VAP: Definition & Epidemiology - Lungs Under Siege
- Pneumonia developing >48 hours after endotracheal intubation.
- Most frequent ICU-acquired infection in mechanically ventilated (MV) patients.
- Affects 9-27% of intubated individuals; ↑ morbidity & mortality.
- Types based on onset:
- Early-onset VAP (EOVAP): <5 days of intubation.
- Usually antibiotic-sensitive bacteria (e.g., S. pneumoniae, MSSA).
- Late-onset VAP (LOVAP): ≥5 days of intubation.
- Often MDR pathogens (e.g., P. aeruginosa, MRSA, Acinetobacter spp.).
- Early-onset VAP (EOVAP): <5 days of intubation.
⭐ LOVAP: ↑ risk of inadequate initial antibiotics & worse outcomes.
VAP: Pathogenesis & Etiology - How Bugs Sneak In
- Pathogenesis:
- Primary: Microaspiration of secretions (oropharyngeal, gastric) past ET tube cuff.
- Biofilm formation on ET tube: Protects bacteria, promotes resistance.
- Others: Contaminated aerosols, rarely hematogenous.
-
Etiology:
Onset Type Timing Common Pathogens Early-onset VAP <5 days S. pneumoniae, H. influenzae, MSSA, antibiotic-sensitive Enterobacteriaceae. Late-onset VAP ≥5 days P. aeruginosa, Acinetobacter spp., MRSA, ESBL-producing GNBs (often MDR). -
Key Risk Factors: Prolonged ventilation, supine positioning, prior antibiotic use, advanced age, stress ulcer prophylaxis (PPIs/H2 blockers).
⭐ Biofilms on endotracheal tubes are a critical factor for VAP development, especially with MDR organisms in late-onset cases.
VAP: Diagnosis - Finding the Foe
- New/progressive lung infiltrate on CXR + ≥2 clinical signs (fever >38°C, leukocytosis/leukopenia, purulent secretions).
- Clinical Pulmonary Infection Score (CPIS): Score >6 suggests VAP.
Component Points Temperature 0-2 WBC Count 0-2 Tracheal Secretions 0-2 Oxygenation (PaO2/FiO2) 0-2 CXR Infiltrate 0-2 Tracheal Aspirate Culture 0-2 - Microbiological confirmation (quantitative cultures preferred):
- Endotracheal Aspirate (ETA): ≥10⁵ CFU/mL
- Bronchoalveolar Lavage (BAL): ≥10⁴ CFU/mL
- Protected Specimen Brush (PSB): ≥10³ CFU/mL

- Diagnostic Algorithm:
(*Fever, ↑WBC, Purulent Secretions)
⭐ Quantitative cultures of lower respiratory tract samples are preferred over qualitative cultures for VAP diagnosis to reduce inappropriate antibiotic use.
VAP: Management - Fighting Back Smart
- Initiate empiric antibiotics promptly (within 1 hour of suspicion).
- Base choice on MDR risk factors & local antibiogram.
- De-escalate therapy based on culture results.
- Typical duration: 7 days.
⭐ Quantitative cultures (e.g., BAL >10,000 CFU/mL, PSB >1,000 CFU/mL) preferred to guide VAP therapy.
VAP: Prevention - Keeping Lungs Clear
VAP prevention focuses on meticulous care bundles. Key elements:
- Head of bed (HOB) elevation: 30-45 degrees continuously.
- Daily sedation interruption ("sedation vacation") & readiness-to-extubate assessment.
- Thorough oral care with chlorhexidine (e.g., 0.12% solution q6-12h).
- Stress ulcer (PUD) prophylaxis.
- Venous thromboembolism (DVT) prophylaxis.
- Maintain endotracheal tube cuff pressure at 20-30 $cm H_2O$.
- Use subglottic secretion drainage (SSD) tubes where possible.
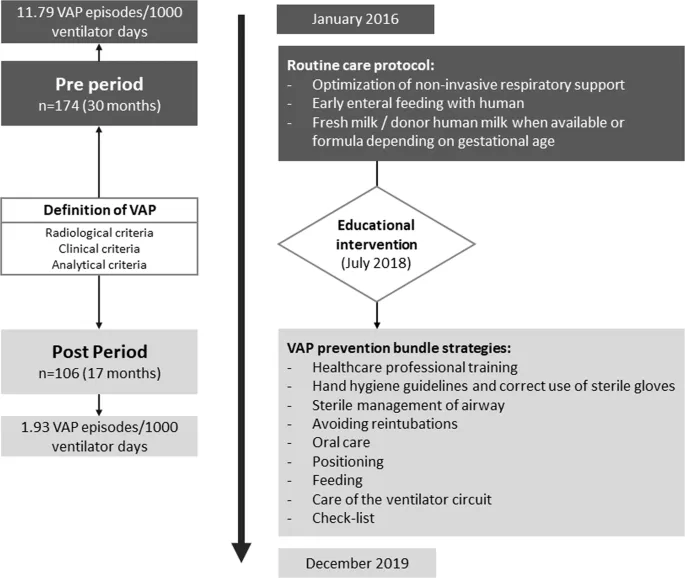
⭐ Consistent application of VAP bundles can decrease VAP rates by over 50%.
High‑Yield Points - ⚡ Biggest Takeaways
- VAP: Pneumonia developing >48 hours post-intubation and mechanical ventilation.
- Common pathogens: P. aeruginosa, Acinetobacter, MRSA, ESBL-producing Enterobacteriaceae.
- Late-onset VAP (≥5 days) strongly associated with MDR organisms.
- Diagnosis: New radiographic infiltrate with clinical signs (fever, purulent sputum) & microbiology.
- Prevention: Key is the VAP bundle (head elevation 30-45°, oral chlorhexidine, sedation holds).
- Treatment: Empiric broad-spectrum antibiotics, then de-escalate based on cultures.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

