Host Defenses Down - Immune Gaps Intro
-
Immunocompromised Host: State of ↑ susceptibility to infections due to deficient host defenses.
-
Major Immune Defects & Common Causes:
Defect Type Key Causes Associated Risk Neutropenia Chemotherapy, malignancy; ANC < 500/µL severe Bacterial, fungal T-cell Dysfunction HIV, transplant drugs, corticosteroids, PID Intracellular pathogens B-cell Dysfunction PID (XLA, CVID), some cancers Encapsulated bacteria Complement Defect PID (e.g., C5-C9 deficiency) Neisseria spp. Asplenia Splenectomy, sickle cell Encapsulated bacteria -
General causes include: Primary Immunodeficiencies (PID), HIV infection, organ/stem cell transplantation, chemotherapy, and chronic corticosteroid use.
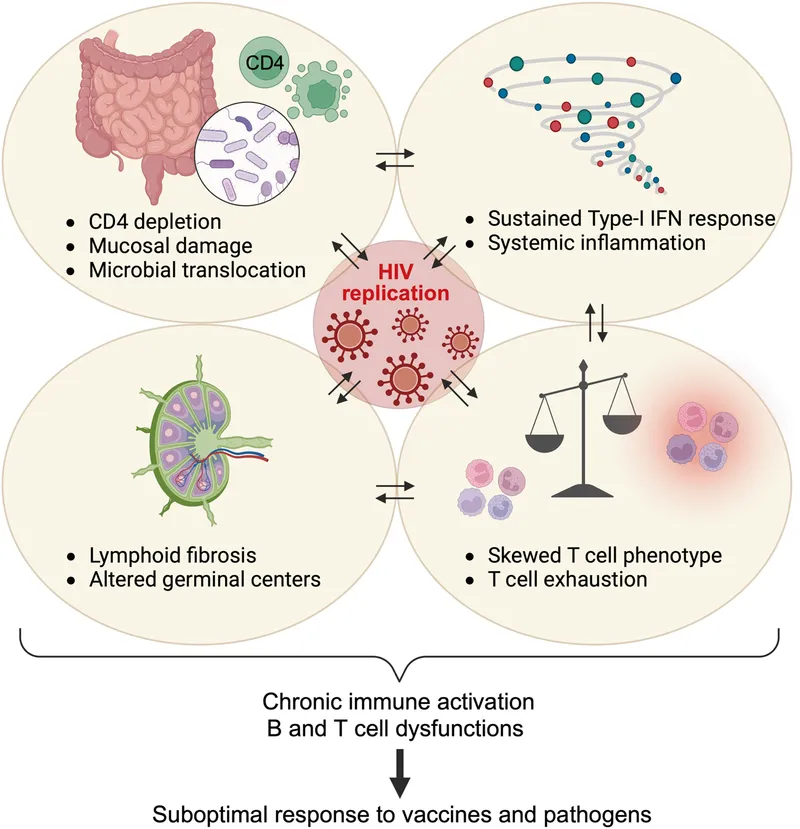
⭐ Severe neutropenia (Absolute Neutrophil Count < 500/µL) dramatically increases the risk of invasive bacterial and fungal infections.
Pathogen Parade - Bugs & Syndromes
| Immune Defect | Common Pathogens | Key Syndromes |
|---|---|---|
| Neutropenia | Pseudomonas aeruginosa, Aspergillus spp. | Sepsis, pneumonia, invasive fungal disease |
| T-cell Defects | Pneumocystis jirovecii (PJP), CMV, Cryptococcus, Listeria, Nocardia, Toxoplasma | Pneumonia, retinitis, meningitis, CNS/systemic infections |
| B-cell Defects | Encapsulated: S. pneumoniae, H. influenzae | Sinopulmonary infections, bacteremia |
| Asplenia | Encapsulated bacteria (as above), Capnocytophaga canimorsus | Overwhelming sepsis (OPSI), dog bite infections |
| Complement Defects | Neisseria spp. (esp. N. meningitidis) | Recurrent meningococcal/gonococcal disease |
⭐ Pneumocystis jirovecii pneumonia (PJP) is a classic opportunistic infection in patients with T-cell immunodeficiency, particularly when CD4 count drops below 200 cells/µL.
