Intro: Emerging Infections - New Bugs on Block
- Emerging Infections: Newly identified in a population or those with rapidly ↑ incidence or geographic spread.
- Re-emerging Infections: Previously controlled infections now reappearing or ↑ in incidence (e.g., Diphtheria).
- Key Factors Driving Emergence:
- Microbial adaptation (e.g., genetic mutations, antimicrobial resistance)
- Human demographics & behavior (e.g., urbanization, international travel)
- Ecological changes (e.g., deforestation, climate change)
- Breakdown in public health measures (e.g., ↓ surveillance, ↓ vaccination rates)
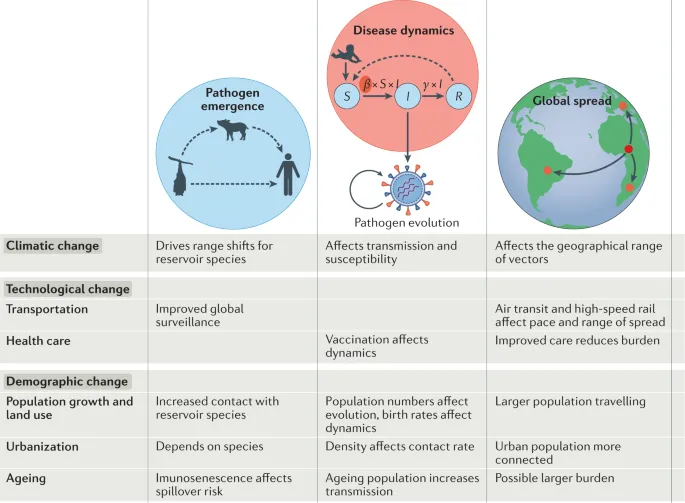
⭐ Antimicrobial resistance (AMR) is a primary engine for the rise of both emerging and re-emerging bacterial infections globally, complicating treatment and control efforts significantly.
Gram-Positive Threats - Super Staph & C.diff Clout
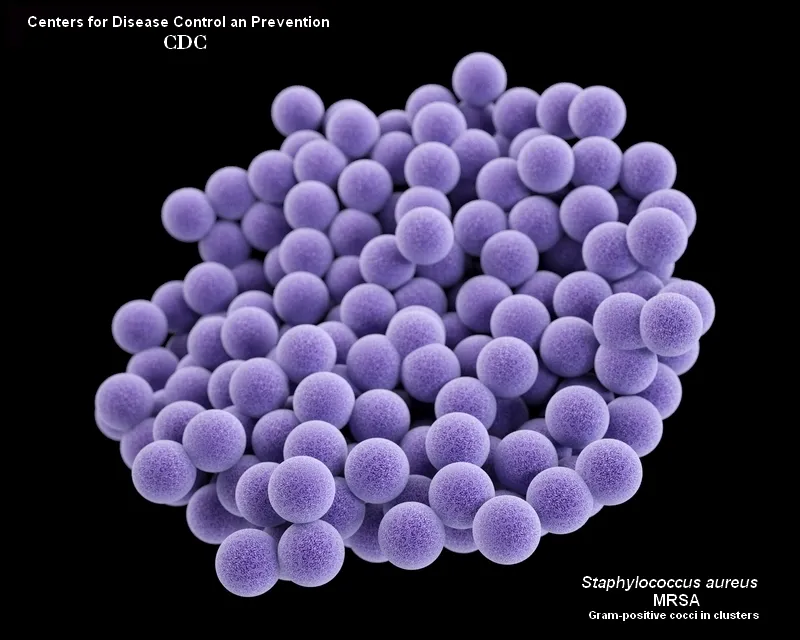 and Gram-positive rods (Clostridioides difficile) microscopy)
and Gram-positive rods (Clostridioides difficile) microscopy)
1. MRSA (Methicillin-Resistant S. aureus)
- CA-MRSA vs. HA-MRSA:
Feature CA-MRSA HA-MRSA Virulence PVL+ (SSTIs, necro. pneumonia) PVL often - SCCmec IV, V I, II, III Rx Sensitivity Better to non-β-lactams Multi-drug resistant - PVL (Panton-Valentine Leukocidin): CA-MRSA virulence, pore-forming.
- Treatment (severe): Vancomycin, Linezolid, Daptomycin.
2. Hypervirulent Clostridioides difficile
- Strain: NAP1/BI/027 - ↑ FQ resistance, ↑ toxin production.
- Toxins:
- Toxin A (enterotoxin)
- Toxin B (cytotoxin, potent)
- Binary toxin (CDT) - assoc. ↑ severity.
- Clinical: Severe diarrhea, pseudomembranous colitis.
- Diagnosis: NAAT for toxin genes.
- Management (initial episode): Oral Vanco (125mg QID)/Fidaxo (200mg BID). FMT (recurrent).
⭐ > NAP1/BI/027 C. difficile: ↑ toxins A & B production → severe disease, ↑ mortality.
