Infective Endocarditis - Valve Vandals
- Etiology: S. aureus (acute, IVDU), Viridans streptococci (subacute, dental), Enterococci, HACEK, Fungi.
- Risk Factors: Prosthetic valves, IVDU, RHD, indwelling lines.
- Pathogenesis: Endothelial injury → Non-Bacterial Thrombotic Endocarditis (NBTE) → Bacteremia → Vegetation.
- Clinical: 📌 FROM JANE: Fever, Roth spots, Osler nodes, Murmur (new), Janeway lesions, Anemia, Nail-bed hemorrhages, Emboli.
- Diagnosis: Duke Criteria
- Major: +ve Blood Culture (typical organism); Echo (vegetation, abscess, new regurgitation).
- Minor: Predisposition; Fever ≥38°C; Vascular (emboli, Janeway); Immunologic (Osler, Roth, Glomerulonephritis); +ve microbiology not meeting major criteria.
- Definite IE: 2 Major OR 1 Major + 3 Minor OR 5 Minor.
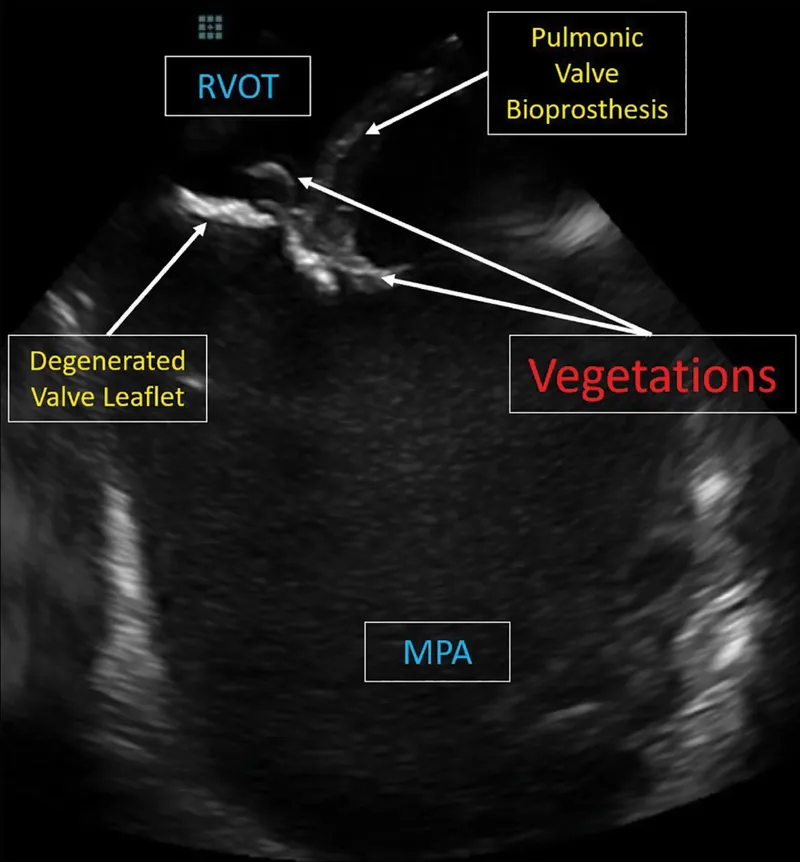
⭐ Culture-negative endocarditis: often due to prior antibiotics; also consider Coxiella burnetii, Bartonella spp.
- Management:
- Empiric antibiotics (e.g., Vancomycin + Gentamicin).
- Specific therapy (culture-guided) for 4-6 weeks.
- Surgery: valve dysfunction, persistent sepsis, large vegetations (>10mm) + emboli risk.
Rheumatic Fever/RHD - Strep's Sad Encore
- Immune-mediated sequel (2-4 weeks) to untreated Group A Strep (GAS) pharyngitis.
- Pathogenesis: Molecular mimicry (Strep M protein vs. host tissues like heart, joints, CNS, skin).
- 📌 JONES Criteria (Evidence of prior GAS infection + 2 Major OR 1 Major & 2 Minor):
- Major: Carditis (pancarditis), Polyarthritis (migratory, large joints), Chorea (Sydenham's), Erythema Marginatum, Subcutaneous Nodules.
- Minor: Fever (≥38.5°C), Arthralgia, ↑ESR (≥60) / CRP (≥3), Prolonged PR.
- Carditis: Most severe. Aschoff bodies (pathognomonic myocardial granulomas); MacCallum patch (LA endocardium).
- RHD: Chronic valvular disease from ARF. Mitral valve most affected (stenosis > regurg.), then aortic. "Fish-mouth"/"button-hole" deformity.
- Prevention: Primary (treat GAS pharyngitis), Secondary (long-term Penicillin prophylaxis post-ARF).
