Standard Precautions - Baseline Defense Duty
- Applied to ALL patients, always, to prevent infection spread.
- Assumes potential infection from contact with:
- Blood, all body fluids (except sweat), secretions, excretions.
- Non-intact skin, mucous membranes.
- Core actions include:
- Hand Hygiene (e.g., WHO 5 Moments).
- Personal Protective Equipment (PPE): Use gloves, gown, mask, eye protection based on anticipated exposure.
- Respiratory hygiene/Cough etiquette.
- Safe injection practices & sharps management.
- Environmental cleaning & disinfection.

⭐ Standard Precautions apply to ALL patients, regardless of their diagnosis or presumed infection status, and involve contact with blood, body fluids (except sweat), non-intact skin, and mucous membranes.
Contact Precautions - Keep Pathogens Put!
- When? Direct/indirect contact with patient or their environment.
- Key Bugs:
- MDROs (e.g., MRSA, VRE, CRE)
- Clostridioides difficile
- Scabies, pediculosis (lice)
- Infectious diarrhea (e.g., rotavirus, norovirus)
- Major draining wounds or skin infections (e.g., impetigo)
- Actions:
- Private room preferred; cohort with same pathogen if not.
- Gloves & Gown: Don upon entry, discard before exiting room.
- Hand Hygiene: Before gloving, after PPE removal.
- Dedicated or disposable patient-care equipment.
⭐ For Clostridioides difficile, always use soap and water for hand hygiene as alcohol-based sanitizers are not effective against spores.
Droplet Precautions - Dodge the Droplets!
- Spread: Large droplets (>5 µm) from coughs, sneezes; travel ~3-6 feet.
- PPE: Surgical mask if within 3-6 feet. Patient wears mask if transported.
- Room: Single room ideal. Cohort if same pathogen.
- Examples (📌 PIMP My Droplets):
- Pertussis, Pneumonia (Mycoplasma)
- Influenza
- Meningitis (N. meningitidis, H. influenzae type B), Mumps
- Diphtheria (pharyngeal), Rubella
⭐ Droplet precautions require wearing a surgical mask when working within 3-6 feet of a patient with infections like influenza or meningococcal meningitis.
Airborne Precautions - Aerosol Alert Actions
⭐ Airborne precautions for diseases like Tuberculosis or Measles mandate an N95 respirator and placement in an Airborne Infection Isolation Room (AIIR) with ≥12 ACH and negative pressure.
- Patient Placement:
- Single patient room: Airborne Infection Isolation Room (AIIR).
- Monitored negative pressure; ≥12 air changes per hour (ACH).
- Keep door closed.
- Respiratory Protection:
- Fit-tested N95 respirator or higher for healthcare workers (HCWs) entering.
- Patient Transport:
- Limit movement; patient wears surgical mask if transport essential.
- Examples: Tuberculosis, Measles, Varicella. 📌 My Tiny Virus Airborne.
