Sterilization and Disinfection - Defining the Battle
-
Sterilization: Kills ALL microbes, including spores.
-
Disinfection: Kills most pathogens (not spores) on objects.
- Antisepsis: Disinfection of living tissue.
-
Asepsis: Prevents microbial contamination.
-
-cidal: Kills microbes.
-
-static: Inhibits growth.
-
Levels of Disinfection:
- High (HLD): Kills all microbes, some spores (e.g., glutaraldehyde).
- Intermediate (ILD): Kills M. tb, most viruses/fungi; no spores (e.g., alcohol).
- Low (LLD): Kills most bacteria, some viruses/fungi (e.g., Quats).
-
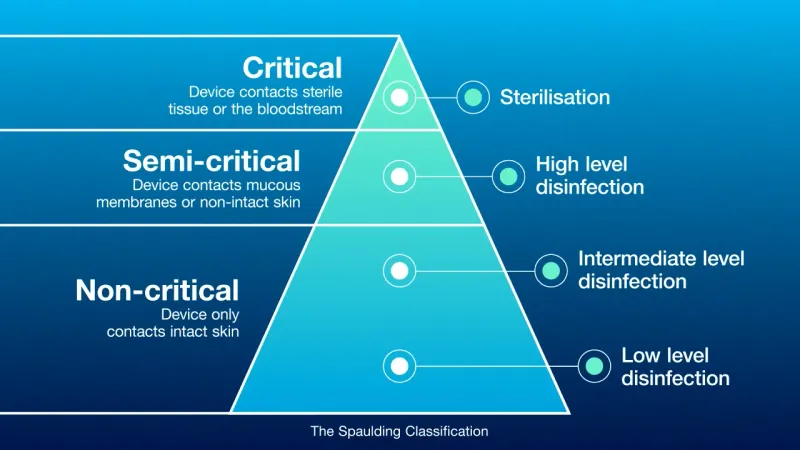
Spaulding's Classification (Item Risk):
- Critical: Sterile tissue entry. Requires Sterilization. (e.g., surgical tools, implants).
- Semi-critical: Mucous membrane/non-intact skin contact. Requires HLD. (e.g., endoscopes, RT equipment).
- Non-critical: Intact skin contact. Requires LLD. (e.g., stethoscopes, BP cuffs).
⭐ Prions are the most resistant infectious agents to standard sterilization methods.
Sterilization and Disinfection - Heat Methods Power
- Dry Heat: Sterilizes by protein denaturation, oxidative damage.
- Hot Air Oven (HAO):
- Parameters: 160°C (2 hrs), 170°C (1 hr), 180°C (30 mins).
- Uses: Glassware, oils, powders, metal instruments (non-cutting).
- Control: Bacillus atrophaeus spores.
- Incineration: Complete combustion.
- Temperature: >800°C.
- Uses: Biomedical waste, infected materials, carcasses.
- Hot Air Oven (HAO):
- Moist Heat: More effective (latent heat of steam); denatures & coagulates proteins.
- Autoclave (Steam under pressure):
- Standard: 121°C, 15 psi pressure, 15-20 mins. Kills spores.
- Uses: Culture media, surgical instruments, dressings, rubber.
⭐ Biological indicator for autoclave efficacy: Geobacillus stearothermophilus spores.
- Pasteurization: Reduces pathogens, not full sterilization.
- Methods: Holder (63°C, 30 min), Flash (72°C, 15-20 sec), UHT (135°C, 1-2 sec).
- Uses: Milk, vaccines, beer.
- Tyndallization (Fractional Sterilization): Steam at 100°C for 20-30 mins, on 3 successive days.
- Uses: Heat-sensitive media (e.g., egg/serum based, sugars).
- Boiling: 100°C for 10-30 mins. Disinfects; kills most vegetative bacteria/viruses. Not reliably sporicidal.
- Autoclave (Steam under pressure):
Sterilization and Disinfection - Other Agents Arsenal
-
Filtration: Removes microbes. Liquids (sera, drugs) via 0.22 µm filters; air via HEPA.
-
Radiation:
- UV (Non-ionizing): Thymine dimers. Surface/air (OTs). Poor penetration.
- Ionizing (Gamma, X-rays): Free radicals. Sterilizes disposables, heat-sensitive items.
-
Chemical Agents:
- Alcohols (Ethanol, Isopropanol): 70%. Denature proteins. Skin antisepsis. Not sporicidal.
- Aldehydes:
- Formaldehyde: Alkylates. Fumigation. Toxic.
- Glutaraldehyde (2%): Alkylates. Sterilant (6-10 hrs for spores). Endoscopes.
- Halogens:
- Iodine (Povidone-iodine): Oxidizes. Skin antiseptic.
- Chlorine (Bleach): Oxidizes. Water/surface disinfection.
- Ethylene Oxide (ETO): Alkylating gas. Heat-sensitive items. Toxic, needs aeration.
⭐ ETO gas sterilizes heat-sensitive items (catheters, scopes); sporicidal but toxic, needs aeration.
- Hydrogen Peroxide ($H_2O_2$): Oxidizing. 3-6% antiseptic; >10% sterilant. Plasma sterilization.
- Phenols (Lysol): Disrupt membranes. Disinfectant.
Sterilization and Disinfection - Control & Checks
- Monitoring Methods:
- Physical: Cycle time, temperature, pressure charts/records.
- Chemical: Indicator tapes (e.g., autoclave tape), Bowie-Dick test (checks pre-vacuum autoclave efficacy).
- Biological (Spore Tests - definitive validation):
- Steam/H₂O₂ plasma: Geobacillus stearothermophilus (spores killed at 121°C).
- Dry heat/Ethylene Oxide (ETO): Bacillus atrophaeus.
- Radiation: Bacillus pumilus.
- Instrument Specifics: Endoscopes require High-Level Disinfection (HLD) e.g., >2% Glutaraldehyde.
- Biomedical Waste (BMW): Must be decontaminated (autoclaved/incinerated) before final disposal.
⭐ Biological indicators (spore tests) are the most reliable method for verifying sterilization efficacy, considered the gold standard for sterility assurance.
High‑Yield Points - ⚡ Biggest Takeaways
- Autoclave (121°C, 15 psi, 15-20 min) is gold standard sterilization, kills spores.
- Hot air oven (160°C, 2 hours) for dry heat sterilization (glassware, oils, powders).
- Glutaraldehyde (2%) is a high-level disinfectant; chemical sterilant with prolonged contact.
- Ethylene oxide gas sterilizes heat-labile items; toxic, carcinogenic.
- Bacillus stearothermophilus spores are biological indicators for autoclave efficacy.
- Bacillus subtilis spores monitor hot air oven and ethylene oxide efficacy.
- Pasteurization (e.g., HTST 72°C, 15 sec) reduces pathogens, not sterilizing.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

