Innate Immunity: Overview & Barriers - First Line Fortifications
-
Core Features: Rapid (minutes-hours), non-specific, no prior exposure, no memory. Germline encoded PRRs.
-
First Line Defenses: Prevent pathogen entry & colonization. Barriers are sequential.
- Physical/Mechanical:
- Intact Skin (keratin, desquamation).
- Mucous Membranes (mucus, cilia, peristalsis).
- Flushing actions (tears, saliva, urine).
- Chemical:
- pH: Gastric acid (pH 1-3), skin (pH ~5.5), vaginal lactic acid.
- Antimicrobial peptides (AMPs): Defensins, Cathelicidins.
- Enzymes: Lysozyme (tears, saliva) - targets peptidoglycan by hydrolyzing $\beta-(1,4)$ NAM-NAG bonds.
- Microbiological:
- Normal Flora: Competitive exclusion, bacteriocins.
- Physical/Mechanical:
⭐ Defensins and Cathelicidins are key antimicrobial peptides (AMPs) that disrupt microbial membranes.
Innate Immunity: Cellular Sentinels - The Immune Foot Soldiers
Key cells for immediate defense:
- Phagocytes: Engulf and destroy pathogens.
- Neutrophils (PMNs): Abundant first responders. Multi-lobed nucleus. Phagocytosis, NETosis. 📌 Neutrophils: Numerous, Nimble.
- Macrophages: From monocytes. Phagocytosis, Ag presentation, cytokines. Tissue-specific (Kupffer cells - liver).
- Dendritic Cells (DCs): Potent APCs; bridge innate to adaptive immunity.
- Natural Killer (NK) Cells: Lymphoid origin, innate function. Target virus-infected & tumor cells with ↓MHC-I.
⭐ NK cells employ "missing-self recognition," targeting cells with reduced or absent MHC class I molecules.
- Mast Cells & Basophils: Release histamine, mediators in allergy/inflammation.
- Eosinophils: Combat parasites; modulate allergic inflammation.
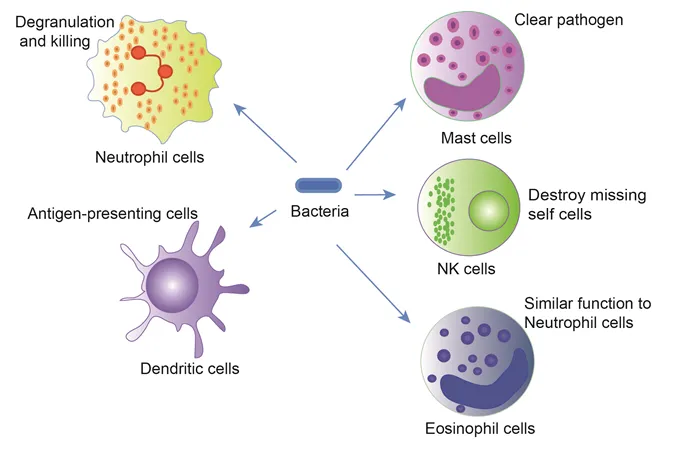
Phagocytosis Overview:
Innate Immunity: Molecular Mediators - Chemical Warfare Crew
Key soluble factors orchestrating innate defense:
- Cytokines:
- Pro-inflammatory: TNF-α, IL-1, IL-6 (fever, inflammation). 📌 "Hot T-Bone stEAk": IL-1 (fever), TNF-α, IL-6 (APPs).
- Type I IFNs (IFN-α, IFN-β): Induce antiviral state in cells.
- IFN-γ (Type II IFN): Activates macrophages; from NK cells/T-cells.
- Chemokines:
- IL-8 (CXCL8): Neutrophil chemoattractant.
- Complement System:
- Key roles: Opsonization ($C_3b$), Inflammation ($C_3a, C_5a$), Lysis (MAC $C_5b-C_9$).
- Acute Phase Proteins (APPs):
- CRP: Opsonin, classical complement activation. (Produced by liver)
- MBL: Lectin pathway activation. (Produced by liver)
- Antimicrobial Peptides (AMPs):
- Defensins, Cathelicidins: Direct microbicidal, membrane disruption.
