Pandemic Basics - Defining Disaster
- Endemic: Disease consistently present in a specific geographic area or population.
- Epidemic: Sudden increase (↑) in disease cases above normal expectations in an area.
- Pandemic: An epidemic that has spread across multiple countries or continents, affecting many people.
- 📌 PANDEMIC = People All Nations Disease Exposed Massively Infecting Continents.
| Feature | Epidemic | Pandemic |
|---|---|---|
| Scope | Local/Regional | Global/Widespread |
| Spread | Rapid, but usually contained | Rapid, crosses intl. borders |
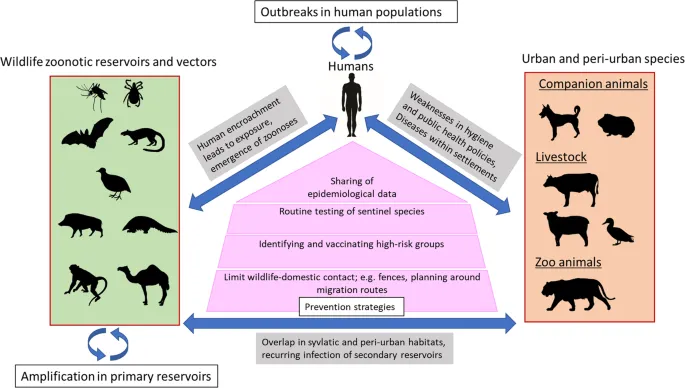
- Spillover: Event where a pathogen jumps from an animal reservoir to a human host.
- Key Historical Pandemics: Plague; Cholera (significant Indian context, multiple pandemics); Influenza (e.g., 1918 H1N1, 2009 H1N1); COVID-19.
⭐ A disease outbreak is declared a Public Health Emergency of International Concern (PHEIC) by the WHO Director-General based on criteria outlined in the International Health Regulations (IHR 2005).
Early Warnings - Spotting Spark
- IHR (2005): Global framework for disease spread. PHEIC declaration by WHO: criteria include serious, unusual, significant international spread risk, potential travel/trade restrictions. Report potential PHEIC: 24 hours.
- IDSP India: National surveillance. 📌 IDSP = Integrated Data Saves Populations.
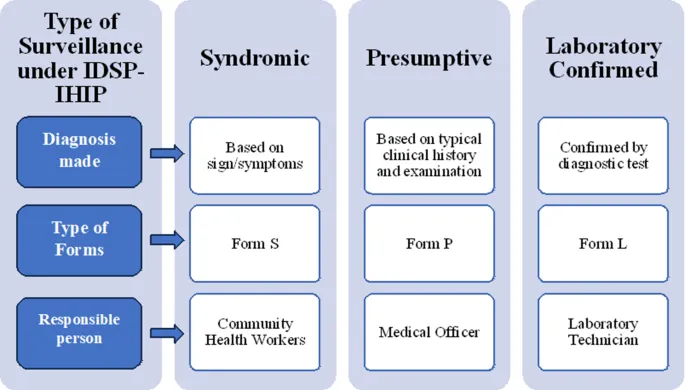
- Forms: S (Syndromic), P (Presumptive), L (Lab-confirmed).
⭐ India's Integrated Disease Surveillance Programme (IDSP) collects data on epidemic-prone diseases through weekly reporting from health facilities (S-form for syndromic, P-form for presumptive, L-form for laboratory-confirmed cases).
- NCDC: Apex body; coordinates IDSP, outbreak investigation.
- Lab Networks: VRDLs (Virus Research and Diagnostic Laboratories) for diagnosis.
- Biosafety:
- BSL-3: Serious/lethal aerosol agents.
- BSL-4: High-risk, life-threatening aerosol agents, no vaccine/treatment.
Action Stations - Gearing Globally
- WHO Pandemic Influenza Preparedness (PIP) Framework: Ensures equitable vaccine access & virus sharing.
- National Disaster Management Authority (NDMA) Guidelines: India's framework for biological disaster management.
⭐ The National Disaster Management Plan (NDMP) of India outlines roles and responsibilities for managing biological hazards, including pandemics, with emphasis on a multi-sectoral approach.
- Core Preparedness:
-
Stockpiling: PPE, antivirals, vaccines.
-
Surge Capacity: ↑ Hospital beds, workforce.
-
Risk Communication: Transparent & timely public information.
-
- WHO Pandemic Phases: 📌 In A Pandemic, Transition!
| Phase | Key Actions |
|---|---|
| Interpandemic | Preparedness, surveillance, capacity building. |
| Alert | Risk assessment, initial containment, vigilance. |
| Pandemic | Mitigation strategies, treatment, community care. |
| Transition | De-escalation, recovery, review. |
Fighting Back - Tools & Tactics
-
Non-Pharmaceutical Interventions (NPIs): 📌 Stay home, Mask up, Avoid crowds, Rinse hands, Travel wisely (SMART).
- Quarantine, isolation, social distancing.
- School/workplace closures, travel restrictions.
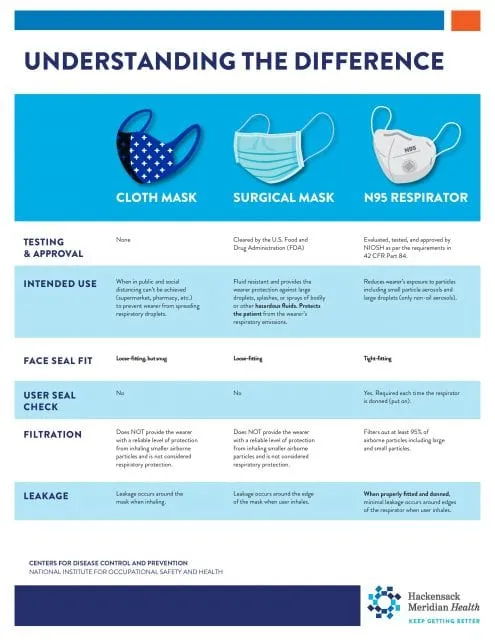
- Hand hygiene, masks (types & efficacy).
-
Table: Quarantine vs. Isolation
Feature Quarantine Isolation Target Exposed, asymptomatic individuals Confirmed cases (symptomatic/asymptomatic) Purpose Prevent spread if infected Prevent spread from known infected Typical Duration E.g., 14 days (incubation) Duration of infectivity -
Pharmaceutical Interventions (PIs):
- Antivirals: E.g., Oseltamivir (influenza).
- Vaccines: Development stages; Types: Live attenuated, inactivated, subunit, mRNA.
-
Contact Tracing: Identify & manage contacts.
⭐ Ring vaccination, a strategy of vaccinating contacts and contacts of contacts of confirmed cases, was a key tactic in the eradication of smallpox and can be used for other diseases.
High‑Yield Points - ⚡ Biggest Takeaways
- IHR (2005): Global framework for PHEIC; mandates core capacities (surveillance, response).
- WHO Pandemic Phases (Interpandemic, Alert, Pandemic, Transition) guide global actions.
- Surveillance (e.g., IDSP) is critical for early detection and tracking of outbreaks.
- One Health Approach: Links human, animal, environmental health to combat zoonoses.
- Rapid Response Teams (RRTs) and stockpiling (vaccines, PPE) are vital for effective response.
- Risk communication is key for public trust and adherence to control measures.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