Sleuthing & Defense - Unmasking & Managing
- Challenges: Atypical presentations, rapid progression. Early diagnosis is key.
- Key Tests:
- Cultures (blood, site-specific).
- PCR (CMV, EBV, BK virus).
- Antigen tests: Galactomannan, β-D-glucan, Cryptococcal Ag.
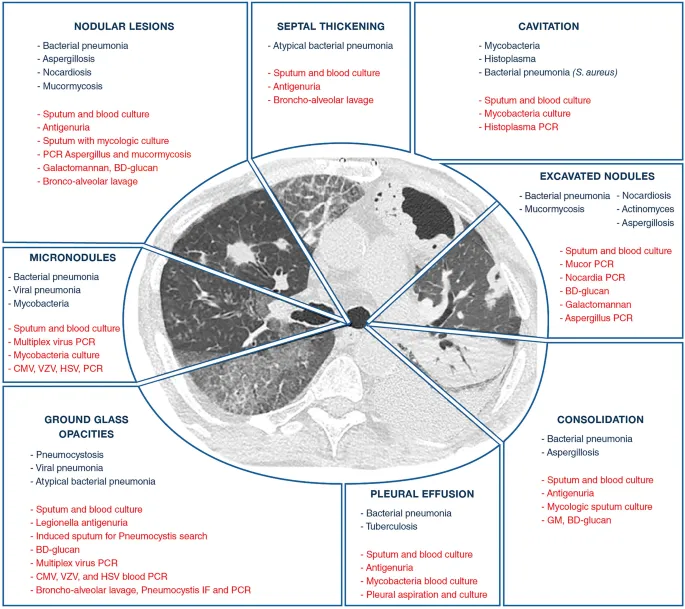
- Imaging (CT/MRI) for occult sites.
- Management:
- Prophylaxis: PJP (TMP-SMX), MAC, fungal, viral (e.g., valganciclovir for CMV).
- Therapy: Empiric (febrile neutropenia: Temp >38.3°C or >38°C for 1hr + ANC <500/µL), pre-emptive, targeted.
- G-CSF use considered.
⭐ In high-risk febrile neutropenic patients, empiric broad-spectrum antibacterial therapy (e.g., anti-pseudomonal beta-lactam) should be initiated within 1 hour of presentation.
Vulnerable VIPs - Transplant & HIV Tales
- HSCT Timeline:
- Pre-engraftment (<30d): Bacterial, HSV, Candida.
- Early post (30-100d): CMV, PJP, Aspergillus.
- Late post (>100d): VZV, Encapsulated bacteria.
- SOT Risks:
- Early (1st month): Nosocomial.
- Mid (1-6 months): Opportunistic (CMV, PJP).
- Late (>6 months): Community-acquired.
- HIV OIs by CD4 Count: (TB risk ↑ with ↓CD4)
CD4 Count (cells/µL) Key Opportunistic Infections <200 PJP <100 Toxoplasmosis <50 CMV, MAC - 📌 Mnemonic: "Below 200 PJP, 100 Toxo, 50 CMV/MAC."
- IRIS: Immune Reconstitution Inflammatory Syndrome with ART.
⭐ CMV retinitis is a common AIDS-defining illness when CD4 count falls below 50 cells/µL.

High‑Yield Points - ⚡ Biggest Takeaways
- CMV (retinitis, colitis) common in HIV (CD4 < 50) & transplants.
- PJP (CD4 < 200 in HIV); TMP-SMX for prophylaxis & treatment.
- Cryptococcal meningitis (CD4 < 100 in HIV); India ink; Amphotericin B.
- Invasive Aspergillosis in neutropenia; halo sign on CT; Voriconazole.
- Disseminated TB & MAC common in advanced HIV.
- Nocardia mimics TB; treat with TMP-SMX.
- Febrile neutropenia: prompt empiric piperacillin-tazobactam.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

