Organism & Virulence - Crypto's ID & Arsenal
- Organism: Cryptococcus neoformans (common, esp. AIDS) & C. gattii (tropics, immunocompetent/compromised).
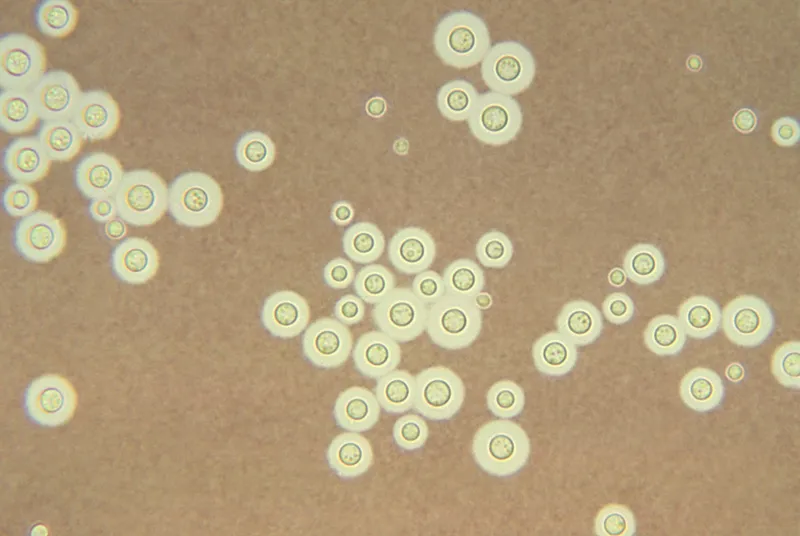
- Encapsulated yeast, 5-10 µm diameter.
- Round to oval, reproduces by narrow-based budding.
- Not dimorphic (yeast form only).
- Virulence Factors (Crypto's Arsenal):
- Polysaccharide Capsule: Major! Mainly GXM (glucuronoxylomannan).
- Antiphagocytic, inhibits leukocyte migration, immunosuppressive.
⭐ The capsule is its primary virulence factor; visualized by India Ink (negative stain) as a clear halo.
- Melanin Production: Via laccase.
- Protects from oxidative stress & host enzymes; neurotropic. (📌 "MELANIN: Mighty & Mind-loving")
- Phospholipase B: Host membrane damage, tissue invasion.
- Urease: Produces $NH_3$, ↑pH, aids CNS invasion (BBB).
- Thermotolerance: Grows at 37°C.
- Polysaccharide Capsule: Major! Mainly GXM (glucuronoxylomannan).
Epidemiology & Risk Factors - Who Gets Hit & How
- Distribution & Species:
- C. neoformans: Ubiquitous worldwide.
- C. gattii: Predominantly tropical/subtropical; emerging temperate (Pacific NW).
- Reservoirs:
- C. neoformans: Soil enriched with pigeon guano.
- C. gattii: Eucalyptus trees, decaying wood.
- Transmission: Inhalation of airborne yeast/basidiospores. No human-to-human spread.
- Risk Factors (C. neoformans):
- Cellular Immunodeficiency (Major):
- HIV/AIDS: CD4+ T-cell count < 100 cells/µL (most critical). 📌 AIDS-defining illness.
- Solid organ transplant recipients (on immunosuppressive therapy).
- Prolonged high-dose corticosteroid therapy.
- Hematologic malignancies (e.g., lymphoma, CLL).
- Sarcoidosis.
- Biologic agents (e.g., TNF-α inhibitors).
- C. gattii: Notably can infect immunocompetent individuals, unlike typical C. neoformans.
- Cellular Immunodeficiency (Major):
⭐ Globally, cryptococcal meningitis is a leading opportunistic infection and a major cause of mortality in patients with advanced HIV/AIDS.
Clinical Manifestations - Brain & Lung Invasion
-
Pulmonary Cryptococcosis:
- Often asymptomatic in immunocompetent individuals.
- Symptoms: Cough (productive or non-productive), low-grade fever, pleuritic chest pain, dyspnea, weight loss.
- Radiology: Nodules (cryptococcomas), infiltrates (diffuse or lobar), pleural effusions, hilar lymphadenopathy.
- Can disseminate, especially in immunocompromised.
-
Cryptococcal Meningoencephalitis (CM): Most common CNS manifestation.
- Predominantly in immunocompromised (HIV/AIDS, CD4 < 100 cells/µL).
- Symptoms: Headache (often severe, persistent), fever, altered mental status, lethargy, nausea, vomiting, neck stiffness, photophobia, seizures.
- Cranial nerve palsies (esp. VI, VII, VIII) common.
- ↑ Intracranial pressure (ICP) is a major cause of morbidity/mortality.
⭐ Raised ICP is a hallmark of cryptococcal meningitis and a poor prognostic indicator. Management often requires therapeutic lumbar punctures or shunting.

- Other sites of dissemination (less common): Skin (papules, pustules, ulcers resembling molluscum contagiosum), bone, prostate, eyes (choroidoretinitis).
Diagnosis & Management - Unmasking & Eradicating
- Diagnosis:
- CSF analysis: ↑Protein, ↓Glucose, Lymphocytic pleocytosis.
- India Ink: Encapsulated budding yeast (halos). Sensitivity ~50-80% in AIDS.
- Cryptococcal Antigen (CrAg): Serum/CSF. Rapid, high Sensitivity & Specificity.
⭐ CrAg titers often correlate with fungal burden and can monitor therapeutic response.
- Culture (SDA): Gold standard.
- Management:
- Manage ↑Intracranial Pressure (ICP): Aggressive! Therapeutic Lumbar Punctures (if Opening Pressure >25 $cm H_2O$); shunts if refractory.
- Antifungal Therapy (Phased for CNS disease):
- Induction (HIV+ or severe CNS): Liposomal Ampho B (LAmB) **3-4** mg/kg/d IV + Flucytosine (5-FC) **100** mg/kg/d PO (div. doses) x ≥**2** wks.
- Consolidation: Fluconazole **400-800** mg/d PO x **8** wks.
- Maintenance: Fluconazole **200** mg/d PO x ≥**1** yr.
- Immune Reconstitution Inflammatory Syndrome (IRIS): Paradoxical worsening on ART; manage with NSAIDs/steroids if severe.
High‑Yield Points - ⚡ Biggest Takeaways
- Cryptococcus neoformans: Encapsulated yeast from pigeon droppings; acquired by inhalation.
- Key virulence: Large polysaccharide capsule (visualized by India Ink, resists phagocytosis).
- High risk: HIV/AIDS patients (CD4 < 100 cells/µL), other immunocompromised states.
- Predominant disease: Meningoencephalitis; also causes pulmonary and cutaneous infections.
- Diagnosis: Cryptococcal antigen (CrAg) test (CSF/serum) is crucial; CSF India Ink for direct visualization.
- Treatment: Amphotericin B + Flucytosine for induction, followed by Fluconazole maintenance.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more


