Clean Sweep - Germ Warfare Intro
- Hospital Acquired Infections (HAIs): Significant cause of morbidity & mortality.
- Environment = critical reservoir for pathogens (bacteria, viruses, fungi).
- Fomites (bed rails, IV poles, medical equipment) facilitate cross-transmission.
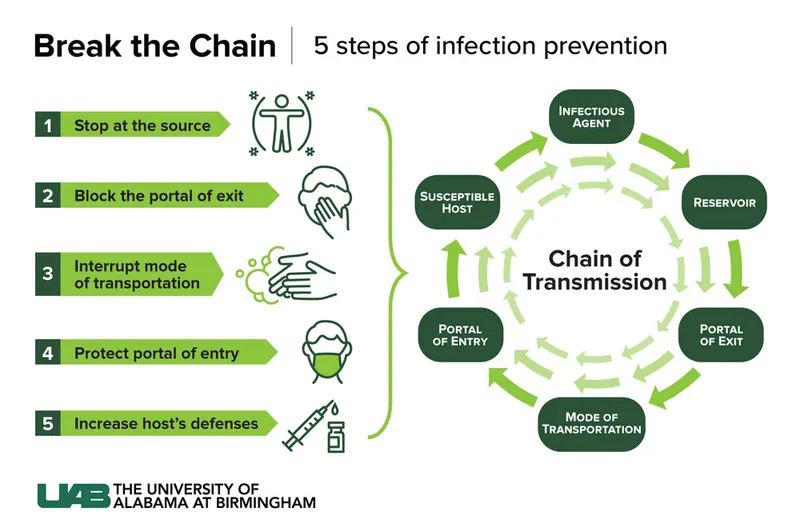
- Goal: Reduce microbial burden, break chain of infection.
- Essential for preventing outbreaks & protecting vulnerable patients.
- Cleaning (physical removal) precedes disinfection (killing microbes).
⭐ Clostridioides difficile spores are highly resistant and require sporicidal disinfectants for effective environmental control, unlike many other vegetative bacteria.
Word Up - Decon Definitions
- Cleaning: Removes visible soil (organic/inorganic) from surfaces. Uses water with detergents/enzymes. Precedes disinfection/sterilization.
- Disinfection: Eliminates most pathogenic microbes (not spores) on objects.
- High-Level (HLD): Kills all microbes, except many spores.
- Intermediate-Level (ILD): Kills M. tuberculosis, bacteria, most viruses/fungi.
- Low-Level (LLD): Kills most bacteria, some viruses/fungi.
- Sterilization: Destroys ALL microbial life, including spores.
- Antisepsis: Applying antimicrobials to living tissue/skin.
⭐ Spaulding's classification categorizes medical devices by infection risk, guiding disinfection/sterilization levels.
Agent Action - Disinfectant Deep Dive
Disinfectants are categorized by their microbial killing efficacy.
- Levels of Disinfection:
- High-Level (HLD): Kills all microorganisms except large numbers of bacterial spores. E.g., Glutaraldehyde, Ortho-phthalaldehyde (OPA), Peracetic acid.
- Intermediate-Level (ILD): Kills vegetative bacteria (including M. tuberculosis), most fungi, and most viruses. E.g., Alcohols, Iodophors, Phenolics.
- Low-Level (LLD): Kills most vegetative bacteria (not TB), some fungi, and some viruses. E.g., Quaternary Ammonium Compounds (QACs).
| Agent | Mechanism | Spectrum | Key Pro(s) | Key Con(s) |
|---|---|---|---|---|
| Alcohols (70% Ethanol/Isopropanol) | Denature proteins | Bact (TB+), Fungi, Vir (env+) | Rapid, no residue | Flammable, inactivated by organic matter |
| Chlorine (Hypochlorite) | Oxidation | Broad; Spores (high conc.) | Cheap, rapid | Corrosive, inactivated by organic matter |
| QACs | Disrupt membrane | Gm+ve > Gm-ve, Vir/Fun (some) | Good cleaning | Inactivated by hard water, resistance |
| Phenolics | Disrupt wall/membrane, proteins | Bact (TB+), Fungi, Vir (some) | Active in organic matter | Skin irritant, residue |
| Glutaraldehyde (2%) | Alkylation | All (sporicidal) | HLD/Sterilant, non-corrosive | Toxic, irritant, long contact (spores) |
| Hydrogen Peroxide (Accelerated) | Free radicals | Broad; Spores (high conc.) | Eco-friendly, rapid HLD | Material compatibility (high conc.) |
⭐ Glutaraldehyde 2% solution requires 6-10 hours of contact time for sterilization (sporicidal action), but significantly less for high-level disinfection of endoscopes (e.g., 20-45 minutes depending on temperature and formulation).
Scrub Strategy - Protocol Playbook
- Protocol: Clean → Disinfect. Top → Down. Cleanest → Dirtiest.
- High-Touch Surfaces (HTS): Bed rails, doorknobs, call bells. Clean ≥2x daily.
- **Spill Management (Blood/Fluids):
- Contain. PPE. Absorb.
- Clean (detergent).
- Disinfect: 1% Sodium Hypochlorite. Contact: 10 min.
- Terminal Cleaning: Thorough cleaning/disinfection post-discharge.
- Disinfectants:
- Alcohols (70%): Small surfaces.
- Chlorine (e.g., hypochlorite): Broad spectrum.
- Quats: Low-level.
⭐ C. difficile spores require sporicidal agents (e.g., 0.1-0.5% sodium hypochlorite); alcohol is ineffective.
Germ Patrol - Audit & Alerts
- Auditing Cleaning:
- Visual inspection: Basic, subjective.
- ATP bioluminescence: Rapidly detects organic matter, indicates cleaning thoroughness.
- Microbial cultures: Swabs/RODAC plates for pathogen detection.
- Alerts & Special Measures:
- C. difficile: Spores resist standard disinfectants; use sporicidal agents (e.g., bleach).
- MDR organisms: Enhanced cleaning, dedicated equipment.
- Outbreak: Intensify cleaning, ↑ audit frequency, terminal disinfection.
⭐ Fluorescent markers (invisible gel/powder) objectively assess cleaning thoroughness by checking removal post-cleaning.
High‑Yield Points - ⚡ Biggest Takeaways
- Cleaning (removal of organic debris) must precede disinfection.
- High-touch surfaces are critical reservoirs; disinfect frequently.
- Sodium hypochlorite (bleach) is broad-spectrum; use 1:10 dilution for C. difficile spores.
- Terminal disinfection of rooms is vital post-discharge, especially for MDROs.
- Contact time and correct dilution are key for disinfectant efficacy.
- Quaternary Ammonium Compounds (Quats) for routine low-level disinfection.
- Alcohol (70%) for small surfaces; ineffective against spores.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

