Aquatic Habitats & Microbes - Diverse Water Worlds
- Freshwater Systems:
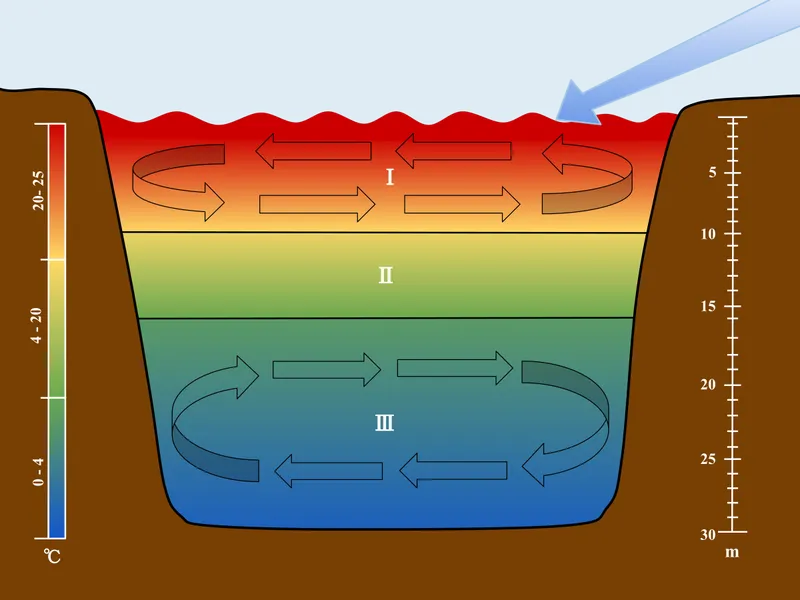
- Lakes (lentic): Exhibit thermal stratification.
- Epilimnion (surface): Aerobic; cyanobacteria, algae, heterotrophic bacteria.
- Hypolimnion (bottom): Anaerobic; methanogens, sulfate-reducers.
- Rivers (lotic): Dynamic; biofilms on surfaces, influenced by terrestrial input.
- Lakes (lentic): Exhibit thermal stratification.
- Marine Systems:
- Oceans: Vast, diverse zones.
- Photic zone: Dominated by phytoplankton (e.g., Prochlorococcus, diatoms), viral lysis common.
- Aphotic/Deep sea: High pressure (piezophiles), low temperature (psychrophiles); chemolithoautotrophy at hydrothermal vents.
- Estuaries: Brackish, fluctuating salinity; high microbial activity.
- Oceans: Vast, diverse zones.
- Groundwater: Often oligotrophic; unique chemolithoautotrophs.
⭐ Prochlorococcus, a picocyanobacterium, is the smallest and most abundant photosynthetic organism on Earth, responsible for a large fraction of marine primary production.
Water Quality & Indicators - Tiny Health Monitors
- Indicator Organisms: Microbes whose presence signals potential faecal contamination & associated pathogens.
- Ideal: Easy to detect, non-pathogenic, survives like pathogens, faecal-specific.
- Key Indicators:
- Total Coliforms: General hygiene indicator.
- Faecal Coliforms: Thermotolerant (grow at 44.5°C), indicate faecal origin.
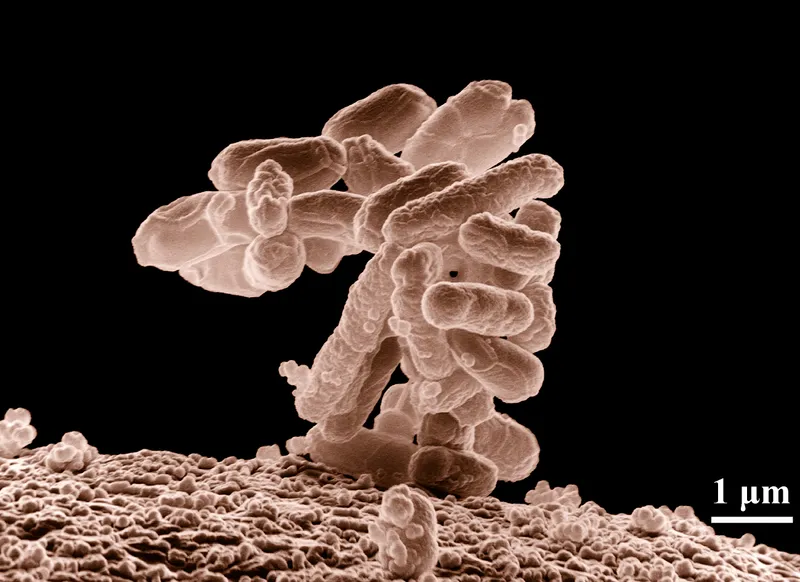
- Escherichia coli: Specific to faecal contamination; most reliable.
