Endemic Mycoses - Dimorphic Invaders
- Fungi geographically restricted to specific regions; cause infection in healthy individuals.
- Exhibit thermal dimorphism.
- 📌 Mnemonic: Mold in Cold, Yeast in Heat/Beast.
- Transmission: Inhalation of spores.
- Primary site: Lungs.
- Increased risk of dissemination in immunocompromised individuals.
⭐ All major endemic mycoses are caused by thermally dimorphic fungi, existing as molds in the environment and yeasts (or spherules for Coccidioides) in host tissues at 37°C (body temperature).
Histoplasmosis - Cave Dweller's Darling
- Organism: Histoplasma capsulatum, dimorphic (mold in soil, yeast at 37°C in tissue).
- Transmission: Inhalation of microconidia from soil with bird/bat guano.
⭐ Associated with bird/bat guano (spelunking, cleaning chicken coops); yeast forms are characteristically found intracellularly within macrophages.
- Clinical:
- Asymptomatic (>90%).
- Acute pulmonary: Flu-like.
- Chronic cavitary: Mimics TB (COPD).
- Progressive Disseminated (PDH): Immunocompromised (AIDS, CD4 < 150); HSM, pancytopenia, ulcers.
- Diagnosis:
- Microscopy: Oval yeasts in macrophages (Giemsa/Wright).
- Antigen detection (urine/serum) for PDH.
- Culture (gold std, slow).
- Treatment:
- Mild/Mod: Itraconazole.
- Severe/PDH: Ampho B (lipid) → Itraconazole.

Blastomycosis - Broad-Based Bad Boy
- Etiology: Blastomyces dermatitidis (dimorphic fungus: mold in soil, yeast at 37°C).
- Morphology: Yeast: Large, thick-walled, single broad-based bud. 📌 "B" for Blastomycosis, Broad-Based Bud.
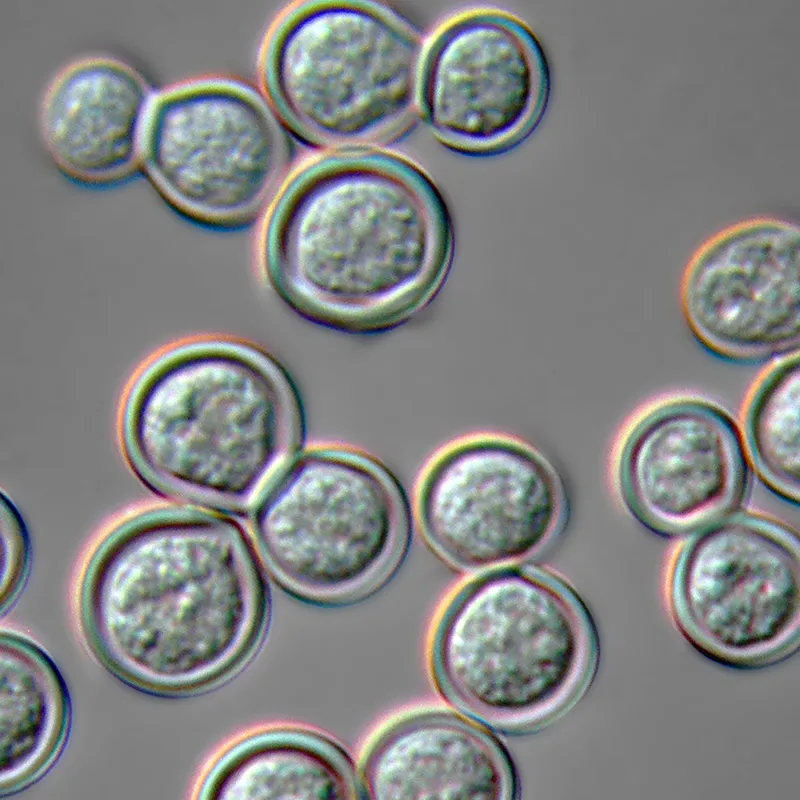
- Transmission: Inhalation of spores from moist soil/decaying wood.
- Endemic: North America (Ohio-Mississippi River valleys, Great Lakes).
- Clinical Features:
- Pulmonary: Asymptomatic, acute/chronic pneumonia (mimics TB/cancer).
