spores | |||
| Rapid, cost-effective initial detection. Observe: yeast, pseudohyphae, true hyphae (septate/aseptate), spores, spherules. | |||
 |
| Clears tissue; 📌 KOH Kills Our Host cells, Fungi Freely Seen | Most fungi | Fungal elements | | India Ink | Capsule stain | Cryptococcus neoformans | Halo around yeast | | Calcofluor White | Chitin binding, fluorescence | Most fungi | Apple-green fluorescence | | Gram Stain | Yeast stain | Candida spp. | Gram +ve yeasts, pseudohyphae | | Giemsa/Wright | Intracellular fungi | Histoplasma capsulatum | Yeasts in macrophages |> ⭐ Calcofluor white stain requires a fluorescence microscope and binds non-specifically to cellulose and chitin.
Fungal Culture - Grow & Glow Fungi
Definitive ID, speciation & susceptibility.
Culture Media & Incubation:
| Medium | Highlights | Use |
|---|---|---|
| SDA | Dextrose, Peptone | General 📌 Sweet Dreams for Aspergillus |
| Mycosel/Mycobiotic | SDA + Abx + Cycloheximide | Pathogens (inhibits contaminants) |
| BHI Agar | Brain Heart Infusion | Fastidious, dimorphic yeast |
| Caffeic Acid Agar | Phenol oxidase detection | C. neoformans (melanin) |
Identification:
- Macroscopic: Colony (texture, color, pigment).
- Microscopic: LPCB (hyphae, conidia, spores).
- Germ Tube Test: C. albicans (+ve 2-3h, 37°C).

⭐ Dimorphic fungi exhibit thermal dimorphism: mold form at 25-30°C (saprophytic/environmental) and yeast form at 37°C (pathogenic/in vivo).
Serology & Antigen Detection - Immune Clue Hunt
| Test (Antigen/Ab) | Target Fungus/Marker | Sample | Significance/Limitations (Common Methods) |
|---|---|---|---|
| Galactomannan (Ag) | Aspergillus spp. | Serum, BAL | Index >0.5 for IA; false positives. (ELISA) |
| (1→3)-β-D-glucan (BDG) (Ag) | Pan-fungal (not Mucorales, Crypto, Blasto) | Serum | Invasive fungal infection marker; non-specific. (ELISA) |
| Cryptococcal Ag (CrAg) | C. neoformans/gattii (capsular Ag) | CSF, Serum | Diagnosis/prognosis of cryptococcosis. (Latex Agglutination, LFA, EIA) |
| Antibody (Ab) Detection | Histoplasma, Coccidioides, Blastomyces | Serum | Endemic mycoses; less useful in immunocompromised. (ID, CF) |
Molecular Methods - DNA Fungal Fingerprints
- PCR: Conventional, Real-time (qPCR), Multiplex.
- Targets: Internal Transcribed Spacer (ITS) regions, 18S/28S rRNA genes.
- Advantages: ↑Sensitivity, ↑Specificity, rapid Turn-Around Time (TAT); detects non-viable/fastidious fungi.
- Other Techniques:
- Probes & Sequencing: For speciation, phylogeny.
- MALDI-TOF MS: Rapid identification of yeast/mold from culture.
- PNA-FISH (Peptide Nucleic Acid Fluorescence In Situ Hybridization).
⭐ Internal Transcribed Spacer (ITS) regions of ribosomal DNA are common targets for fungal PCR due to interspecies variability and conserved flanking regions for primer binding an ITS region is a piece of non-functional RNA situated between structural ribosomal RNAs on a common precursor transcript
Histopathology - Tissue Tales: Fungi
- Biopsy vital for invasive infections: shows fungi & host response.
- Key Stains: | Stain | Stains | Color | Uses | |---|---|---|---| | H&E | Host, morphology | Variable | Candida | | GMS | Walls | Black | General | | PAS | Glycogen | Magenta | General | | Mucicarmine | Capsule | Pink/Red | Cryptococcus | | Fontana-Masson | Melanin | Brown/Black | Dematiaceous, Crypto |* 📌 GMS: Great Myco Staining; PAS: Pretty Awesome Sugar.
- Morphology: Yeast, hyphae (septation, branching, pigment), spherules.

⭐ Aspergillus: septate hyphae, 45° branching. Mucorales: broad, non-septate/pauciseptate hyphae, wide-angle branching.
High‑Yield Points - ⚡ Biggest Takeaways
- KOH wet mount: For rapid screening and visualization of fungal elements in clinical samples.
- India Ink stain: Specifically demonstrates the polysaccharide capsule of Cryptococcus neoformans, especially in CSF.
- Sabouraud Dextrose Agar (SDA): The most common selective medium for fungal culture, often with antibiotics.
- Calcofluor White stain: A fluorescent stain binding to chitin and cellulose in fungal cell walls, enhancing detection.
- Serological tests (e.g., Galactomannan, Beta-D-Glucan) and PCR: Crucial for early diagnosis of invasive fungal infections.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