- Faecal Streptococci (Enterococci): Indicate faecal pollution, more resistant.
- Clostridium perfringens: Spores indicate past/intermittent pollution.
- Testing Methods:
- MPN (Most Probable Number): Estimates density.
- Membrane Filtration: Direct viable count.
- Presence-Absence Test.
- IMViC: Differentiates E. coli.
⭐ Escherichia coli is the most reliable indicator of recent faecal pollution in drinking water due to its exclusive faecal origin and shorter survival time outside the host.
Waterborne Pathogens - Invisible Threats Lurking
Contaminated water harbors diverse pathogens. 📌 Key Types: Bacteria, Viruses, Protozoa.
- Bacteria:
- Vibrio cholerae: Cholera ("rice-water stools", severe dehydration)
- Salmonella typhi: Typhoid fever (step-ladder pyrexia, rose spots)
- Shigella spp.: Shigellosis (bacillary dysentery, tenesmus)
- E. coli (ETEC, EHEC): Diarrhea (traveler's, HUS from O157:H7)
- Campylobacter jejuni: Gastroenteritis (common, Guillain-Barré link)
- Leptospira interrogans: Leptospirosis (Weil's disease: jaundice, renal failure)
- Viruses:
- Hepatitis A & E: Acute viral hepatitis (fecal-oral)
- Rotavirus: Severe infantile diarrhea (vaccine-preventable)
- Norovirus: Epidemic gastroenteritis ("winter vomiting bug")
- Protozoa:
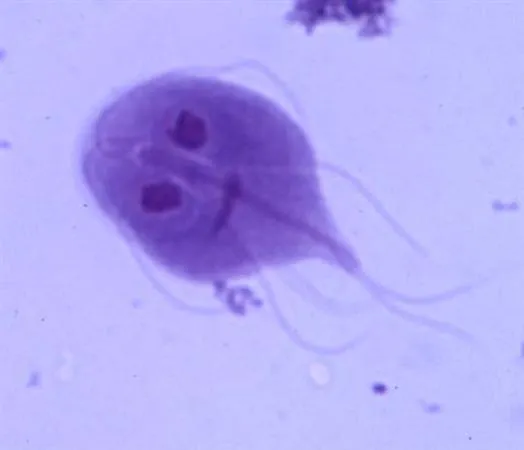
- Giardia lamblia: Giardiasis (foul-smelling steatorrhea, "beaver fever")
- Entamoeba histolytica: Amoebiasis (dysentery, liver abscess)
- Cryptosporidium parvum: Cryptosporidiosis (watery diarrhea, severe in AIDS CD4 < 100)
⭐ Hepatitis E virus (HEV) infection in pregnant women (3rd trimester) carries high mortality (up to 20-30%).
Biofilms & Water Treatment - Slime & Shine
- Biofilms: Structured microbial communities encased in self-produced Extracellular Polymeric Substance (EPS), offering protection.
- Formation Stages: Attachment → Colonization (Quorum Sensing vital) → Maturation (complex 3D architecture) → Dispersal.
- Significance: ↑ Antimicrobial resistance (e.g., Pseudomonas), persistent infections, medical device/pipe biofouling.
- Water Treatment Process: Essential multi-barrier approach for safe drinking water.
- Key Disinfection Methods:
- Chlorination: Must achieve breakpoint for adequate free residual chlorine.
- UV Radiation: Damages microbial DNA, preventing replication.
- Ozone ($O_3$): Powerful, broad-spectrum oxidizing agent.
⭐ Breakpoint chlorination is critical: chlorine demand satisfied, further addition gives proportional free residual chlorine (target 0.2-0.5 mg/L) for sustained disinfection.
📌 Smart Chemists Study Fluids Diligently (Screening, Coagulation, Sedimentation, Filtration, Disinfection)
High‑Yield Points - ⚡ Biggest Takeaways
- Indicator organisms (e.g., E. coli) signal fecal contamination and assess water quality.
- Key waterborne diseases: cholera, typhoid, hepatitis A/E, shigellosis.
- Biofilms in water systems harbor pathogens, aiding antimicrobial resistance.
- Eutrophication causes algal blooms; some produce cyanotoxins.
- Legionella pneumophila in water systems causes Legionnaires' disease.
- Leptospirosis is transmitted via water contaminated with infected animal urine.
- Water purification (chlorination, filtration) is vital for disease prevention.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

