Dermatophyte Basics - Skin Invaders
- Keratinophilic fungi causing superficial mycoses (tinea/ringworm).
- Invade dead, keratinized tissues: stratum corneum (skin), hair, nails.
- Do not typically invade living tissue.
- Three Anamorph Genera:
- Trichophyton (T): Infects skin, hair, nails.
- Microsporum (M): Infects skin, hair.
- Epidermophyton (E): Infects skin, nails. (📌 Mnemonic: E for Epidermophyton, Excludes hair)
- Ecological Classification (Sources):
- Anthropophilic: Humans; chronic, mild inflammation (e.g., T. rubrum).
- Zoophilic: Animals; acute, intense inflammation (e.g., M. canis).
- Geophilic: Soil; moderate inflammation (e.g., M. gypseum).

⭐ Dermatophytes possess keratinases, enzymes that digest keratin, allowing them to colonize and derive nutrients from skin, hair, and nails.
Clinical Tineas - Ringworm Ruckus

| Tinea Site | Common Name | Key Features & Organisms |
|---|---|---|
| Corporis | Body Ringworm | Annular, erythematous, scaly lesions; central clearing, active raised border. T. rubrum, M. canis. |
| Pedis | Athlete's Foot | Interdigital (maceration, fissures), moccasin (dry, diffuse scaling), vesiculobullous. T. rubrum, T. interdigitale. |
| Cruris | Jock Itch | Groin; erythematous, scaly, well-demarcated active border; typically spares scrotum. T. rubrum, E. floccosum. |
| Capitis | Scalp Ringworm | Scaling, alopecia. Ectothrix (Microsporum spp.; Wood's lamp +ve), Endothrix (T. tonsurans; Wood's lamp -ve), Favus (scutula), Kerion (boggy lesion). |
| Unguium | Onychomycosis | Nail discoloration (yellow/white), thickening, subungual hyperkeratosis/debris. T. rubrum. |
| Barbae | Beard Ringworm | Folliculitis, kerion-like lesions in beard. T. verrucosum, T. mentagrophytes. |
| Manuum | Hand Ringworm | Unilateral palm scaling/hyperkeratosis; "one hand, two feet" syndrome. T. rubrum. |
| Faciei | Face Ringworm | Annular lesions on face (non-bearded). Tinea incognito (steroid-modified, atypical). M. canis, T. rubrum. |
Lab Diagnosis - Scope & Spores
- Specimen Collection: Skin scrapings, nail clippings, plucked hairs (infected part).
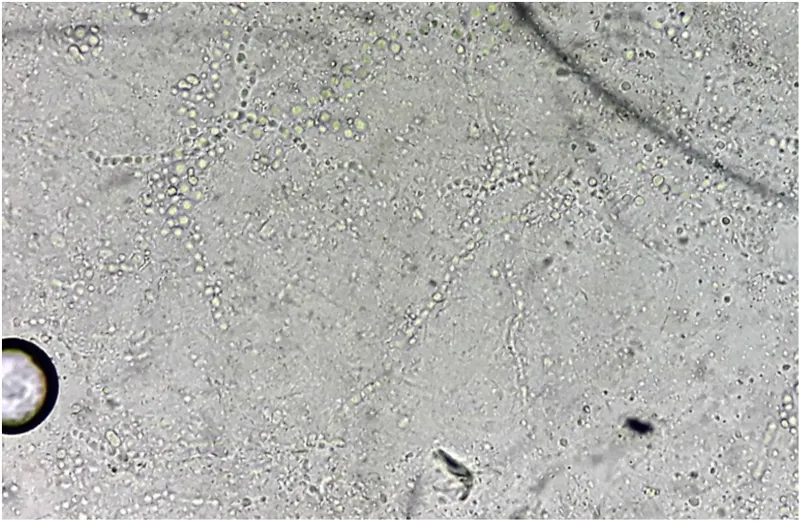
- Microscopy (KOH Mount):
- Reagent: 10-20% KOH (dissolves keratin).
- Visualizes: Septate hyaline hyphae, arthroconidia.
- Parker ink / Calcofluor white stain enhances visibility.
- Culture:
- Medium: Sabouraud Dextrose Agar (SDA) with cycloheximide & chloramphenicol.
- Incubation: 25-30°C for 1-4 weeks.
- Identification: Colony morphology (obverse/reverse pigment), microscopic features (macroconidia, microconidia).
- Wood's Lamp (UV light ~365nm):
- Microsporum audouinii, M. canis: Bright green fluorescence (pteridine).
- Trichophyton schoenleinii: Pale green fluorescence.
- Not all dermatophytes fluoresce.
⭐ Arthroconidia are the infectious propagules formed by fragmentation of hyphae, characteristic of dermatophytes in tissue.
Dermatophyte Treatment - Fungal Fighters
- Topical Antifungals (Localized/Mild Infections):
- Azoles: Clotrimazole, Miconazole, Ketoconazole, Luliconazole, Sertaconazole.
- Allylamines: Terbinafine cream (highly effective).
- Ciclopirox olamine.
- Duration: 2-4 weeks, continue for 1-2 weeks after clinical resolution.
- Systemic Antifungals (Extensive/Nail/Hair/Resistant Infections):
- Terbinafine: 250 mg OD. Tinea capitis (4-8 weeks), onychomycosis (6-12 weeks for fingernails, 12-24 weeks for toenails).
- Itraconazole: 100-200 mg OD/BD. Pulse therapy for onychomycosis (200 mg BD for 1 week/month).
- Fluconazole: 150 mg once weekly for 4-6 weeks (tinea corporis/cruris); 50 mg OD for tinea pedis.
- Griseofulvin: (Mainly for tinea capitis in children) 10-20 mg/kg/day.
- 📌 Mnemonic: "Greasy Griseofulvin" - take with fatty meal for ↑ absorption.
⭐ Terbinafine is generally considered fungicidal against dermatophytes, while azoles are primarily fungistatic.
- Adjunctive Therapy:
- Keratolytics (Salicylic acid) for hyperkeratotic lesions.
- Keep area dry; loose cotton clothing.
- ⚠️ Avoid topical steroid monotherapy (can worsen infection - tinea incognito).
High‑Yield Points - ⚡ Biggest Takeaways
- Dermatophytes (Trichophyton, Epidermophyton, Microsporum) are keratinophilic fungi infecting skin, hair, and nails.
- Cause various Tinea infections (ringworm), classified by anatomical location (e.g., Tinea pedis, Tinea cruris).
- Trichophyton rubrum is the most common etiological agent worldwide.
- Diagnosis relies on KOH microscopy (revealing septate hyphae) and Wood's lamp (fluorescence for some Microsporum species, e.g., M. canis).
- Arthroconidia are the infective elements responsible for transmission.
- Treatment includes topical antifungals; oral agents like terbinafine, itraconazole, or griseofulvin are used for extensive or nail/hair infections.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