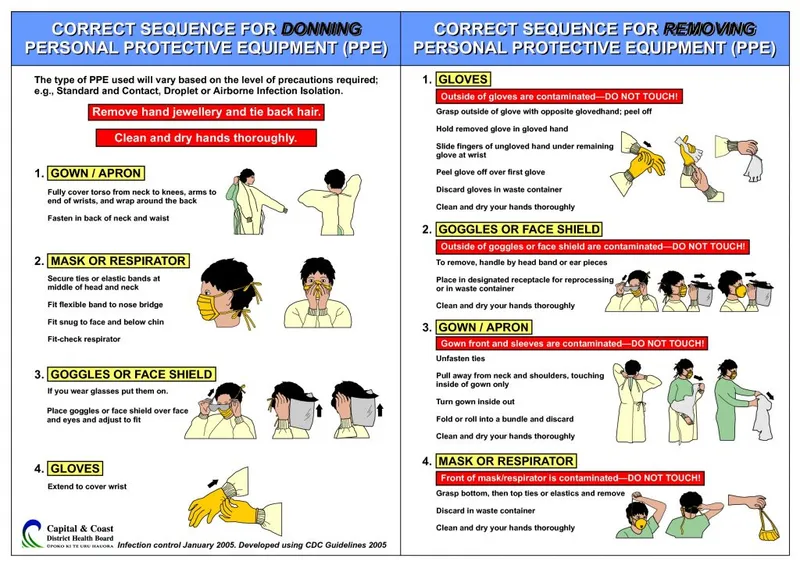
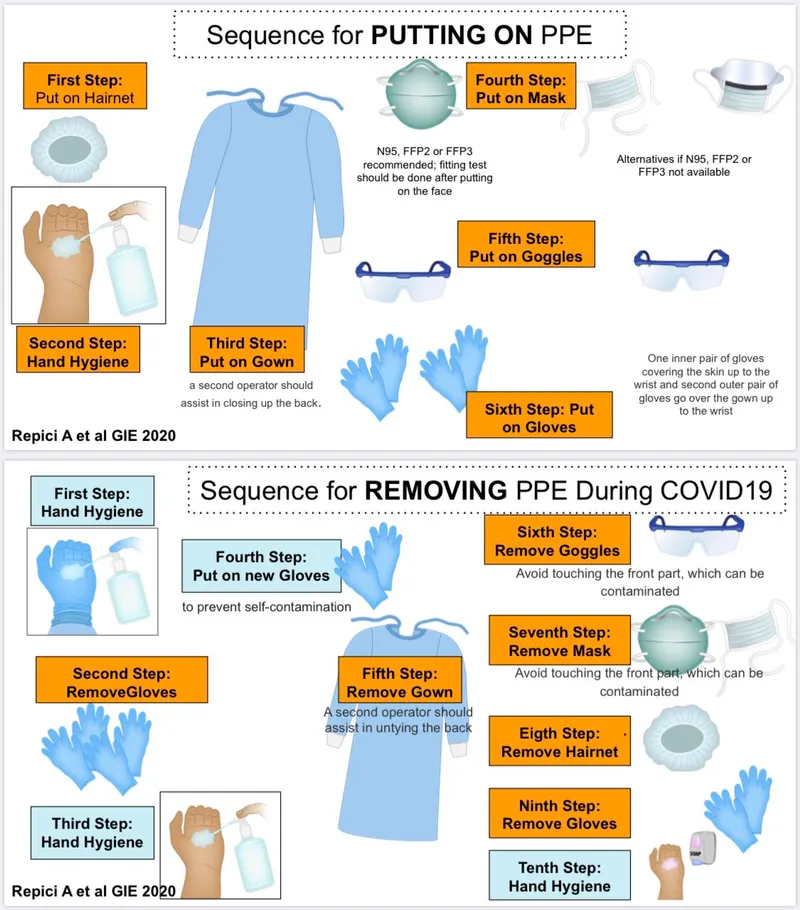
PPE Protocol - Gear Up & Off Right!
Donning (Gear Up) - Order is Key:
- Hand Hygiene: Essential first step.
- Gown: Fully cover torso, tie securely.
- Mask/Respirator: Ensure proper seal (fit check).
- Goggles/Face Shield: Protect eyes and face.
- Gloves: Pull over gown cuffs (last on).
Doffing (Gear Off) - Critical for Safety:
- Perform in designated area, avoid self-contamination.
⭐ Correct sequence of doffing PPE is critical to prevent self-contamination; typically: 1. Gloves, 2. Gown, (Hand Hygiene), 3. Goggles/Face Shield, 4. Mask/Respirator, (Hand Hygiene).
High‑Yield Points - ⚡ Biggest Takeaways
- Standard Precautions: Apply to all patients; key is hand hygiene & appropriate PPE.
- Contact Precautions: For MDROs (e.g., MRSA), C. difficile. Require gloves & gown.
- Droplet Precautions: For influenza, meningitis. Use surgical mask within 3-6 feet.
- Airborne Precautions: For TB, measles, varicella. Need N95 respirator & negative pressure room.
- Hand hygiene is the cornerstone of infection prevention.
- For C. difficile or soiled hands, soap & water is mandatory over alcohol rubs.
- PPE Doffing: Gloves first, mask/respirator last; perform hand hygiene frequently.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

