Normal Microbiota - Our Tiny Tenants
- Definition: Resident microbes (commensals) on/in healthy individuals; vital for health.
- Key Sites & Predominant Flora:
- Skin: Staphylococcus epidermidis, Propionibacterium acnes.
- Nasopharynx: S. aureus (carrier), Viridans streptococci.
- Mouth: S. mutans (dental caries), anaerobes (Bacteroides).
- Colon: Highest load ($10^{11}-10^{12}$/g); >95% anaerobes (Bacteroides fragilis, Clostridium); E. coli.
- Vagina: Lactobacillus spp. (maintains acidic pH, protective).
- Beneficial Roles:
- Vitamin K & B synthesis.
- Colonization resistance (vs pathogens).
- Aids immune development.
- Sterile Sites (Normally): Blood, CSF, Lungs (LRT), Bladder, internal organs.
- Dysbiosis & Pathogenicity:
- Dysbiosis: Imbalance in flora; can cause disease.
- Opportunistic infections: Flora pathogenic if host immunocompromised or flora displaced.
⭐ Bacteroides fragilis: most common colon anaerobe; causes intra-abdominal infections if displaced.
Pathogenicity & Virulence - Villains' Toolkit
-
Pathogenicity: Ability to cause disease.
-
Virulence: Degree of pathogenicity. $LD_{50}$ (Lethal Dose): ↓ = ↑ virulence.
-
Infectivity: Ability to colonize. $ID_{50}$ (Infectious Dose): ↓ = ↑ infectivity.
-
Virulence Factors (Arsenal):
- Adhesion: Critical for colonization.
- Pili, adhesins (M protein - S. pyogenes, Opa protein).
- Invasion & Spread: Aid tissue penetration.
- Enzymes: Hyaluronidase, collagenase, coagulase, kinases, DNase.
- Evasion of Host Defenses:
- Capsules (S. pneumoniae): Antiphagocytic, mask PAMPs.
- Biofilms: Resist antibiotics/phagocytosis.
- Antigenic variation (Influenza).
- IgA proteases.
- Toxins:
- Exotoxins: Secreted proteins (G+/G-). Potent, specific. Mostly heat-labile. Toxoids (vaccines). Plasmid/phage coded.
- Types: A-B (Diphtheria, Cholera), membrane-disrupting (lecithinase), superantigens (TSST-1).
- Endotoxins: Lipid A (LPS of G-). Released on lysis. Fever, DIC, shock (TNF-α, IL-1). Heat-stable. No toxoids.
⭐ Lipid A of LPS is the endotoxin component of Gram-negative bacteria, responsible for septic shock.
- Exotoxins: Secreted proteins (G+/G-). Potent, specific. Mostly heat-labile. Toxoids (vaccines). Plasmid/phage coded.
- Adhesion: Critical for colonization.
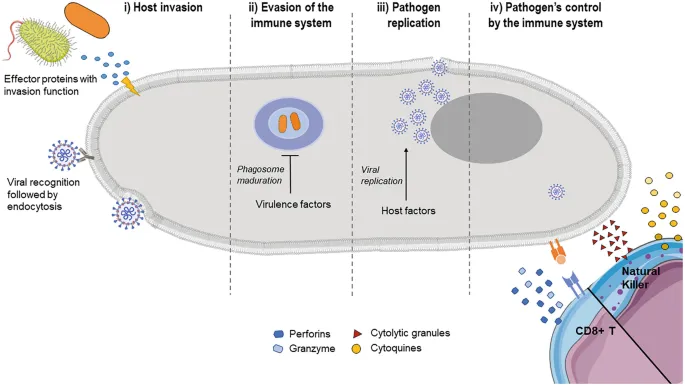
Host-Pathogen Tango - Infection Unfolded
Dynamic interplay: invading microbes vs. host defenses, shaping infection's course and outcome.
- Infection Unfolds:
- Entry: Via portals (e.g., respiratory, GI). Adherence via adhesins.
- Invasion & Spread: Localized or systemic dissemination.
- Multiplication: Colonization, often evading host immunity (e.g., capsules, biofilms).
- Damage: Caused by pathogen (toxins, enzymes) or host response (immunopathology).
- Critical Factors:
- Pathogen: Virulence factors, inoculum size (ID₅₀).
- Host: Immune status, genetic susceptibility, age.
- Possible Outcomes:
- Resolution, asymptomatic carrier, latency, chronic disease, or death.
⭐ Infectious Dose 50 (ID₅₀) is the number of organisms needed to infect 50% of exposed individuals. A lower ID₅₀ indicates greater virulence.
Opportunistic Infections - Friends Turned Foes
- Commensals or low-virulence microbes causing disease when host defenses are weakened.
- Key predisposing factors:
- Immunodeficiency (e.g., HIV, chemotherapy, steroids).
- Disruption of normal flora (e.g., broad-spectrum antibiotics → C. difficile).
- Breached anatomical barriers (e.g., trauma, surgery, catheters, burns).
- Common examples:
- Candida albicans (oral thrush, vulvovaginitis).
- Staphylococcus epidermidis (catheter-related infections, endocarditis).
- Pseudomonas aeruginosa (burn wounds, ventilator-associated pneumonia).
- Pneumocystis jirovecii (PCP pneumonia in AIDS patients).
⭐ Pseudomonas aeruginosa is notorious for causing infections in burn patients and individuals with cystic fibrosis.
- 📌 Remember SPACE organisms for nosocomial infections (often opportunistic): Serratia, Pseudomonas, Acinetobacter, Citrobacter, Enterobacter.
High‑Yield Points - ⚡ Biggest Takeaways
- Normal microbiota offers colonization resistance, preventing pathogen invasion.
- Opportunistic pathogens primarily infect immunocompromised individuals or disrupted microbiota sites.
- Pathogenicity is the capacity to cause disease; virulence quantifies this capacity.
- Adherence via structures like pili and adhesins is critical for infection initiation.
- Exotoxins (secreted proteins) and endotoxins (LPS of Gram-negatives) are key virulence factors.
- Biofilms contribute to chronic infections and increased antimicrobial resistance.
- Koch's postulates are criteria to link a specific microbe to a specific disease.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more



