Hypersensitivity Overview - Immune Overdrive Basics
- Exaggerated or inappropriate immune response to an antigen (allergen, autoantigen), resulting in host tissue damage.
- Classified by Coombs & Gell (Types I-IV) based on the underlying mechanism of injury.
- 📌 Mnemonic for types: ACID
- Type I: Allergic / Anaphylactic (IgE-mediated)
- Type II: Cytotoxic (Antibody vs cell surface/matrix antigen)
- Type III: Immune complex (Antigen-Antibody complexes)
- Type IV: Delayed (T-cell mediated)
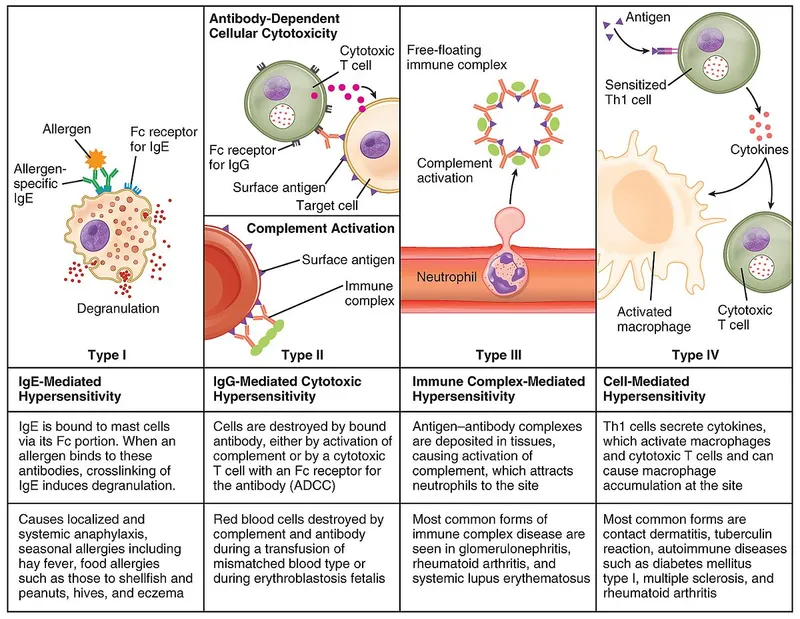
⭐ Type IV is the only purely cell-mediated hypersensitivity; Types I, II, and III are antibody-mediated (humoral immunity).
Type I Reactions - Allergic Alarms
- Immediate hypersensitivity; IgE-mediated. "Allergic" reactions.
- Mechanism:
- Sensitization: Initial allergen exposure → Antigen Presenting Cell (APC) → Th2 cells → IL-4, IL-13 → B cells switch to IgE production → IgE binds FcεRI on mast cells & basophils.
- Re-exposure: Allergen cross-links surface-bound IgE → mast cell/basophil degranulation → release of preformed (histamine, tryptase) & newly synthesized mediators (leukotrienes, prostaglandins).
- Key Mediators: Histamine, tryptase, leukotrienes (LTC4, LTD4, LTE4), prostaglandins (PGD2), cytokines.
- Clinical Examples: Anaphylaxis, allergic asthma, urticaria (hives), allergic rhinitis (hay fever), angioedema.
⭐ Atopy refers to a genetic predisposition to develop localized Type I hypersensitivity reactions (e.g., allergic asthma, eczema, hay fever).
- 📌 Mnemonic: FIRST (Type I), FAST (occurs rapidly), Allergic, Anaphylaxis, Asthma.

Type II Reactions - Cytotoxic Chaos
- Mediators: IgG, IgM antibodies bind to cell surface or ECM antigens.
- Mechanisms (📌 CAD):
- Complement activation: Lysis (MAC), opsonization (C3b).
- Antibody-Dependent Cell-mediated Cytotoxicity (ADCC): NK cells, eosinophils, macrophages.
- Cellular Dysfunction: Antibodies act as receptor agonists (Graves') or antagonists (Myasthenia Gravis).
- Key Examples: AIHA, ITP, Goodpasture's, Rheumatic fever, Transfusion reactions, Erythroblastosis fetalis.

⭐ In Goodpasture syndrome, antibodies target the non-collagenous domain (NC1) of the α3 chain of type IV collagen in glomerular and alveolar basement membranes.
Type III Reactions - Complex Clutter
- Mechanism: Antigen-Antibody (IgG, IgM) immune complexes (ICs) form, deposit in tissues.
- Pathogenesis: ICs activate complement (C3a, C5a chemotaxis). Neutrophils recruited, release lysosomal enzymes → tissue damage (vasculitis, nephritis, arthritis).
- Onset: 3-8 hours (local Arthus) to days/weeks (systemic Serum Sickness).
- Examples:
- Systemic: Serum sickness, SLE, Polyarteritis Nodosa (PAN), Post-Streptococcal Glomerulonephritis (PSGN).
- Local: Arthus reaction, Farmer's lung (Hypersensitivity Pneumonitis).
- 📌 Mnemonic: Imagine 3 components: Antigen, Antibody, Complement.
⭐ Fibrinoid necrosis of vessel walls is a characteristic histological finding in Type III hypersensitivity reactions like Polyarteritis Nodosa.
Type IV Reactions - Delayed Drama
- Cell-mediated; T-lymphocyte (Th1, CTLs) driven. No antibodies involved.
- Delayed onset: 24-72 hours post-antigen exposure.
- Mechanism: Initial sensitization of T-cells. Upon re-exposure, sensitized T-cells (Th1, CTLs) release cytokines (IFN-γ, TNF-α), recruiting and activating macrophages and CTLs, causing localized tissue damage.
- Examples: Tuberculin test (PPD), contact dermatitis (poison ivy, nickel), granulomas (TB), Type 1 DM.
- 📌 Mnemonic: Type 4 = 4 T's: T-cells, Time-delayed, Tuberculin test, Contact dermatitis.

⭐ The Mantoux test, detecting prior TB exposure, relies on measuring induration (not erythema) at 48-72 hours.
High‑Yield Points - ⚡ Biggest Takeaways
- Type I (Anaphylactic): IgE-mediated, rapid mast cell degranulation (e.g., anaphylaxis, allergic asthma).
- Type II (Cytotoxic): IgG/IgM binds cell-surface antigens, complement-mediated lysis (e.g., Goodpasture's, AIHA).
- Type III (Immune Complex): Ag-Ab complexes deposit in tissues, causing vasculitis (e.g., SLE, serum sickness, Arthus reaction).
- Type IV (Delayed-Type): T-cell mediated (Th1 cells activate macrophages), cytokines (e.g., contact dermatitis, PPD test).
- Mnemonic: ACID (Anaphylactic, Cytotoxic, Immune complex, Delayed).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