Gram-Negative Threats - Resistance Rampage
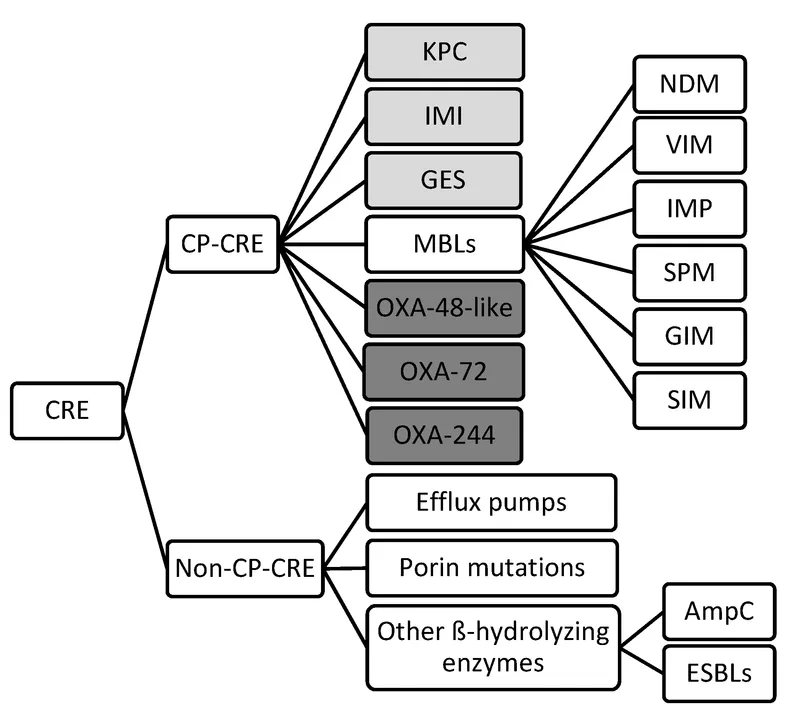
- Carbapenem-Resistant Enterobacteriaceae (CRE): Significant global health threat.
- Key Species: Klebsiella pneumoniae, E. coli.
- Mechanisms (Carbapenemases): 📌 King New Ox (KPC, NDM, OXA)
- KPC (Klebsiella pneumoniae carbapenemase): Class A Serine β-lactamase.
- NDM-1 (New Delhi metallo-β-lactamase): Class B Metallo-β-lactamase.
- OXA-48 (Oxacillinase-48 type): Class D Serine β-lactamase.
- Detection:
- Phenotypic: Modified Hodge Test (MHT), Carba NP test, mCIM (modified Carbapenem Inactivation Method).
- Genotypic: PCR for resistance genes (e.g., blaKPC, blaNDM, blaOXA-48).
- Treatment: Challenging; often requiring last-resort drugs (e.g., colistin, tigecycline) or newer agents (ceftazidime-avibactam). Associated with ↑ mortality.
- MDR Acinetobacter baumannii & P. aeruginosa: Also significant carbapenem-resistant threats, complicating treatment.
⭐ NDM-1 confers resistance to almost all β-lactams, including carbapenems, except aztreonam (variable) and newer β-lactam/β-lactamase inhibitor combinations.
Zoonotic & Vector-Borne - Ticks & Tricks
- Lyme Disease (Borrelia burgdorferi)
- Vector: Ixodes ticks (deer tick)
- Features: Stage 1: Erythema migrans (bull's-eye rash); Stage 2: Bell's palsy, AV block; Stage 3: Arthritis, encephalopathy
- Dx: Serology (ELISA, Western Blot)
- Rx: Doxycycline; Amoxicillin (<8 yrs); Ceftriaxone (severe)
- Ehrlichiosis (Ehrlichia chaffeensis - HME) & Anaplasmosis (Anaplasma phagocytophilum - HGA)
- Vectors: Ticks (Lone Star - Ehrlichia; Ixodes - Anaplasma)
- Features: Fever, myalgia, headache; Morulae in WBCs (monocytes - HME; granulocytes - HGA)
- Dx: PCR, Serology, Blood smear (morulae)
- Rx: Doxycycline
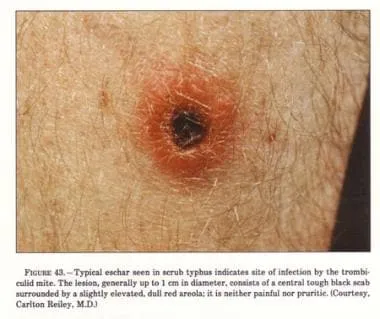
- Scrub Typhus (Orientia tsutsugamushi)
- Vector: Trombiculid mites (chiggers, larval stage)
- Features: Eschar (often pathognomonic), fever, rash. Severe: ARDS, multi-organ dysfunction
- Dx: Serology (Weil-Felix OX-K positive), IFA, PCR
- Rx: Doxycycline, Azithromycin
⭐ Orientia tsutsugamushi (Scrub Typhus) is a key cause of acute undifferentiated fever in India, frequently presenting with an eschar.
High‑Yield Points - ⚡ Biggest Takeaways
- Melioidosis, caused by Burkholderia pseudomallei, shows "safety pin" appearance on Gram stain; endemic in SE Asia.
- Capnocytophaga canimorsus from dog bites causes severe sepsis in asplenic patients.
- Elizabethkingia meningoseptica causes neonatal meningitis and is often multidrug-resistant.
- CRE (e.g., NDM-1 Klebsiella) pose a significant threat due to extensive antibiotic resistance.
- Whipple's disease (Tropheryma whipplei) presents with PAS-positive macrophages on duodenal biopsy.
- Cat Scratch Disease (Bartonella henselae) causes regional lymphadenopathy; bacillary angiomatosis in immunocompromised individuals.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