- Extrapulmonary (disseminated):
- Skin (most common): Verrucous, crusted, or ulcerative lesions.
- Bone: Osteolytic lesions, arthritis.
- Genitourinary: Prostatitis, epididymitis.
⭐ Characterized by large yeast cells with a single broad-based bud; frequently causes skin (verrucous/ulcerative) and bone (lytic) lesions.
- Diagnosis: Microscopy (KOH/histology showing broad-based budding yeast), culture (gold standard).
- Treatment: Itraconazole (mild-moderate); Amphotericin B (severe/CNS).
Coccidioidomycosis - Desert Spherule Spectre
- Organism: Coccidioides immitis/posadasii (dimorphic).
- AKA: Valley Fever. Endemic: Arid SW USA, Mexico.
- Transmission: Inhalation of arthroconidia.
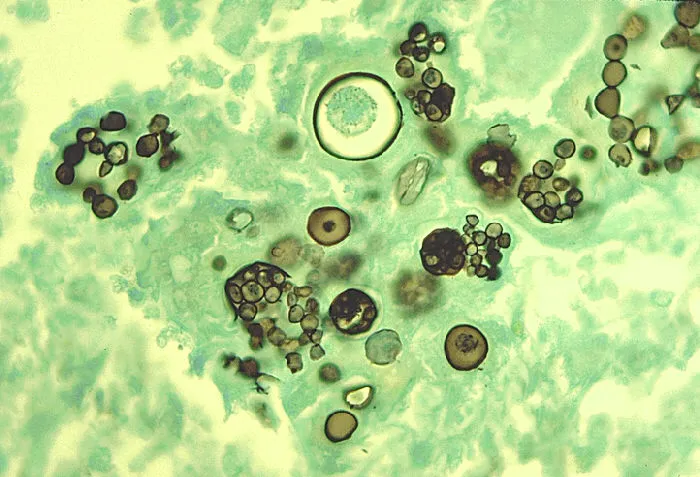
- Pathology: Arthroconidia → spherules (20-60 µm) in tissue, release endospores. Mold (arthroconidia) at 25°C.
⭐ Unique among these fungi for forming spherules containing endospores in tissue (not yeast); endemic to arid/semi-arid regions (e.g., Southwestern US, leading to 'Valley Fever').
- Clinical: Often asymptomatic. Flu-like illness, erythema nodosum. Severe: pulmonary disease, dissemination (skin, bone, CNS) in immunocompromised.
- Diagnosis: Microscopy (spherules), culture (⚠️ biohazard!), serology.
- Treatment: Amphotericin B (severe), azoles.
Paracoccidioidomycosis - Pilot's Wheel Peril
- Agent: Paracoccidioides brasiliensis (dimorphic fungus).
- Epidemiology: Endemic in Latin America. Affects adult male agricultural workers. Route: Inhalation of soil conidia.
- Clinical Forms:
- Acute/Subacute (Juvenile): Disseminated; reticuloendothelial system involvement.
- Chronic (Adult): Reactivation; pulmonary lesions (fibrosis), mucocutaneous ulcers (e.g., oral "mulberry-like").
- Diagnosis: Microscopy (characteristic yeast), culture, serology.
- Treatment: Itraconazole (mild/moderate); Amphotericin B (severe).
⭐ Yeast form shows multiple peripheral budding from a large central cell, resembling a 'mariner's wheel' or 'pilot's wheel'; predominantly affects adult male agricultural workers in Latin America.
oka
High‑Yield Points - ⚡ Biggest Takeaways
- Endemic mycoses: Caused by dimorphic fungi (mold in cold, yeast in tissue at 37°C).
- Histoplasmosis: Bat/bird droppings; mimics TB; intracellular yeasts in macrophages.
- Blastomycosis: Broad-based budding yeast; affects lungs, skin, bone; North America.
- Coccidioidomycosis: Spherules with endospores; "Valley Fever"; Southwestern US/deserts.
- Paracoccidioidomycosis: "Mariner's wheel" yeast; prevalent in Latin America.
- Sporotrichosis: "Rose gardener's disease"; lymphocutaneous spread; cigar-shaped yeasts.
- Talaromycosis (Penicilliosis): AIDS in SE Asia; red diffusible pigment; yeast-like cells dividing by fission.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

