Free-Living Amoebae - Brain Invaders & Eye Ills
| Amoeba | Entry Route | Key Disease(s) | Key Dx/Feature | Rx Highlights |
|---|---|---|---|---|
| Naegleria fowleri | Nasal (warm freshwater) | PAM (acute, fulminant) | Motile trophozoites in CSF (no cysts in tissue) | Amphotericin B (IV+IT), Miltefosine |
| Acanthamoeba spp. | Cornea, skin, lungs | GAE (chronic), AK | Cysts (double-walled) & trophozoites (biopsy) | AK: Topical biguanides; GAE: Miltefosine |
| Balamuthia mandrillaris | Skin, respiratory | GAE (chronic) | Cysts & trophozoites (biopsy) | Miltefosine, combination therapy |
⭐ Naegleria fowleri causes Primary Amoebic Meningoencephalitis (PAM), a rapidly fatal infection typically from warm freshwater swimming.
- PAM: Rapid onset fever, headache, nuchal rigidity, AMS; death in 1-2 weeks.
- GAE: Insidious onset; focal deficits, seizures, headache; common in immunocompromised.
- Acanthamoeba Keratitis (AK): Severe eye pain (out of proportion), photophobia; ring infiltrate (late). 📌 Risk: Improper contact lens care.
Emerging Coccidians - Diarrhea Dynamos
Emerging coccidian protozoa causing significant, often profuse, watery diarrhea, particularly severe in immunocompromised individuals.
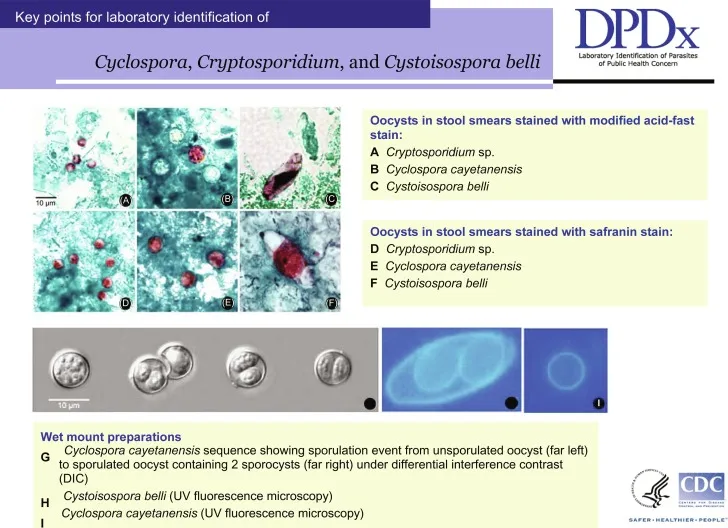
| Feature | Cryptosporidium spp. | Cyclospora cayetanensis |
|---|---|---|
| Oocyst Size | 4-6µm | 8-10µm |
| MAF Stain | Positive (red-pink oocysts) | Positive (variable staining, often ghosts) |
| Autofluorescence | No | Yes (blue/green under UV light) |
| Clinical | Acute, profuse watery diarrhea; chronic in immunocompromised | Prolonged, relapsing watery diarrhea, fatigue, anorexia |
| Transmission | Fecal-oral (water, food, zoonotic); low infective dose | Fecal-oral (imported fresh produce, water) |
- Management: Nitazoxanide (for both; especially immunocompetent for Crypto); supportive care (rehydration).
- 📌 Mnemonic: Crypto is smaller; Cyclo cycles (autofluoresces & larger).
⭐ Cryptosporidium parvum is highly resistant to standard chlorine disinfection in water supplies.
Emerging Helminths - Wandering Worms
- Focus on tissue-invasive helminths with distinct clinical presentations.
| Feature | Angiostrongylus cantonensis (Rat Lungworm) | Dirofilaria spp. (Dog Heartworm) | Gnathostoma spinigerum (Spinigerous Gnathostome) |
|---|---|---|---|
| Transmission | Ingestion of raw/undercooked snails/slugs, contaminated produce | Mosquito bite (zoonotic, humans are dead-end hosts) | Ingestion of raw/undercooked freshwater fish, frogs, poultry |
| Key Syndrome | Eosinophilic meningitis (severe headache, paresthesia) | Solitary pulmonary nodules ("coin lesion"), subcutaneous nodules | Larva migrans (cutaneous or visceral), migratory swellings, neurological signs |
| Diagnostic Clues | CSF eosinophilia (>10%), history of exposure, serology (limited) | Imaging (X-ray, CT), serology, biopsy of nodule | Peripheral eosinophilia, history, serology, recovery of larva |
| Management | Supportive, corticosteroids for severe inflammation; antihelminthics controversial | Surgical excision of nodules; antihelminthics usually not needed | Surgical removal, albendazole/ivermectin (may reduce symptoms) |
⭐ Angiostrongylus cantonensis is a leading cause of eosinophilic meningitis globally.
📌 Mnemonic (A.D.G. for syndromes): Angio Meningitis, Dirofilaria Nodules, Gnathostoma Migrans.
High‑Yield Points - ⚡ Biggest Takeaways
- Naegleria fowleri: Causes fatal Primary Amoebic Meningoencephalitis (PAM) from warm freshwater contact.
- Acanthamoeba: Leads to keratitis (contact lens) and Granulomatous Amoebic Encephalitis (GAE) (immunocompromised).
- Cyclospora cayetanensis: Causes prolonged diarrhea linked to fresh produce; its oocysts are acid-fast.
- Microsporidia: Induce chronic diarrhea in HIV/AIDS patients; use modified trichrome stain for spores.
- Babesia microti: Transmitted by Ixodes ticks; causes malaria-like illness, Maltese cross in RBCs.
- Balamuthia mandrillaris: Results in GAE and skin lesions; affects immunocompetent and compromised_ individuals_
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