- Enzymes:
- Lysozyme: Hydrolyzes peptidoglycan in bacterial cell walls.
⭐ Type I interferons (IFN-α, IFN-β) are crucial for inducing an antiviral state in uninfected cells, limiting viral spread.
Innate Immunity: Recognition & Response - Sensing Danger, Sounding Alarm
-
Sensing Danger (Recognition):
- Microbial PAMPs (LPS, peptidoglycan, viral RNA) & host DAMPs (ATP, HMGB1) detected.
- Key PRRs (Pattern Recognition Receptors):
- TLRs (Toll-like Receptors): Surface (TLR2-peptidoglycan, TLR4-LPS, TLR5-flagellin); Endosomal (TLR3-dsRNA, TLR9-CpG DNA).
- NLRs (NOD-like Receptors): Cytosolic. NOD1/2 (peptidoglycan); NLRP3 (inflammasome → IL-1β/IL-18 via Caspase-1).
- RLRs (RIG-I-like Receptors): Cytosolic. RIG-I/MDA5 (viral RNA → Type I IFN via IRFs).
- CLRs (C-type Lectin Receptors): Dectin-1 (fungal β-glucans).
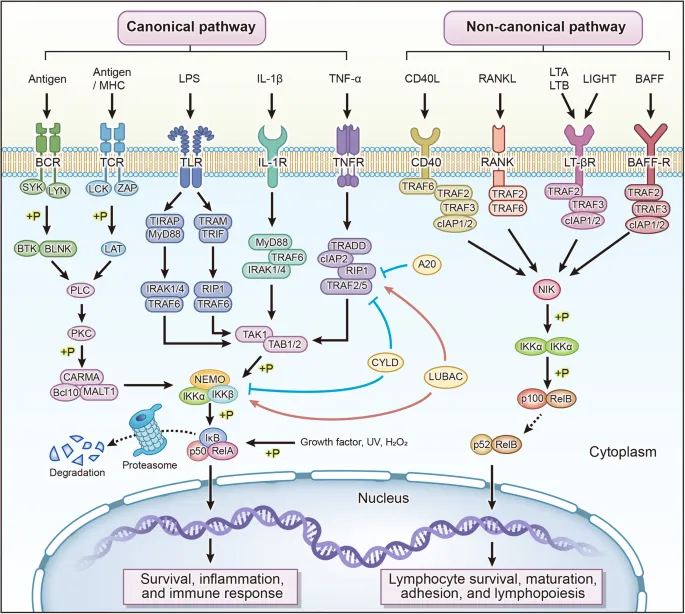
⭐ TLR4 (with CD14/MD-2) recognizes Gram-negative LPS, activating NF-κB for pro-inflammatory cytokine release (TNF-α, IL-1, IL-6).
-
Sounding Alarm (Response):
- Signaling Pathways: NF-κB (pro-inflammatory cytokines, chemokines like CXCL8); IRFs (Type I IFNs: IFN-α/β for antiviral state).
- Key Effector Mechanisms:
- Inflammation: Vasodilation, ↑vascular permeability, neutrophil recruitment.
- Phagocytosis: By macrophages/neutrophils; opsonins (C3b, IgG) enhance.
- Antimicrobial peptides (AMPs): Defensins, cathelicidins.
- NK cell activation.
High‑Yield Points - ⚡ Biggest Takeaways
- Innate immunity is the rapid, non-specific first defense; lacks immunological memory.
- Key players: phagocytes (neutrophils, macrophages), NK cells, complement, cytokines.
- PRRs (e.g., TLRs) on innate cells detect PAMPs (e.g., LPS, viral RNA).
- Inflammation (redness, heat, swelling, pain) is a core innate response.
- Type I interferons (IFN-α/β) are critical for antiviral defense.
- Complement system enhances phagocytosis, causes cell lysis (MAC), and promotes inflammation.
- NK cells provide early defense against viral infections and tumors without prior sensitization.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

