Intro & Species - Yeastie Beasties 101
- Candida: Opportunistic yeast, part of normal flora (skin, GIT, GU).
- Dimorphic: Exists as budding yeast (commensal) & pseudohyphae/hyphae (invasive).
- C. albicans forms true hyphae (germ tubes).
- Species:
- C. albicans: Most common.
- Non-albicans Candida (NAC): C. tropicalis, C. parapsilosis, C. glabrata (often reduced azole susceptibility), C. krusei (intrinsic fluconazole resistance).
⭐ Candida albicans is the most common species and is germ tube positive.
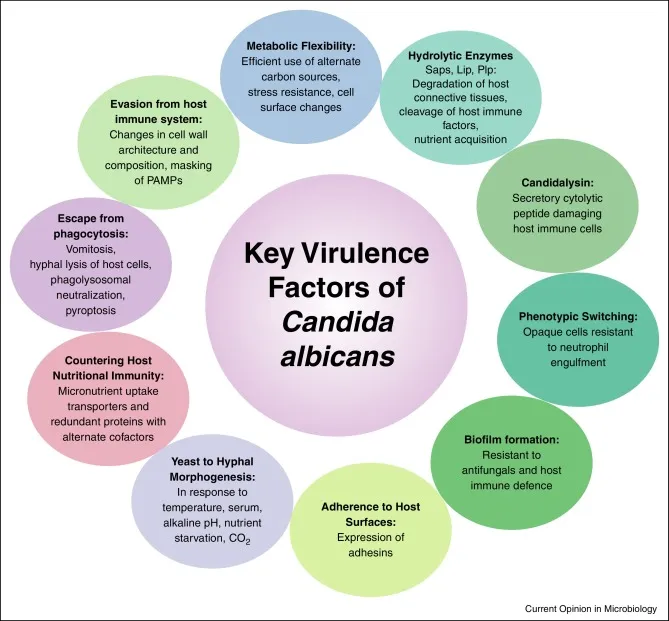
Pathogenesis & Virulence - Candida's Crafty Conquests
- Adherence: Mediated by Als proteins (Agglutinin-like sequence) & Hwp1 (Hyphal wall protein 1); crucial first step.
- Biofilms: Structured communities on surfaces (e.g., catheters, implants); ↑ drug resistance, protects from host defenses.
⭐ Biofilm formation by Candida species, especially on indwelling medical devices, is a major virulence factor contributing to drug resistance.
- Phenotypic Switching: Yeast-to-hyphae transition (dimorphism) is key for invasion. Hyphae penetrate tissues.
- Hydrolytic Enzymes: Secreted aspartyl proteases (SAPs), phospholipases, lipases; damage host tissues, facilitate invasion.
Clinical: Mucocutaneous - Surface Skirmishes
- Oral Thrush: White, removable plaques (pseudomembranes) on oral mucosa. Risk: Infants, immunocompromised, steroid inhalers.
- Esophagitis: Dysphagia, odynophagia, especially in HIV/AIDS.
- Vulvovaginitis (VVC): Intense itching, burning; thick, white "cottage cheese" discharge. Risk: Diabetes, antibiotics, pregnancy.
⭐ Recurrent vulvovaginal candidiasis (RVVC) is defined as ≥4 symptomatic episodes in 12 months.
- Intertrigo: Erythematous rash with satellite lesions in moist skin folds (axillae, groin, inframammary).
- Diaper Rash: Confluent erythematous rash with satellite pustules in diaper area.
- Onychomycosis: Fungal infection of nails; thickened, discolored.
Clinical: Invasive - Deep Dive Dangers
Invasive candidiasis: severe, life-threatening infections, often in immunocompromised.
- Key Risk Factors: Central lines (CVCs), TPN, neutropenia, broad-spectrum antibiotics, major surgery, immunosuppression, prolonged ICU stay.
- Major Syndromes:
- Candidemia: Candida in blood; most common.
- Disseminated: Hematogenous spread.
- Endophthalmitis (eye; risk of blindness).
- Endocarditis (heart valves).
- CNS infection (meningitis, abscesses).
- Hepatosplenic, osteoarticular.
- Candida UTI: Often catheter-related, esp. in high-risk.
⭐ In patients with candidemia, an ophthalmologic exam is mandatory to rule out Candida endophthalmitis, even in asymptomatic patients.
Lab Diagnosis - Unmasking the Yeast

- Microscopy: KOH mount (budding yeasts, pseudohyphae; true hyphae - C. albicans). Gram stain (Gram-positive).
- Culture: Sabouraud Dextrose Agar (SDA).
- Identification: Germ Tube Test (C. albicans/dubliniensis). Chromogenic agar (species differentiation).
- Advanced: (1,3)-β-D-glucan assay, PNA-FISH, MALDI-TOF MS.
⭐ The germ tube test is a rapid, simple, and inexpensive test for the presumptive identification of Candida albicans and Candida dubliniensis.
Treatment - Candida Combat Plan
| Class | Drugs | Notes |
|---|---|---|
| Azoles | Fluconazole, Voriconazole | Common; C. krusei resistant. Fluconazole 200-400mg. |
| Polyenes | Amphotericin B | Severe/invasive. |
| Echinocandins | Caspofungin | Invasive, azole-resistant (C. glabrata, C. krusei). |
High‑Yield Points - ⚡ Biggest Takeaways
- Candida albicans: Most common, dimorphic (yeast & pseudohyphae). Germ tube test positive.
- Clinical forms: Oral thrush, vulvovaginitis (cottage cheese), esophagitis, cutaneous, systemic (immunocompromised).
- Risk factors: Immunosuppression, diabetes, antibiotics, corticosteroids, catheters.
- Diagnosis: KOH mount (yeast, pseudohyphae), culture on SDA; Chromogenic agar for speciation.
- Treatment: Topical azoles; oral fluconazole; echinocandins or Amphotericin B for severe/invasive disease.
- Chronic Mucocutaneous Candidiasis (CMC) linked to T-cell defects (e.g., AIRE).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

