Intro to Interactions - Microbial Mingling
Microorganisms constantly interact, influencing ecological balance and host health.
| Interaction | Effect | Description |
|---|---|---|
| Neutralism | (0/0) | Neither population affected. |
| Mutualism | (+/+) | Both benefit; obligatory. |
| Commensalism | (+/0) | One benefits; other unaffected. |
| Synergism | (+/+) | Both benefit; not obligatory (protocooperation). |
| Competition | (-/-) | Both inhibited striving for same resource. |
| Amensalism | (-/0) | One inhibited; other unaffected. |
| Parasitism | (+/-) | Parasite benefits; host harmed. |
| Predation | (+/-) | Predator engulfs/kills prey. |
⭐ Quorum sensing, a cell-density dependent communication, often mediates complex microbial interactions.
Beneficial Alliances - Win-Win & Win-Neutral
-
Mutualism (+/+): Both benefit; obligatory.
- Lichens: Fungus + Alga/Cyanobacterium. 📌 Lichens Love MycoRhizae.
- Mycorrhizae: Fungi + Plant roots (nutrient exchange).
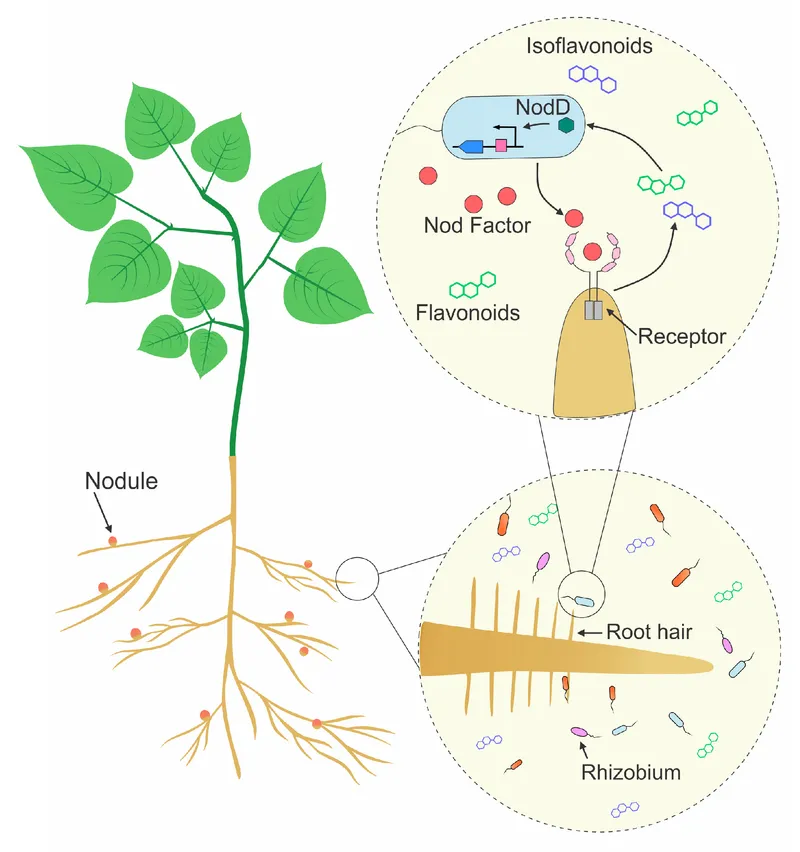
- Root nodules: Legumes + N₂-fixing Rhizobium; $N_2 \rightarrow NH_3$.
-
Synergism (+/+): Both benefit; non-obligatory.
- Lactobacillus + Enterococcus (e.g., complete amino acid synthesis).
- Azotobacter (aerobe) + Clostridium (anaerobe) for soil N₂ fixation.
-
Commensalism (+/0): One benefits; other unaffected.
- Gut E. coli creates anaerobic state for Bacteroides.
- Facultative anaerobes deplete $O_2$, aiding obligate anaerobes.
⭐ Rhizobium-legume mutualism (N₂ fixation) is a classic, vital example for agriculture.