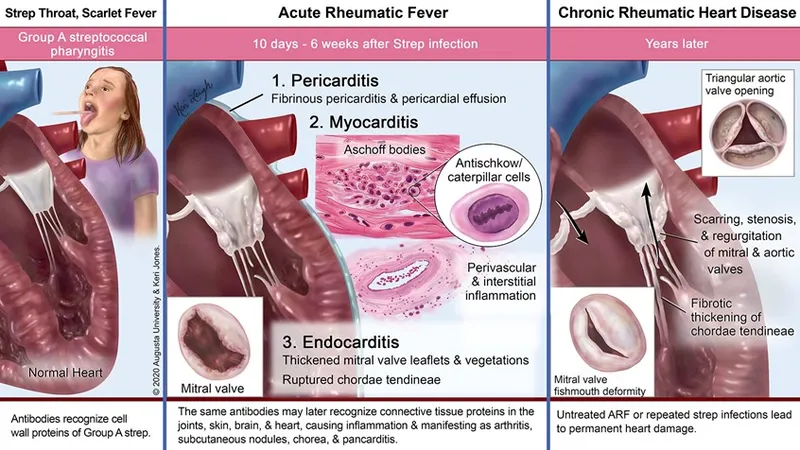
⭐ Mitral valve: most frequently and severely affected in chronic RHD, classically causing stenosis.
Myo/Pericarditis - Heart's Inflamed Hug
- Etiology:
- Viral (Coxsackie B, Adenovirus, Parvovirus B19) common for both.
- Myocarditis: Also autoimmune (SLE, sarcoidosis), drugs (clozapine), toxins, Chagas disease, giant cell myocarditis.
- Pericarditis: Also bacterial (TB), fungal, uremia, post-MI (Dressler's syndrome), autoimmune, malignancy, trauma, radiation.
- Clinical Features:
- Myocarditis: Chest pain (often vague), dyspnea, fatigue, palpitations, arrhythmias, signs of heart failure (HF). Can be fulminant.
- Pericarditis: Sharp, pleuritic chest pain (relieved by sitting up/leaning forward, worsened by lying supine/inspiration), pericardial friction rub (triphasic, often transient). Fever common.
- Investigations:
- ECG:
- Myo: Sinus tachycardia, ST-T changes (non-specific), AV block, ventricular arrhythmias.
- Peri: Diffuse concave ST elevation & PR depression (Stage 1); T-wave inversions (Stage 3).
- Biomarkers: ↑ Troponin (more significant in Myo), ↑ CK-MB, ↑ ESR/CRP.
- ECHO: Myo (LV systolic dysfunction, regional wall motion abnormalities), Peri (pericardial effusion, signs of tamponade e.g., diastolic RV collapse).
- CXR: Myo (cardiomegaly, pulmonary edema), Peri (normal or "water-bottle" heart with large effusion).
- ECG:
- Management:
- Supportive: Rest, O2. Treat HF (ACEi, ARBs, beta-blockers, diuretics), arrhythmias.
- Myocarditis: Specific Rx if cause identified (e.g., immunosuppression for giant cell/sarcoidosis).
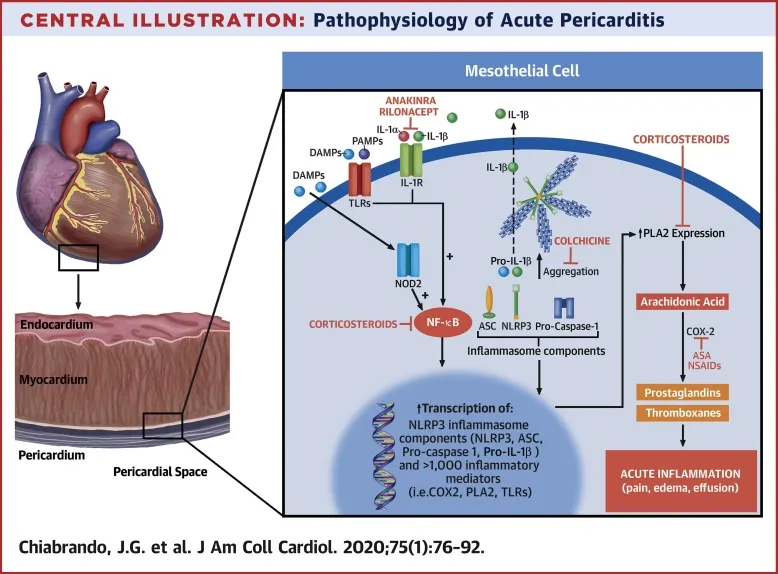
- Pericarditis: NSAIDs (e.g., Ibuprofen 600-800 mg TID) + Colchicine (0.5-0.6 mg OD or BID for 3 months to prevent recurrence). Steroids for refractory cases or if NSAIDs contraindicated.
- Pericardiocentesis for tamponade or large symptomatic effusion.
- Complications:
- Myo: Dilated cardiomyopathy (DCM), arrhythmias, sudden cardiac death (SCD).
- Peri: Cardiac tamponade, constrictive pericarditis, recurrent pericarditis.
⭐ In acute pericarditis, PR segment depression is highly specific, especially when present with diffuse ST elevation.
High‑Yield Points - ⚡ Biggest Takeaways
- Infective Endocarditis (IE): Diagnosis via Duke Criteria. Staph. aureus (IVDU, tricuspid), Viridans streptococci (post-dental).
- Culture-negative IE: Consider Coxiella, Bartonella, HACEK. Stigmata: Janeway lesions, Osler's nodes.
- Acute Rheumatic Fever: Post-Group A Strep; Jones Criteria. Mitral valve most affected.
- Myocarditis & Pericarditis: Often viral (Coxsackie B). Pericarditis pain improves leaning forward.
- TB pericarditis prevalent in India. Early Prosthetic Valve Endocarditis: Staph. epidermidis.
- IE Prophylaxis: For high-risk patients during specific dental/respiratory procedures.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

