HICP Basics - Germ Warfare HQ
- Aim: Prevent & control HAIs through a structured program.
- Team Structure:
- HIC Committee (HICC): Multidisciplinary; chaired by institutional head. Sets policies, reviews data.
- Infection Control Officer (ICO): Trained Microbiologist/Physician. Leads HICP, investigates outbreaks.
- Infection Control Nurse (ICN): Ratio 1:250 beds (📌 ICN:250). Conducts surveillance, education, audits.
- Key Activities:
- Surveillance (data collection, analysis, feedback).
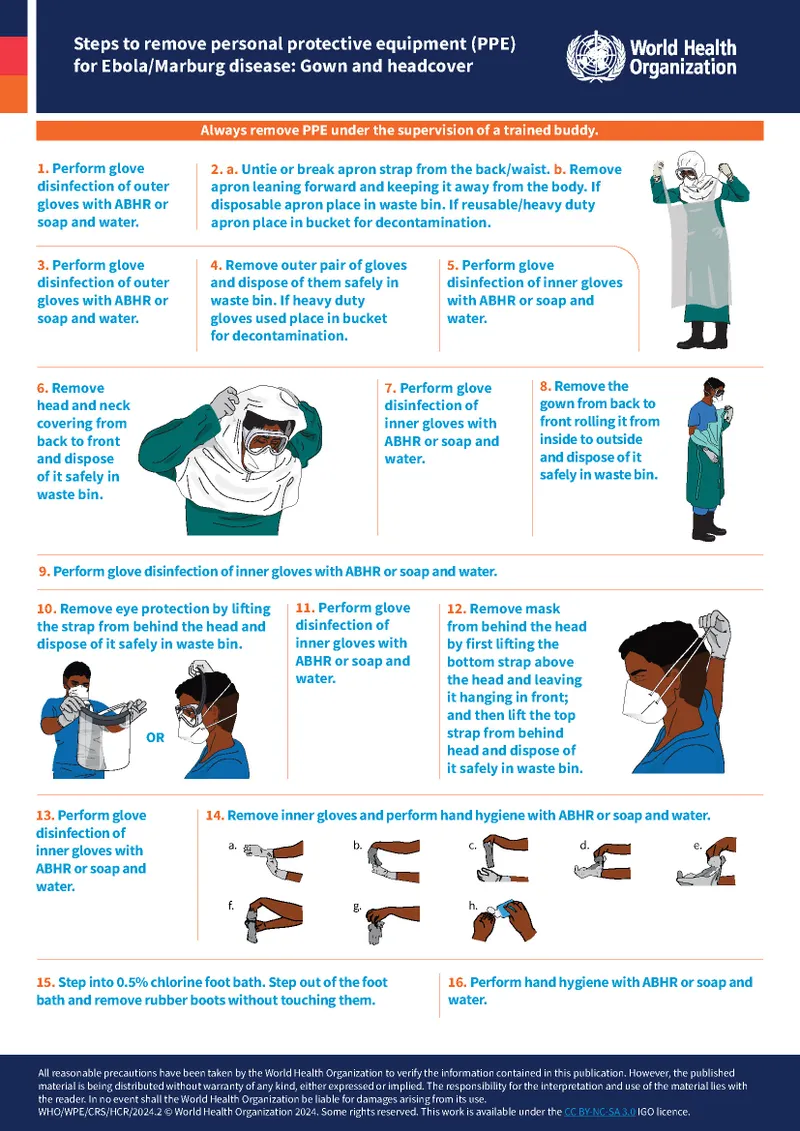
- Adherence to Standard & Transmission-based Precautions.
- Outbreak investigation & control.
- Antimicrobial Stewardship Program (ASP).
- Staff training & environmental hygiene.
⭐ The recommended ratio for Infection Control Nurses (ICNs) is 1 ICN per 250 beds.
Prevention Pillars - Shield Up!
- Hand Hygiene: Cornerstone! 📌 WHO "5 Moments". ABHR (preferred) or soap & water if soiled.
⭐ Hand hygiene is the single most effective measure to prevent HAIs. HCW compliance often <50%.
- Standard Precautions (SP): For ALL patients. Incl. hand hygiene, PPE (risk-based), safe injections, cough etiquette.
- Transmission-Based Precautions (TBP): Added to SP for known/suspected infections.