Antagonistic Encounters - Microbial Warfare
Microbes harm/inhibit others; vital for ecological balance, disease.
- Competition: Struggle for limited resources (nutrients, space, light).
- Example: P. fluorescens outcompetes for iron using siderophores.
- Amensalism (Antibiosis): One produces inhibitors (e.g., antibiotics, bacteriocins, acids) harming others.
- Example: Streptomyces spp. (antibiotics); Lactic acid bacteria (acids).
- Predation: Predator actively attacks, engulfs & consumes prey.
- Example: Bdellovibrio drills into, replicates in periplasm of Gram-negatives.
- Parasitism: Parasite lives on/in host, deriving nutrients & causing harm.
- Example: Bacteriophages (bacteria); Chlamydia (intracellular human cells).
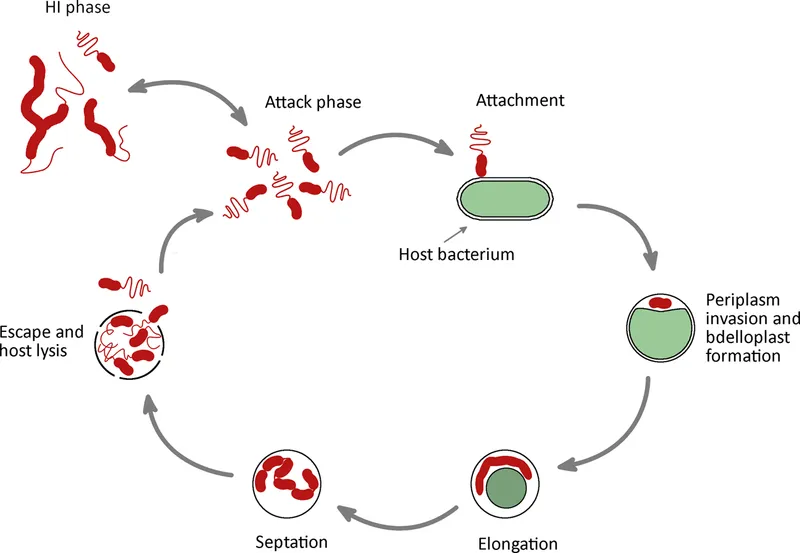
⭐ Bdellovibrio bacteriovorus is a unique bacterial predator, notable for its periplasmic replication within prey, making it a potential "living antibiotic".
Biofilms & Quorum Sensing - United We Stand, Talk We Must
- Biofilms: Structured microbial communities encased in a self-produced Extracellular Polymeric Substance (EPS) matrix.
- Adherent to biotic/abiotic surfaces; offer ↑ resistance to antimicrobials & host immune responses.
- Key in persistent infections (e.g., medical devices, cystic fibrosis lungs).
- Quorum Sensing (QS): Bacterial cell-to-cell communication; population density-dependent gene regulation.
- Autoinducers (e.g., Acyl-Homoserine Lactones - AHLs in Gram-neg; Autoinducing Peptides - AIPs in Gram-pos) trigger collective behaviors.
- Governs biofilm formation, virulence factor production. 📌 QBS: Quorum sensing Builds Strong biofilms.
⭐ Pseudomonas aeruginosa utilizes multiple QS systems (e.g., Las, Rhl, PQS) to control biofilm development and the expression of numerous virulence factors, making it a prime target for anti-biofilm strategies in chronic infections.
High‑Yield Points - ⚡ Biggest Takeaways
- Symbiosis (mutualism, commensalism, parasitism) dictates microbial ecosystem structure and host interactions.
- Biofilms, structured microbial communities, offer protection and ↑ antibiotic resistance.
- Quorum sensing coordinates bacterial group behaviors like virulence and biofilm development.
- Microbes are essential for biogeochemical cycles (e.g., nitrogen fixation, carbon, sulfur).
- Antagonism (e.g., antibiotic production by Streptomyces) influences microbial community composition.
- Horizontal Gene Transfer (HGT) in environmental microbes spreads antibiotic resistance and virulence factors.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