- Contact: Gown, gloves (MRSA, C. diff).
- Droplet: Surgical mask (Influenza, Meningococcus). Single room/cohort.
- Airborne: N95, AIIR (TB, Measles).
- Environmental Disinfection: High-touch surfaces.
- Antimicrobial Stewardship: Optimize use, ↓resistance.
- HCW Vaccination: Hep B, Flu, MMR.
- Biomedical Waste (BMW) Management: Segregate, treat.
Watch & Act - HAI Detectives
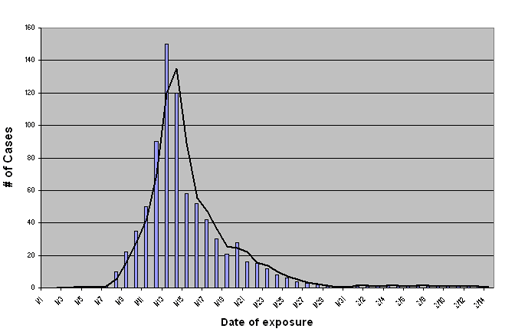
- HAI Surveillance: Systematic collection, analysis, interpretation & dissemination of HAI data for action.
- Types: Active (dedicated staff, higher detection) vs. Passive (routine reporting, underestimation risk).
- Methods: Lab-based, patient-based (chart review), targeted (e.g., ICU, device-days for VAP, CLABSI, CAUTI).
- Key Metrics: Incidence density (e.g., infections per 1000 device-days), Standardized Infection Ratio (SIR).
- Outbreak Investigation: A structured approach.
- Calculate Attack Rates (AR): $\frac{\text{New cases in population}}{\text{Total population at risk}} \times 100$.
- Key Program Activities:
- Regular audits (e.g., hand hygiene, bundle compliance) & feedback.
- Root Cause Analysis (RCA) for significant HAIs/outbreaks.
- Monitoring antimicrobial resistance patterns (Antibiogram).
- Reporting: Crucial for HICC and public health authorities.
⭐ Sentinel surveillance for specific HAIs (e.g., MRSA, C. difficile) in high-risk units provides critical early warnings.
Clean Sweep & Safe Disposal - Zap & Wrap
Essential for HAI prevention: thorough cleaning, disinfection/sterilization, and strict Biomedical Waste (BMW) management.
-
Decontamination Steps:
- Cleaning: Removes visible soil, organic matter. Prerequisite.
- Disinfection: Reduces most pathogens (not all spores).
- High-Level (HLD): e.g., 2% Glutaraldehyde. For semi-critical items (endoscopes).
- Intermediate-Level (ILD): e.g., Alcohols. For non-critical items with blood.
- Low-Level (LLD): e.g., Quats. For environmental surfaces.
- Sterilization: Kills ALL microbial life, including spores.
- Autoclave: Steam, $121^{\circ}C$, 15 psi, 15-20 min.
- Ethylene Oxide (ETO): For heat-sensitive items.
-
BMW Management (Zap & Wrap): Segregate → Treat (Zap) → Dispose (Wrap) 📌 Yellow Red White Blue: Yucky Rubbish Wants Binning!
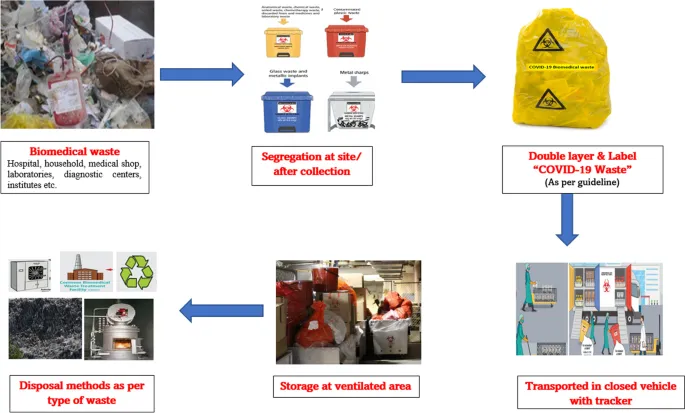
⭐ BMW Rules 2016: Untreated human anatomical waste, animal waste, soiled waste, and biotechnology/microbiological waste must not be stored beyond 48 hours.
High‑Yield Points - ⚡ Biggest Takeaways
Error: Failed to generate content for this concept group.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

